NHS crisis: A&E chiefs from 68 hospitals warn patients are 'dying in hospital corridors' amid 'intolerable' safety risks

The heads of more than 60 Accident & Emergency units have written to the Prime Minister warning that patients are "dying prematurely" amid "intolerable" safety risks.
It came as official figures show Accident and Emergency performance at major units is the worst on record, with fears the situation will worsen amid rising cases of norovirus and flu.
The letter from the most senior doctors at A&E units across the country said the health service is "chronically underfunded" and ill-prepared for winter.
They said more than 50 patients at a time had been left waiting for beds in casualty units, with 120 patients a day being managed in corridors, "some dying prematurely".
The letter, reported by the Health Service Journal, told the prime minister that shortages of beds and staff meant patients were being put at higher risk of death.

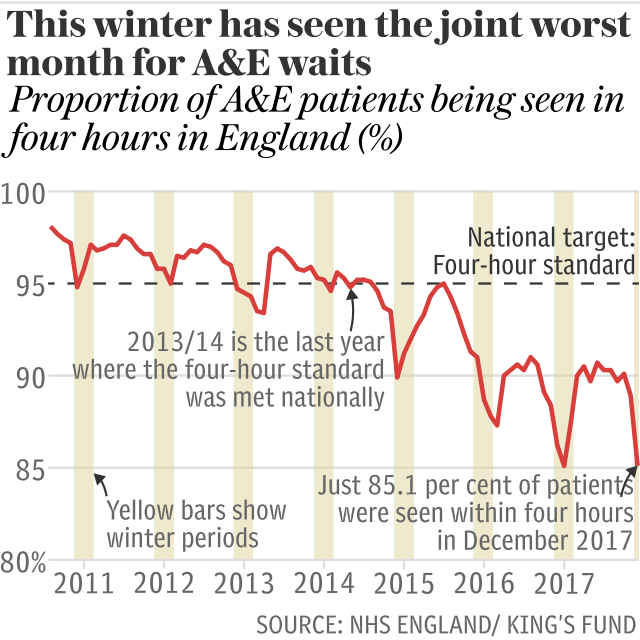
Monthly figures from NHS England show just 77.3 per cent of patients treated at major units - known as type 1 A&Es - were seen within four hours - against a target of 95 per cent.
This is the worst performance since records began - below the previous low of 77.6 per cent recorded in January 2017 and the 79.3 per cent seen in December 2016.
The worst performance was at Blackpool Teaching Hospitals Foundation Trust, with just 40 per cent of patients seen within four hours last month, the figures show.
At Hillingdon Hospitals Foundation Trust and Royal Cornwall Hospitals Trust the figure was just 58 per cent, with 59 per cent recorded at London North West Healthcare Trust and University Hospitals Of North Midlands Trust.

Across all A&E units, performance was 85.1 per cent, the same as last January, which was the worst on record.
Just three out of 134 NHS trusts hit the 95 per cent A&E target, with just two trusts with major units achieving it, the figures show.
The latest statistics from NHS England show crowding on hospital wards is continuing to worsen, while levels of norovirus have risen by almost one third in a week.
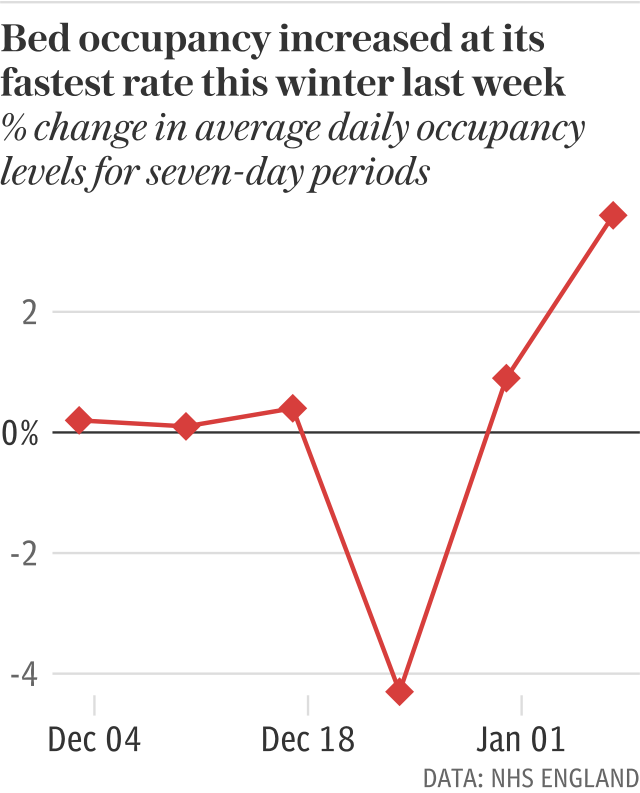
Bed occupancy levels, which dropped over Christmas, are now back up to 95 per cent, the figures show.
The weekly figures show 16,690 ambulance handover delays in the week ending 7 January - including 5,082 waits of at least an hour.
In total, 944 beds were closed because of winter vomiting and norovirus, compared with 731 the week before - a rise of 29 per cent.
Latest figures show hospitalisations because of flu almost tripled the previous week, with new figures due to be published later today. One in four cases in hospital has the strain dubbed "Aussie flu".
The new statistics show hospital occupancy rates have now reached 95 per cent - a rise from 91.7 per cent in one week.
In the letter to the Prime Minister, the clinical leads from 68 A&E units apologise to patients for putting safety at risk, as they demand a major cash injection.
As well as calling for "a significant increase in Social Care Funding to allow patients who are fit to be discharged from acute beds to be cared for in the community" they call for a review of hospital beds, which have been reduced in recent decades.
"In the meantime we would like to apologise to our patients for being unable to fulfil our pledge for a safe efficient service and acknowledge the hard work and dedication of the staff," the letter states.
In the letter to the Prime Minister, the clinical leads from 62 A&E units state: "We feel compelled to speak out in support of our hardworking and dedicated nursing, medical and allied health professional colleagues and for the very serious concerns we have for the safety of our patients.
"This current level of safety compromise is at times intolerable, despite the best efforts of staff.
"It has been stated that the NHS was better prepared for this winter than ever before. There is no question that a huge amount of effort and energy has been spent both locally and nationally on drawing up plans for coping with NHS winter pressures. Our experience at the front line is that these plans have failed to deliver anywhere near what was needed. "
Acknowledging efforts across the NHS to tackle the pressures, it continues: "The facts remain however that the NHS is severely and chronically underfunded. We have insufficient hospital and community beds and staff of all disciplines especially at the front door to cope with our ageing population’s health needs.
"As you will know a number of scientific publications have shown that crowded Emergency Departments are dangerous for patients. The longer that the patients stay in ED after their treatment has been completed, the greater is their morbidity and associated mortality.
"Recent media coverage has reported numerous anecdotal accounts of how appalling the situation in an increasing number of our Emergency Departments has become. These departments are not outliers. Many of the trusts we work in are in similar positions," it warns.
NHS England has stopped publishing weekly figures measuring A&E performance. But the figures, from those in charge of around half of A&E departments state: "Last week’s 4 hour performance target was between 45 and 75%. Thousands of patients are waiting in ambulances for hours as the hospitals lack adequate space. "
The senior doctors said their hospitals were dealing with:
Over 120 patients a day managed in corridors, some dying prematurely
An average of 10-12 hours from decision to admit a patient until they are transferred to a bed
Over 50 patients at a time waiting beds in the Emergency Department
Patients sleeping in clinics as makeshift wards
It comes as hospital chiefs said the NHS was at a "watershed moment" and needs tens of billions in extra cash to deliver the required levels of care.
NHS Providers, the trade body which represents NHS services, had previously warned the health service was "not where it would want to be" heading into winter amid concerns over a bad strain of flu.
A letter, written to Jeremy Hunt, the Health and Social Care Secretary, calls for extra investment on a long-term basis - and help with the immediate financial impact of "exceptional winter pressures" - to address the "fragility of the wider NHS".
Chris Hopson, chief executive of NHS Providers, said last year was "the first time ever" in NHS history that all of its key targets for A&E, cancer and planned operations across the UK had been missed.
He said hospitals were short of 10,000-15,000 beds, calling on the Government to invest billions more on the NHS.
Tens of thousands of non-urgent operations and routine outpatient appointments have been shelved by NHS England to ease pressures on hospitals.
Dr Nick Scriven, president of the Society for Acute Medicine, said today's data showed the NHS was struggling to cope, but hid the misery and lack of dignity for patients.
“These figures support the messages we have been getting from our members about conditions across the NHS and the struggle they are facing to provide safe and compassionate care in exceedingly difficult conditions," he said.
And he warned worse could come as flu spreads across England.
Dr Scriven said: “NHS Providers is right when it says we are at a watershed moment in the health service and the government must recognise this - it has had long enough and been warned of this dangers enough times in the last two years alone.
“The data hides the misery and lack of dignity some people are being treated with and it is a potentially worrying side note that the Care Quality Commission is postponing inspections during 'winter,'" he added.
Liberal Democrat former Health Minister Norman Lamb said: "The NHS is facing record levels of pressure - meaning every day patients are dying and experiencing dreadful failures of care.
"Yet all the government does is offer inadequate sums of money which barely keep our health service going. "Theresa May cannot ignore this crisis any longer. Ministers have a choice: agree to work with others to deliver a proper, sustainable settlement for the NHS or be left with blood on their hands."
Health officials said the four-hour A&E performance in December was the same as it was last January, even though the NHS had treated almost 40,000 more patients within four hours.
Latest figures show a tripling in patients hospitalised with flu, with one in four cases suffering from the deadliest strain, dubbed Australian flu, after it fuelled the country’s worst season for two decades.
Across England, around 4.5m people are estimated to be suffering from flu-like symptoms, while across the channel, France has declared an epidemic.
The Department of Health says ambulance crews should be able to hand patients over to A&E staff within 15 minutes of arrival at hospital, and not doing so increases the risk to patients due to delays in diagnosis and treatment, as well as the chance that a patient will get worse while waiting on a trolley. But 16,690 patients waited at least half an hour in the last week, the figures show.
Meanwhile there were record calls to 111, with 1.68 million such calls last December, up from 1.48 million the previous year.
A spokesperson for the Royal College of Surgeons said: “December’s A&E performance is disappointing and shows a system under pressure. It further demonstrates why it has been necessary to cancel patients’ non-urgent procedures until the end of January.
“Despite the best efforts and dedication of NHS staff to treat patients quickly, waiting times for non-urgent care have also deteriorated again in the past year.
“Last week, NHS England advised that hospitals defer non-urgent inpatient planned care until the end of January and that day-case procedures and routine patient appointments should also be deferred where this will release clinical time for emergency care. Although this should help relieve some of the pressures on hospitals and avoid last-minute cancellations, it is a short term solution and will cause huge disruption to those patients whose appointments and operations have been cancelled. The fact remains that we do not have adequate funding or capacity in our health or social care services.”
An NHS England spokesman said: “Despite the clear pressure on the NHS in December, with rising levels of flu and record numbers of 111 calls and hospital admissions, we managed to hold A&E performance at the same level as last January.
"We also saw the best seasonal performance on NHS delayed transfers of Care in four years, and went into winter with cancer and routine surgery waits both showing improvements."
The latest weekly figures show 23 trusts which hit 100 per cent occupancy in the week ending 7 January.
Three trusts - The Hillingdon Hospitals NHS Foundation Trust, James Paget University Hospitals NHS Foundation Trust and Walsall Healthcare NHS Trust - were at full capacity on every day of the week.
Last year, the British Red Cross provoked outrage by declaring a "humanitarian crisis" in the NHS as pressures mounted.
Today its chief executive Mike Adamson said: “Despite the best efforts of hardworking NHS staff, many A&Es and emergency departments remain under serious pressure this winter.
“It is increasingly clear that we will never address the ongoing pressures on hospitals by focusing on the NHS in isolation. We need a joined-up approach to health and social care, because we know that many people’s health problems start in the home."
Hospitals which hit 100 per cent capacity in the week ending January 7
The Hillingdon Hospitals NHS Foundation Trust
James Paget University Hospitals NHS Foundation Trust
Walsall Healthcare NHS Trust
Barnsley Hospital NHS Foundation Trust
Weston Area Health NHS Trust
The Princess Alexandra Hospital NHS Trust
East Cheshire NHS Trust
North Middlesex University Hospital NHS Trust
The Whittington Hospital NHS Trust
Kettering General Hospital NHS Foundation Trust
Isle Of Wight NHS Trust
Croydon Health Services NHS Trust
Lewisham And Greenwich NHS Trust
Northampton General Hospital NHS Trust
West Suffolk NHS Foundation Trust
Tameside And Glossop Integrated Care NHS Foundation Trust
East And North Hertfordshire NHS Trust
Milton Keynes University Hospital NHS Foundation Trust
Bolton NHS Foundation Trust
Leeds Teaching Hospitals NHS Trust
Salford Royal NHS Foundation Trust
South Tyneside NHS Foundation Trust
University Hospitals Of Morecambe Bay NHS Foundation Trust
Source: NHS England

 Yahoo News
Yahoo News 
