Coronavirus patients on ventilators are unusually likely to die, causing some doctors to change strategy
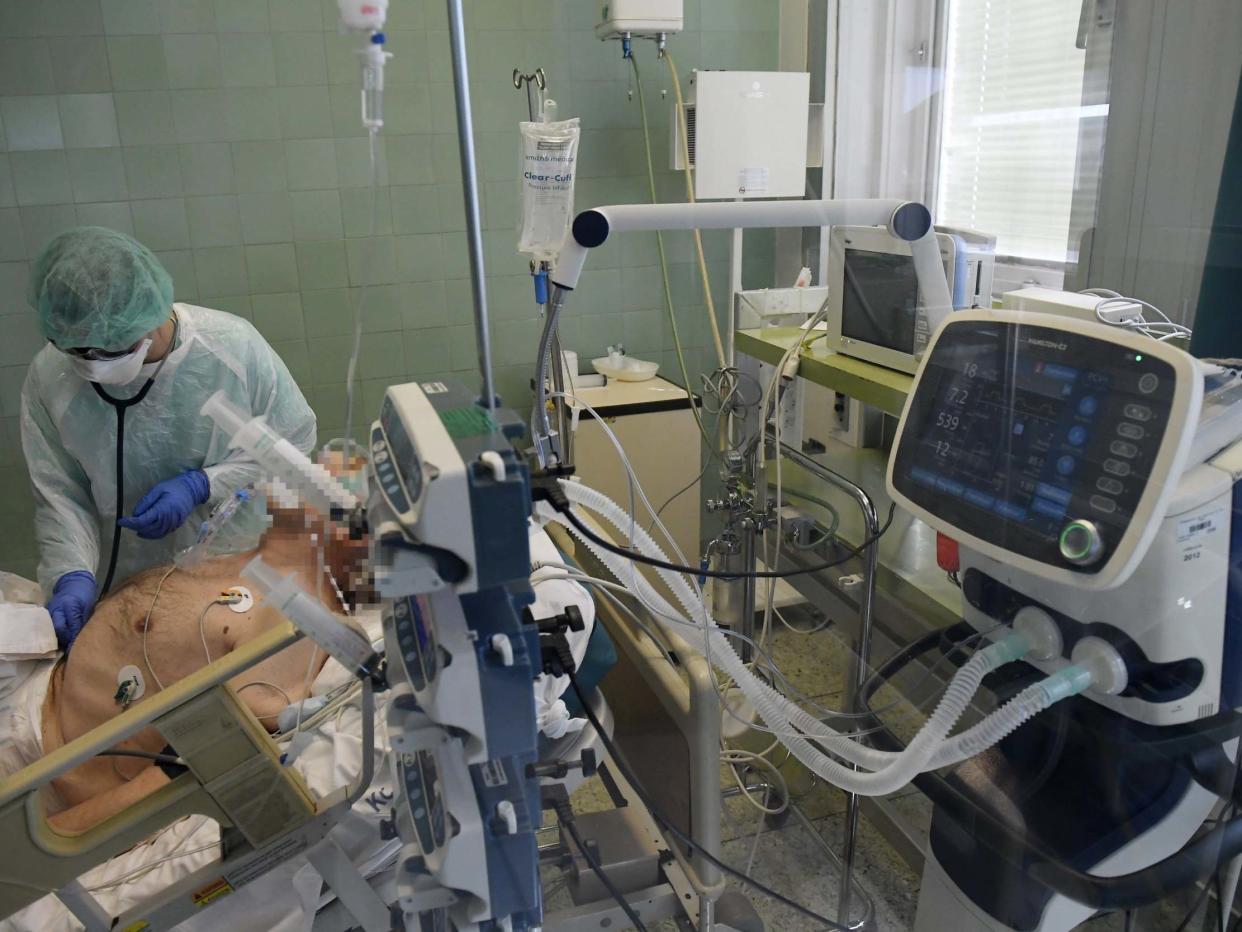
Ventilators are being sourced and stockpiled across the world — but some working on the front lines of the coronavirus epidemic are now wondering whether they might do more harm than expected.
A recent report from the NHS shows that over 67 per cent of coronavirus patients put on ventilators go on to die. Normally, around 40 per cent of patients would be expected to die while receiving mechanical ventilation.
This unusually high death rate has also been shown in the US: on Wednesday morning, the Associated Press reported that around 80 per cent of coronavirus patients put on ventilators in New York go on to die, according to state and city officials.
A small study from Wuhan also showed that out of 37 people treated with mechanical ventilation, only seven survived.
The numbers are alarming enough that some physicians in the US are now trying to keep their patients away from ventilators for as long as possible.
"If we're able to make them better without intubating them, they are more likely to have a better outcome — we think," Dr Joseph Habboushe, an emergency physician working on coronavirus wards in New York, told Time magazine Wednesday.
In an letter to the editor published in Intensive Care Medicine, Dr Luciano Gattinoni, an expert in anaesthesiology and intensive care at the Medical University of Gottingen, wrote that coronavirus patients in Italy showed symptoms subtly but significantly different from those of other patients in respiratory distress. So far, doctors have been following standard protocols for Acute Respiratory Distress Syndrome (ARDS) as their guide on how to treat coronavirus patients, he notes, but those protocols may be doing damage.
Ventilators force oxygen into the lungs via a tube down the throat while a patient is heavily sedated. Pressure and volume of oxygen, as well as oscillation, can be varied according to need. It may be that standard high-pressure ventilation that works well in patients with ARDS is not well tolerated by people whose lungs have been damaged by coronavirus. Forcing air into the lungs at such high pressures may cause further inflammation or irritate an immune system already in hyperdrive.
“We need to be patient,” Gattinoni wrote, noting that aggressive, high-pressure ventilation could lead to bad outcomes in coronavirus-caused pneumonia, where lung damage presents differently to how it might with other types of pneumonia.
“All we can do ventilating these patients is ‘buying time’ with minimal additional damage: the lowest possible PEEP [Positive End Expiratory Pressure] and gentle ventilation,” Gattinoni added.
An emergency physician working on the front lines of the coronavirus pandemic in the NHS told The Independent: “Initially we assumed this illness was very similar to ARDS, so we have been using ventilator strategies which are standard in ARDS, but in recent days there are lots of suggestions that the similarities are not as strong as initially thought.”
“To argue that using any ventilator at all is worse than using no ventilator, you need to know what would happen to the patient without a ventilator,” the physician added. “Nobody would get ethical approval to randomise people to ‘ventilator or no ventilator’ [in a trial], therefore we cannot prove what the difference would be. But the expert consensus would be, basically everybody who goes onto a ventilator does so because their lungs are doing so badly at oxygenation they are about to die. People would argue — without proof — that, of all the people who need a ventilator, if you didn’t put them on one, mortality would be close to 100 per cent. So from there you can’t argue that 60 to 80 per cent [as has been reported in coronavirus patients] is worse.”
"Current anecdotal evidence is that obesity is really important," the doctor continued. "We are seeing loads of obese people becoming extremely unwell, especially men aged 55 to 70. It's unclear exactly why that's happening."
A retired NHS doctor who specialised in lung disease told The Independent that successful ventilation often depends on “the skill of the operator of the ventilator”, meaning that those who have never specialised in ventilation but have been called on to help in Covid-19 wards could be unwittingly harming coronavirus patients through their lack of expertise.
The former specialist, who is one of many previously retired doctors who has been asked to return to the NHS due to excessive need, added that normal intensive care units also do not have the right “calibre of pipe” required to deliver as much oxygen as is currently needed for those suffering from Covid-19 and so ventilation may be less effective in those settings. Usually, such wards would have far fewer patients requiring ventilation. Additionally, coronavirus patients who receive mechanical ventilation stay ventilated for much longer than most other pneumonia patients.
“In the purpose-built hospitals, like the Nightingale Hospital, they may have those wide diameter pipes needed to deliver that amount of oxygen,” the expert added. “But in other hospitals, it’s not usual.”
According to the BMJ, two thirds of patients in the UK with coronavirus who require critical care receive mechanical ventilation within 24 hours of admission.
Read more
Hospitals fear shortage of vital drugs will make ventilators useless
Lives could be at risk from new NHS ventilators, warn experts
Tesla ventilators won’t arrive before coronavirus apex, Cuomo says

 Yahoo News
Yahoo News 
