Ambulance delays and A&E waits worst on record but waiting list falls

Ambulance response times and A&E waits are the worst on record, though the number of people on the NHS waiting list has fallen slightly, new figures show.
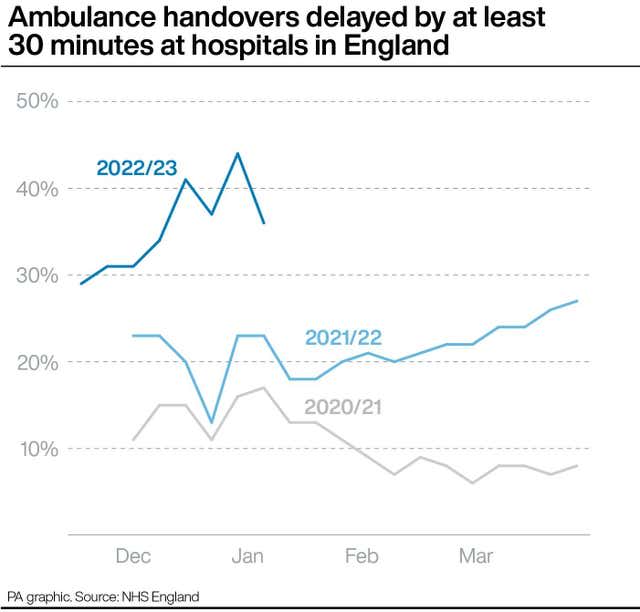
The data from NHS England shows the average response time in December for ambulances dealing with the most urgent incidents, such as cardiac arrest, was 10 minutes and 57 seconds.
This is the worst performance on record and is set against a target of seven minutes.
Ambulances in England also took an average of one hour, 32 minutes and 54 seconds in December to respond to emergency calls such as strokes, heart attacks and sepsis.
This is the longest on record and well above the target of 18 minutes.
Downing Street said the figures are “obviously unacceptable” but the Government is “very focused” on improving NHS performance.
The figures for England found a record 54,532 people waited more than 12 hours in A&E departments last month from a decision to admit to actually being admitted.
And the proportion of patients seen within four hours in England’s A&Es fell to a record low of 65% in December.
Elsewhere, the waiting list for routine treatment such as cataract operations and hip replacements has fallen slightly from a record 7.21 million people to 7.19 million.

It comes a day after up to 25,000 ambulance workers walked out on strike in a dispute with the Government over pay.
More NHS strikes are scheduled, with nurses due to walk out next Wednesday and Thursday, and another ambulance strike the week after, on January 23.
Siva Anandaciva, chief analyst at the King’s Fund, said there was “no shying away from the reality that the NHS is deep in crisis”, adding: “Since modern records began, A&E performance is the worst it has ever been and not a single NHS trust in the country is managing to meet the national target to be seen within four hours.
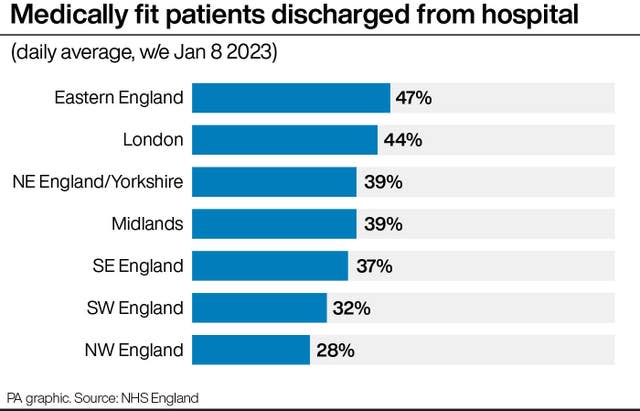
“While there are huge delays in admitting patients, there are also serious issues in discharging patients – with over 13,000 people stuck in hospital despite being medically fit to leave.
“Meanwhile, the waiting list for planned hospital care remains stubbornly over seven million and cancer services are also under pressure, which underlines the challenge in meeting the Government’s latest pledge to reduce waiting lists by the end of 2023.”
He said that while a cash injection was welcomed, the Government must think longer term and bring forward a timeline for its plan to increase the workforce.
Tim Gardner, senior policy fellow at the Health Foundation, said the data showed the “NHS is facing an emergency but the roots of this lie in political choices made over the last decade, not the cold weather or seasonal flu”.
He said 347,707 people in 2022 spent more than 12 hours in A&E waiting for a hospital bed, which is “over four times as many 12-hour trolley waits as in the previous 10 years put together.”
He added: “Waits for cancer treatment reached new highs in 2022, while the waiting list for routine operations is 7.2 million.
“Behind these numbers are patients left in pain, people enduring unnecessary suffering and, in some cases, lives tragically lost…
“The pressures on the NHS result from a decade of underinvestment in the NHS and other public services, a failure to address chronic staff shortages, raiding capital budgets and the longstanding neglect of adult social care.”
The new data shows 61% of the record 16,296 cancer patients who had their first treatment in November after an urgent referral by their GP had waited less than two months – up from 60.3% the previous month but well below the 85% target.
In better news, a record 264,391 urgent cancer referrals were made by GPs in England in November, the highest number in records going back to 2009.
The proportion of cancer patients in England who saw a specialist within two weeks of being referred urgently by their GP also increased from 77.8% in October to 78.8% in November but was still below the 93% target.
Meanwhile, 69.7% of patients urgently referred for suspected cancer were diagnosed or had cancer ruled out within 28 days in November, up from 68.5% the previous month. The target is 75% by March 2024.
Cancer Research UK chief executive Michelle Mitchell said the figures “paint an extremely troubling picture for people affected by cancer”, adding: “The last time all targets for cancer waiting times were met was as far back as 2015, and the number of people waiting for diagnosis and treatment remains unacceptably high.
“It can be easy to get lost in statistics – but each one of those numbers represents someone’s child, parent, partner, sibling or friend.”
NHS England said a record number of tests and checks were delivered by staff in November (2,172,150 – up from 2,055,449 in October), while the NHS dealt with a record number of patients attending A&E in December (2,283,196) and call handlers answered more 999 calls than ever before.
The NHS has written to trusts asking them to book in all remaining patients waiting more than 18 months for their appointment or treatment by the end of March.
NHS national medical director, Professor Sir Stephen Powis, said: “As staff responded to record A&E attendances, 999 calls and emergency ambulance callouts as the ‘twindemic’ led to unprecedented levels of respiratory illness in hospital, they also continued to deliver for patients with more people than ever before receiving diagnostic tests and cancer treatment.
“These figures show just how hard our staff are working, not only in the face of extreme pressure but also in bringing down the Covid backlogs and checking more people for cancer than ever before in one month.
“The NHS will keep its foot on the accelerator to continue to make progress on the Covid backlog and hospitals have today been asked to ensure anyone waiting longer than 18 months has their treatment booked in before March.”
He urged people to only call 999 in an emergency, to get their vaccinations and to use 111 online for non-urgent needs.
Liberal Democrat health spokeswoman Daisy Cooper said: “Thousands of excess deaths, millions on waiting lists and hours until an ambulance arrives – this is a horror show of the Government’s creation. People will be petrified when they or their loved ones fall ill.”
Shadow health secretary Wes Streeting said: “The NHS is in the biggest crisis in its history.
“The terrifying truth is that patients in an emergency can no longer be sure the NHS will be there for them.”
Royal College of Nursing (RCN) director for England, Patricia Marquis, said: “Corridor care appears to have become the norm. Some nurses are being booked to work in hospital corridors, others are being asked to buy Ikea hooks so intravenous drips can be attached to the corridor wall, and some patients are having cardiac arrests because of mistakes made using cumbersome oxygen cylinders to treat them.”

 Yahoo News
Yahoo News 
