Physiotherapist's 'bad hangover' turned out to be a rare condition that left her paralysed

A physiotherapist has revealed how her “bad hangover” turned out to be a rare condition that left her paralysed and unable to speak.
Rachael Bailey, 25, was on a night out during freshers’ week in October 2014 when she developed a tingling sensation in her legs.
The following day, the then 19-year-old woke up unable to move her lower body.
Read more: Man paralysed after developing rare disorder mistaken for the flu
After calling the NHS non-emergency number 111, Bailey was airlifted to the Queen’s Medical Centre in Nottingham, where she was diagnosed with the one in 100,000 neurological condition Guillain-Barré syndrome.
Within three days she was on a ventilator and eventually put into a medically-induced coma.
After 59 days in critical care and 76 days of rehabilitation, Bailey walked out of hospital that September.
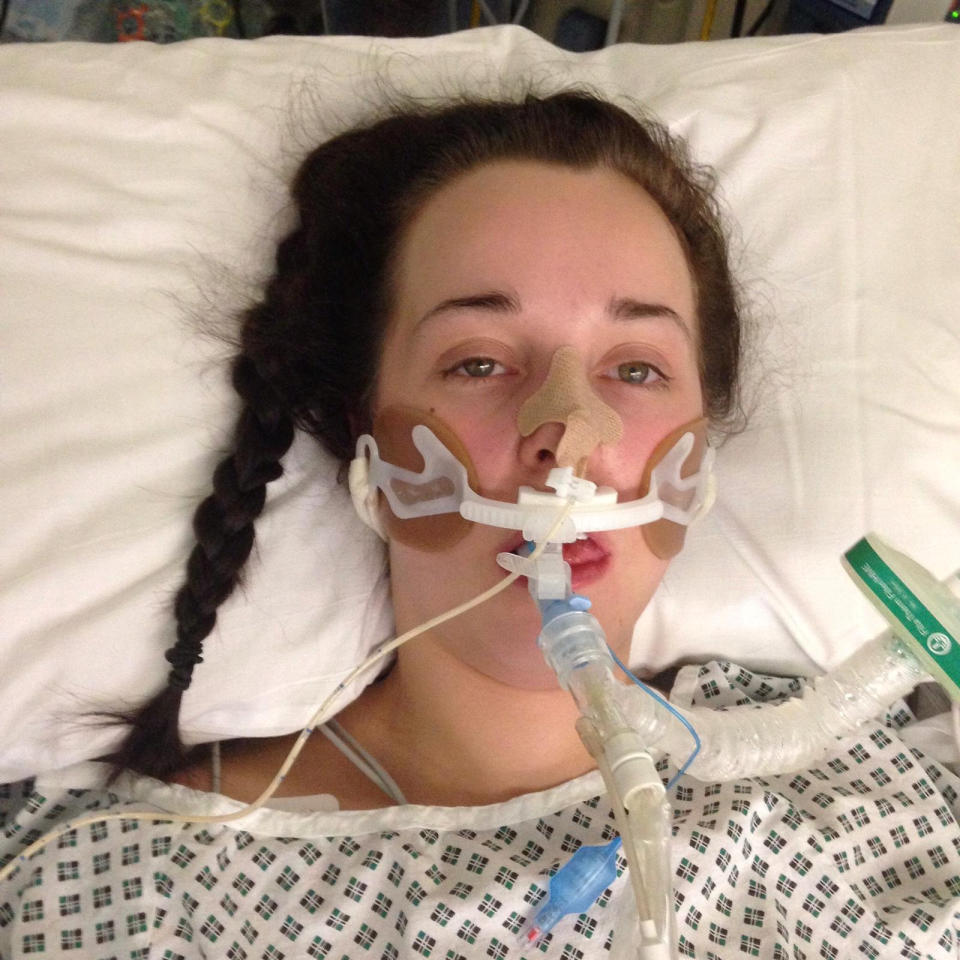
‘I was paralysed from head to toe’
After developing tingling in her legs, Bailey initially blamed it on her shoes.
“I'd been dancing that evening and thought it was just my new high heels,” she said. “The next morning it got so much worse and I had to crawl out of bed.”
Once in hospital, Bailey did not think much of her diagnosis at first.
“I was calm because I thought I was young and physically fit and I’d be home by the weekend,” she said.
“I ended up spending nearly half of the year in hospital with tubes in my mouth, being spoon-fed and moving in a wheelchair.”
When Bailey came round from the coma, she was barely able to move.
Read more: Bachelorette star can’t hold his kids after Guillain Barré diagnosis
“It was terrifying because I was paralysed from my head to my toe and I could only move some of my face,” she said.
“I couldn’t speak, I couldn’t move, I couldn’t scream.”
Bailey was transferred to Nottingham City Hospital on 11 November, her 20th birthday, where a team of 50 rehabilitation specialists helped her get back on her feet.
“The rehab was very intense,” she said. “For the first three weeks I hated everyone; I hated my situation and everyone around me.
“I cried every time I had to see a physiotherapist because it reminded me of everything.
“I was in denial of how hard the recovery was going to be, but the physios were amazing and helped me throughout.”
Bailey’s mobility started to return after three months.

‘I’d never felt pain like I did back then’
Bailey had planned to return to Liverpool John Moores University where she was studying criminology and psychology.
She decided to switch to physiotherapy at the University of Nottingham after being inspired by the team that helped her.
In June, Bailey earned a first class degree – tutored by one of the physiotherapists who cared for her – and is due to start working at London’s Royal Brompton Hospital in two weeks.
Read more: Cowboys player Travis Frederick diagnosed with Guillain-Barré syndrome
“When I first woke up in hospital it was the worst thing I’d ever been through,” she said.
“The first year was a nightmare, I hated every moment of it. Everything I had planned turned upside down and I felt lost.
“I’d never felt anger or pain like I did back then, but it’s given me a new purpose in life.
“I didn’t know much about physios, I thought they just helped footballers and massaged people, but they were like heroes and magicians.”
What is Guillain-Barré syndrome?
Guillain-Barré syndrome is a serious condition that affects the nerves, mainly in the feet, hands and limbs.
Symptoms include pain, numbness, muscle weakness, pins and needles, and a loss of balance or co-ordination.
In severe cases, patients struggle to swallow, walk or even breathe.
Symptoms may worsen over several days or weeks, before gradually improving.
Although unclear, Guillain-Barré syndrome is thought to come about when the immune system mistakenly attacks the body’s nerves. This can occur after an infection, like flu or food poisoning.
Most patients are treated in hospital via IV immunoglobulin; a therapy made from donated blood that helps bring the immune system under control.
Alternatively, plasma exchange filters the blood to remove the harmful substances that are attacking the nerves.
Some patients require breathing or feeding tubes, as well as pain relief.
The majority make a full recovery, however, one in five endure long term problems. These may include being unable to walk without assistance, weakness, balance issues or extreme fatigue.
Physio, occupational and speech therapy can help.
One in 20 cases are fatal due to blood clots or breathing difficulties.

 Yahoo News
Yahoo News 

