High levels of coronavirus cases and deaths ‘could last until spring’
There could be “high levels” of Covid cases, demand on health care and deaths until next spring, an expert has said.
Professor Neil Ferguson, the scientist whose modelling prompted the UK-wide lockdown in March, told the PA news agency that measures in Tier 2 and Tier 3 areas are “unlikely to cause daily cases and deaths to fall rapidly”.
He said modelling suggests this could leave the country with high caseloads for several months.
A former chief scientific adviser to the Government said the number of people in hospital with Covid-19 could more than double within weeks.
Professor Sir Mark Walport said it is “not unrealistic” to say there could be 25,000 people in hospital by the end of November.
It comes as pressure mounts on medical staff, with more than 9,000 patients in hospital with Covid-19. The number in the North West of England is nearly back to where it was at the peak of the first wave.
The Nightingale hospital in Manchester will start receiving patients who do not have Covid-19 from Wednesday, the NHS said.
Prof Ferguson, from Imperial College London, told PA: “The concern at the moment is that even if the measures adopted in Tier 2 and Tier 3 areas slow spread in the next few weeks, they are unlikely to cause daily cases and deaths to fall rapidly.
“Modelling from all the academic groups informing Sage suggests that this could leave the country with high levels of Covid circulation, healthcare demand and mortality for several months, at least until spring 2021.”

Sir Mark, a member of the Government’s Scientific Advisory Group for Emergencies (Sage), told BBC Radio 4’s Today programme the UK is “still relatively early in the second wave”, but added: “The number of cases is rising very significantly – it was 22,800 on October 27 and the seven-day average was just over 22,000. So there are an awful lot of cases.
“One of the differences of course is that we are better at looking after people with coronavirus now.
“And so hopefully the case fatality rate will be lower than it was in the first wave. But at the end of the day, the fatality rate, the number of people who die, is a product of the number of people who are infected and their vulnerability.”
Asked about the possibility of 25,000 people being in hospital by the end of November, he said: “It’s certainly not unrealistic to think about that.”
The comments come as some hospitals announced measures to cope with additional pressures from the virus.
Nightingale hospitals in northern England were put on standby earlier this month as a result of rising cases.
A spokesperson for the NHS in the North West said: “The NHS Nightingale Hospital North West will accept patients from today to provide care for those who do not have Covid-19, but do need further support before they are able to go home, such as therapy and social care assessments.”
In Leeds, health officials said only essential operations will go ahead at hospitals in the city after the number of Covid-19 patients passed the totals treated at the peak of the first wave.
Leeds Teaching Hospitals NHS Trust – which runs Leeds General Infirmary and St James’s Hospital – said it was postponing some planned operations due to pressures.
We have 263 patients in our beds who have tested positive for COVID-19, including 22 in intensive care. This means we have more COVID-19 patients in our hospitals than at the peak of the pandemic in mid-April. Please read and share this important update: https://t.co/yBttbcOUjj pic.twitter.com/2VsV755gnn
— Leeds Teaching Hospitals (@LeedsHospitals) October 27, 2020
Four cancer operations were cancelled in Nottingham on Tuesday, the Independent reported.
Nottingham University Hospitals Trust said pressure on intensive care units from Covid-19 and non-Covid related emergencies meant it needed to postpone the procedures.
Airedale Hospital, near Keighley, West Yorkshire, said it is suspending non-urgent surgery for two weeks.
It said in a statement: “We are seeing increasing demand on the hospital which is in turn meaning that our inpatient beds are at capacity.
“As a result, and as per our escalation plans, we have taken the decision to postpone any elective surgery that needs an overnight stay. This comes into effect immediately for the next two weeks.”
We are seeing a high demand for our hospital services & our inpatient beds are at capacity. We are therefore postponing any operations that need an overnight stay apart from urgent and cancer surgery. We do apologise to everyone affected by this https://t.co/09jb3SxTIb
— Airedale Hospital (@AiredaleNHSFT) October 28, 2020
Hospitals in Northern Ireland are treating more people with Covid-19 than during the first peak of the pandemic.
According to official statistics there were 360 inpatients – the highest in the first wave was 322 on April 8.
Overall in England there are 7,454 people in hospital with Covid-19.
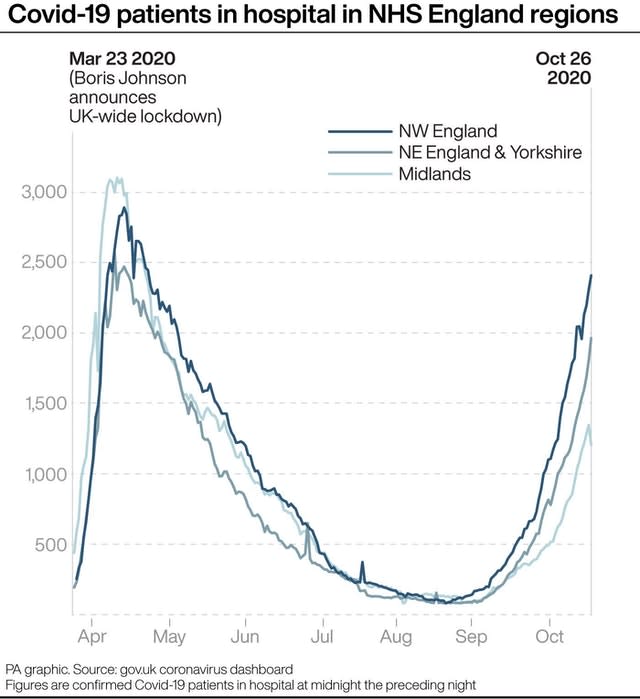
The number of in north-west England, as of October 26, stood at 2,407 – the highest since April 23, and not far below the peak of the first wave, which was 2,890 on April 13.
In north-east England and Yorkshire, the latest total is 1,962. This is the highest since April 28, and is also close to the first wave peak of 2,567 on April ).
By contrast, in the Midlands the total on October 26 stood at 1,203 – less than half the peak of the first wave – 3,101 on April 10.
The October 26 data show there were 1,052 people in hospital beds in Scotland with Covid-19 and 654 in Wales.
Dr Susan Crossland, president of the Society for Acute Medicine, told PA: “There are real concerns that the NHS is starting to struggle across the country now and that is worrying considering the workforce has not really recovered from the first peak earlier in the year.
“We now see Covid rotas coming into play which means redeployment for some staff – especially juniors – and more intense working arrangements for senior clinicians which will increase pressure greatly on those already stressed.”

 Yahoo News
Yahoo News 
