Beware super-gonorrhoea: the gift nobody wants at Christmas
As the Christmas party season comes upon us, too much alcohol and too few inhibitions may lead to an unwanted gift in the form of a sexually transmitted infection (STI).
Young people are particularly at risk of both being given and regifting this particular festive favourite, with figures from Public Health England showing that in 2017 an STI was diagnosed in a young person once every four minutes, with those aged between 15 and 24 disproportionately affected.
Today’s climate – where more liberal attitudes prevail and a willing sexual partner is available with a swipe right on a dating app – provides a perfect breeding ground for STIs at any time of the year.
And while most of us have heard of things like herpes and chlamydia there are new, mutating and re-emerging STIs that everyone needs to know about to ensure that no surprise presents get unwrapped on Christmas day.
Gonorrhoea
Gonorrhoea was a disease that many sexual health experts thought had gone away. But in recent years the number of cases has skyrocketed: in 2017 there were just over 44,000 cases, an increase of 22 per cent compared to the previous year.
Gonorrhoea is a nasty infection – it is often symptomless but it can cause an unpleasant, watery, green discharge from the penis or vagina, a pain or burning sensation when passing urine among both men and women, as well as bleeding between periods and after sex for women.
But what really worries health experts is the drug-resistant form of the disease, a growing threat around the world. In April the UK reported the world’s “worst ever” case of “super-gonorrhoea” picked up by a British man on holiday in Bali.
In this case the the two front-line treatments proved ineffective and the patient ended up having to be admitted to hospital and given a three-day infusion of antibiotics.

Despite fears of the bug spreading authorities appear to have caught it in time although a couple of cases of the same bug were also reported in Australia.
Mark Lawton, a consultant in sexual health in Liverpool and spokesman for the British Association of Sexual Health and HIV (BASHH), says the spread of untreatable STIs is a real threat.
“This is not just about sensationalist headlines about super gonorrhoea. It’s a real concern among doctors,” he says.
If this resistant bug is circulating in south east Asia, a popular gap-year destination, more cases will be sure to crop up.
“We need to be ready for the next wave of resistance. We’ve seen one case and it will only be a matter of time before we see more,” says Dr Lawton.
Gonorrhoea can occur throughout the body, including the throat, joints (leading to arthritis) and even the eyes. And this is one reason for it developing resistance, says Dr Lawton.
“If you get it in the back of the throat the gonorrhoea can acquire resistance from other bacteria in the back of the throat and swap genetic material,” he says.
And while it won’t cause problems with fertility it can still be passed to other people, says Joe Petersen-Camp, a sexual health doctor at the Homerton Hospital in east London.
“Most women with gonorrhoea in their throat will also have it in their vagina so it’s easily transmissible through unprotected sex,” he says.
Mycoplasium genitalium
Known as the fastest growing STI you’ve never heard of Mycoplasium genitalium – known as M.gen – is the new STI on the block.
The disease is often symptomless but in women it can cause a burning sensation when passing urine and pain or bleeding during and after sex. If left untreated it can also lead to infertility in women. In men symptoms include include watery discharge from the penis. Around one to two per cent of men and women are thought to be infected with the disease, although rates in some STI clinics are as high as 38 per cent.
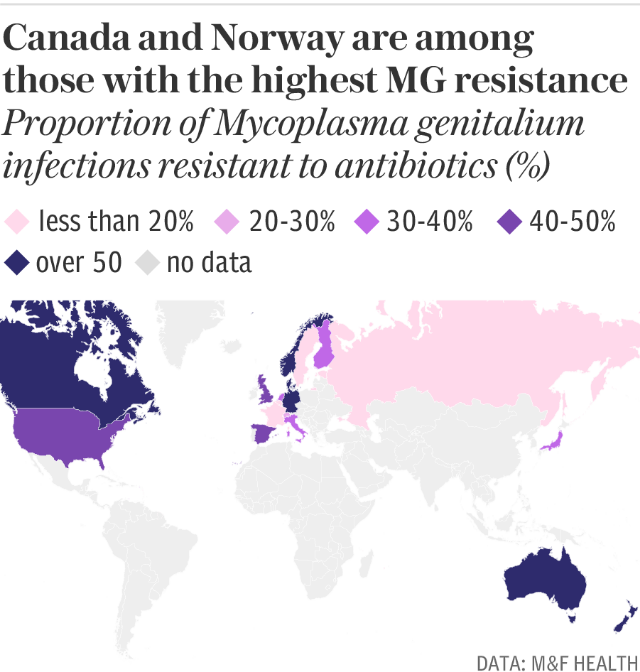
In the UK around 40 to 50 per cent of cases of M. gen, first identified in the 1980s, are thought to be resistant to treatment and resistance is spreading around the world, with high rates in Australia and holiday destinations in Europe, such as Spain and Italy.
Earlier this year, the National Institute for Health and Clinical Excellence introduced new guidelines for the treatment of M. gen, recommending the use of a specific diagnostic test.
Suneeta Soni, a sexual health consultant in Brighton and spokesperson for BASHH, says that the lack of specific testing for the disease has driven up rates of resistance.
“If you can’t test for an organism you end up treating what you think it might be. You end up giving an antibiotic and hoping for the best and this is what we have been doing for the past 15 to 20 years,” she says.
Doctors have been treating it as if it were chlamydia but not prescribing a high enough dose of antibiotics. Dr Soni had to order a specialist antibiotic from France to treat one patient.
“The patient came back multiple times before we realised what was going on. It was more more expensive than standard antibiotics and it was a pain to get hold of. We’re just not used to dealing with this infection,” she says.
Syphilis
Rates of syphilis – another STI assumed to have been consigned to history are also growing alarmingly. There were more than 7,000 diagnoses of the disease reported in 2017, compared to around 2,600 in 2010.
In south Wales, there was a spike in the number of cases over the summer with 56 cases between April and August, compared to 11 in the same period last year.
Syphilis is a complex infection. Initially patients may find a small sore on the penis, vagina or anus. This will pass and, if left untreated, will progress to a second stage when a blotchy red rash appears on the body, usually on the soles of the hands and feet.

Without treatment this can progress to tertiary syphilis which can spread to the brain or nerves, leading to blindness, strokes, heart problems and memory loss.
Syphilis is treatable with penicillin although those with the more advanced stage of the disease have to undergo a daily injection in the buttocks every two weeks.
Martin Godfrey, a GP in south London, says: “I have seen patients in their 60s who have heart complaints and discovered that it was syphilis they picked up years ago.
"One patient came to me who had never been unfaithful to his wife. He realised that when he was in the army he had had an encounter which led to a nasty sore. It went away but then reappeared years later. “
But people can also go for a long time without symptoms which may go some way to explain why it has risen stealthily in recent years, says Dr Petersen-Camp.
“That’s why it’s important to have regular screening. People who are having sex with more than one person should have a check up every three months,” he says.
Shigella
In 2016 PHE began warning gay men of a diarrhoeal disease called shigella, a type of dysentery which usually occurs in countries where there is poor sanitation.
Nick Thomson, professor of microbiology at the Wellcome Sanger Institute in Cambridge, and an expert in the genetic sequencing of STIs, said public health experts noticed that more men than women were falling ill with this very unpleasant stomach bug.
“We know that dysentery doesn’t target men, but the rise in the number of cases was through men who have sex with men. When it was researched further it turned out you can catch this, fairly unsurprisingly, through oral anal sex,” he says.

This infection was resistant to a class of antibiotic called macrolides, says Prof Thomson.
“The reason for this is because the MSM group are a high risk group for gonorrhoea and chlamydia and you use macrolides to treat those, even if you don’t use them to treat diarrhoea,” he says.
While this was a rare event in a particular group of the population it is an example of the way STIs change and evade detection, says Prof Thomson.
“People aren’t as cautious about HIV as they used to be and we have apps on our phones to find people. The rules are changing but one thing that doesn’t change is that bacteria are very good at spreading, given the right opportunities. So if we change our behaviour there will always be a bacteria or infection that profits from that change,” he says.

Protect yourself and your family by learning more about Global Health Security

 Yahoo News
Yahoo News 
