California Was a COVID Success. Here’s Why It’s Veering Back to Lockdown.

Weeks before Gov. Gavin Newsom’s announcement Monday that California would dramatically reverse its reopening, a doctor 2,500 miles away saw a new COVID-19 crisis emerging there.
It began ahead of Memorial Day, as clusters erupted in the deserts of Imperial County, down along the Mexican border. Driven north with increasing commercial activity and seasonal travel, as the state reopened and summer began, the disease tore through nursing homes in Tulare, Modesto, and Fresno counties as May bled into June.
Los Angeles, meanwhile, had its own flare-up that never quite cooled down.
For a time, it seemed that the Bay Area and the northern precincts of the state would prove immune to the resurgence, perhaps thanks to heavy mask usage and cool temperatures that kept people from huddling into the air-conditioned indoors. But finally, the outbreaks on their edges—possibly fueled by relaxed attitudes around social gatherings—overwhelmed them too, and sent their curves spiking upward.
“California is the epicenter,” said Dr. David Rubin, who watched the data come in from his post as director of PolicyLab, a research facility at the Children’s Hospital of Philadelphia that feeds data into the White House Coronavirus Task Force. “I would add them to the list with Texas, Arizona, and Florida.”
‘They Put Us in Here to Let Us Die’: ICE Prison Sees Outbreak of Coronavirus—and Guard Violence
But unlike those other states, California is famed for its progressive and technocratic policies, and in particular for its first-in-the-nation shutdown. Newsom’s order on Monday again ended indoor dining, closed bars, shuttered zoos and museums, and obligated most counties to revert to the earliest stages of the reopening process.
What went wrong?
According to Rubin, many leaders in the state saw only the spare capacity in their emergency rooms and intensive care units, and overlooked a crucial underlying factor: the virus’s growing transmissibility rate. Often referred to by experts as its reproductive value, or R0, it reflects how easily and how often an illness is spreading. This number oscillated up or down on a daily basis across counties in California. But the trend—“the signal,” as Rubin puts it—was unmistakable.
Prior to Newsom’s order, PolicyLab was predicting a fresh outbreak in San Francisco, according to models shared with The Daily Beast. The graphs include projections of transmissibility rates, and models of case counts expected under various phases of reopening—three in all, along with a shelter-in-place scenario, and the latest real-life trajectory. Last week, Dr. Rubin and his colleagues passed their findings—along with information and modeling for counties nationwide—to the Task Force, which incorporates the data into its tailored recommendations to governors.
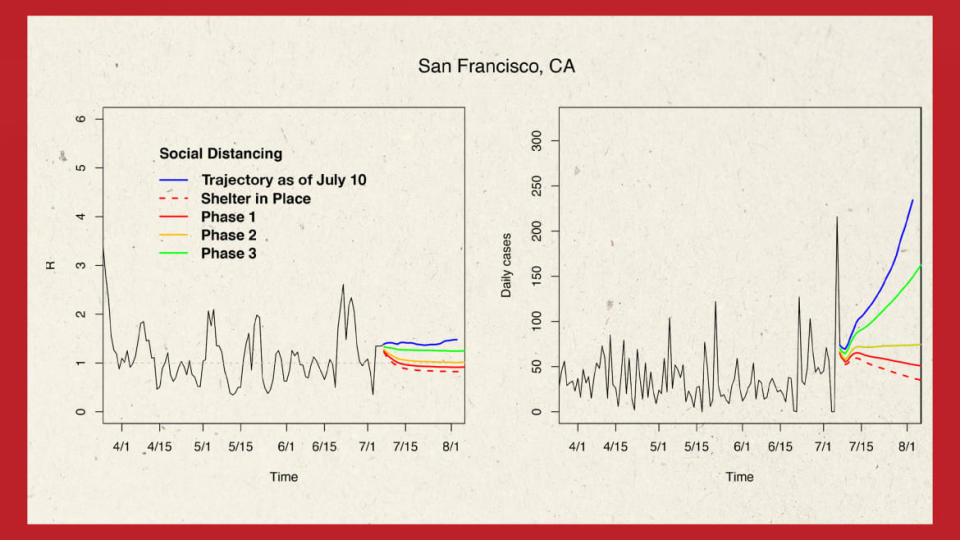
“I think [California] pushed through their reopening even as they had evidence that their transmission rate was increasing,” Rubin said, arguing that the sporadic outbreaks across the state illustrated the growing threat. “People look for that visual cue that says, ‘Hey, we better do something.’ But it’s already too late. It's like waiting for the stock market to crash before selling your stock.”
In an interview with The Daily Beast, Newsom’s Health & Human Services Secretary Dr. Mark Ghaly defended the administration’s handling of the outbreak. He highlighted California’s strong performance early on, and asserted his office had tracked the virus’s transmissibility rate—along with hospitalizations, and reports from industries and localities. Relying on county input, he argued, was necessary in a state as vast as California.
“We saw a trajectory of spread that made California leaders comfortable with reopening,” he said. “I feel very strongly that California has a plan that includes the description the governor uses, the dimmer switch. We always knew we would go up and down with our interventions.”
But while epidemiologists in the Golden State diverged from Rubin’s analysis, they shared a conviction that the state’s caseload had veered horribly off course—and that it will take tremendous efforts to rectify.
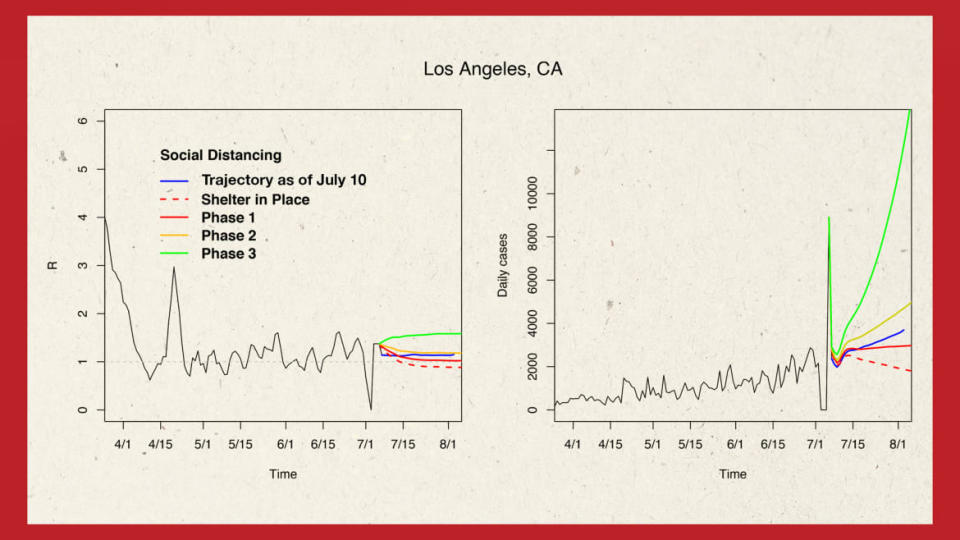
Researchers at the University of Southern California’s Keck School of Medicine have for months monitored and modeled COVID-19 spread in Los Angeles—a city that Mayor Eric Garcetti this week warned may need to shut down again entirely.
A month and a half ago, Garcetti was announcing the sprawling metropolis would enter stage three of its reopening, allowing restaurants, beauty parlors, and houses of worship to return to some level of normal function, and offices to resume business where telework was impossible. The result, as the team at USC observed, was an uptick in cases and transmission rates, which have only continued to rise.
In an interview, USC’s Dr. Abigail Horn pointed out that, although L.A. entered its initial lockdown at roughly the same time as New York City, the California city was at a far earlier stage of the pandemic. That, combined with lower density and other factors, likely accounted for the City of Angels suffering a far lower death toll than NYC in the outbreak’s early months.
She also pointed out even though the city managed to flatten its curve, it didn’t ever manage to actually drive it down.
“The worrisome thing is we weren’t decreasing our cases yet. Infections as a whole were never decreasing. We did open in that context,” Horn said, adding that the USC scientists noticed increasing mobility and contacts between L.A. residents. “We predicted that cases would go up. That was inevitable. The question was, ‘How much?’”
But even with that question hanging, Horn’s colleague Dr. David Conti defended the city and state’s decisions to move forward with reopening. The reason the reprise of the disease proved so severe, he argued, was not public policy but public behavior—including the failure to wear masks, practice proper hygiene, and obey social distancing guidelines.
“From a public health perspective, I think it was fine to reopen. The problem is how people react,” said Conti, who called for intensifying government messaging so as to achieve more uniform compliance. “So long as there are cases out there, there is potential for a spike. The question is how people behave.”
Four hundred miles away, at the University of California, San Francisco, Dr. George Rutherford saw a very different problem.
He admitted the recent upswing in cases in the Bay Area likely owed to celebrations before and during the Fourth of July weekend. Nonetheless, he argued the COVID-19 surge was less a consequence of personal choices, and more of the personal obligations imposed on essential workers—particularly those in the state’s Hispanic communities.
“Everybody has in mind some guy in board shorts and a t-shirt hanging out in Huntington Beach. That's not where the infection is,” he said, citing a recent paper researchers at his school published on testing in San Francisco’s Mission District. “This is an endemic disease in the Latino community in California.”
DeSantis Says Florida Has a COVID-19 ‘Blip.’ Nurses Say It’s Far Worse.
This goes beyond the national trend of COVID-19 hitting communities of color far harder than their share of the population, and—according to Rutherford—has to do with California Latinos’ overrepresentation among essential workers, and their often crowded living conditions.
Thus, he sees the failure to contain the disease as stemming from leaders’ unwillingness or inability to implement a massive social services intervention that would allow infected essential workers to self-isolate outside their homes while simultaneously providing for their families.
Worsening the overall picture for the state and the region, Rutherford added, was the California Department of Corrections’ decision to move 121 untested inmates from the Institute for Men at Chino into San Quentin State Prison. More than a thousand people at the latter facility have now contracted the virus.
But, overall, Rutherford faulted the Newsom administration’s policies less than local authorities who lobbied the state for waivers in order to prematurely expedite their reopening.
“I think clearly some places moved too soon, and the governor set up this process to walk it back,” he said.
For his part, Ghaly, the state Health and Human Services Secretary, noted that, for all the waivers the state granted, it never extended one to Imperial County, the site of some of the worst flare-ups. He added that the state prison network’s health system is in the hands of a court-appointed federal receiver, and insisted that the quality of care at San Quentin has steadily improved.
“It’s all part of our ongoing, evolving response,” said Ghaly. “These are absolutely important parts that we continue to build on in California. We have done a lot already, but there’s more to do.”
The independent epidemiologists The Daily Beast consulted agreed that the trajectory of the outbreak would vary tremendously by region. And Rubin and Rutherford argued that, with Newsom’s order and continued observation of masking and social distancing norms, the Bay Area might be able to quickly reverse its latest surge. The situation in Southern California, however, appears more intractable.
All the doctors agreed that the state needs consistent and concerted outreach at every level of government, however much their visions of that intervention might differ.
As for what the unfortunate example of California could teach the nation, Rubin noted that transmission rates have ticked up again recently in some of the most battered regions of the United States: New York, New Jersey, and Pennsylvania. To avoid a complete relapse like the one on the West Coast, he recommended the states act quickly and brake their reopening process before fall.
“I see the same patterns emerging,” he warned. “If you’re waiting for some obvious signal in two to three weeks, it’s already too late.”
Get our top stories in your inbox every day. Sign up now!
Daily Beast Membership: Beast Inside goes deeper on the stories that matter to you. Learn more.

 Yahoo News
Yahoo News 
