Closure of record numbers of GP practices forces 250,000 patients to go elsewhere
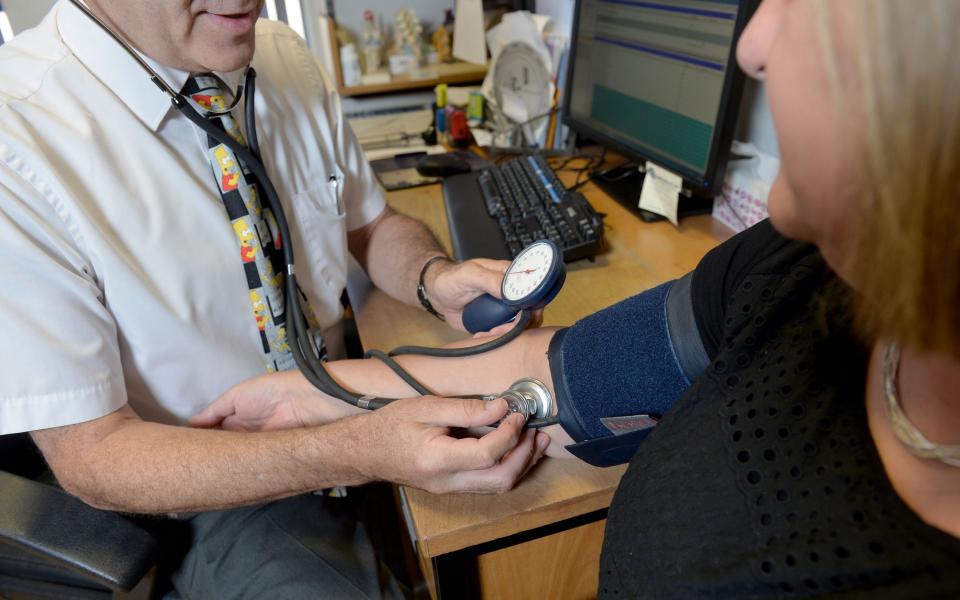
Record numbers of GP practices are closing, following a rise in the number of doctors retiring early ahead of a tax clampdown on pension pots, new figures show.
More than 250,000 patients have been “displaced” by surgery closures in the last year, amid plummeting GP numbers, the figures reveal.
In total, the number of practices closing has risen five-fold since 2013.
Senior doctors last night said communities were being left bereft, with elderly patients increasingly enduring long journeys to see a GP, and longer waiting times.
The exodus follows a series of tax clampdowns on bumper pensions, which have seen a sharp rise in the number of GPs retiring early, and reducing their tax burden.
Since 2012, the cap on what savers can amass without being taxed has dropped from £1.8 million to £1 million.
Meanwhile, the numbers retiring or going part-time is failing to be matched by that of new recruits.
In the last year, the total number of family doctors has fallen by 400, despite targets to boost numbers by 5,000 amid rising demand.
The new figures, from Pulse magazine, show a five-fold rise in closures of GP practices since 2013.
In total, 92 practices closed their doors last year, with 57 shutting up shop completely, and the rest closing as a result of mergers into “supersurgeries”. This compares with 20 such closures in 2013.
As a result, 265,000 patients saw their practice close last year, the figures reveal - compared with just 43,000 in 2013.
The investigation shows some areas have been severly affected, with Brighton losing seven surgeries in two years.
Last month ministers disclosed plans for the country’s 7,500 surgeries to become 1,500 “superhubs”.
Health officials claimed the move would not see the closure of thousands of practices, with existing surgeries working more closely together.
But the new figures show a steep rise in closures already underway, while the average list size has risen by almost 20 per cent in a decade.
Last night GP leaders said the situation was a “tragedy” amid claims the NHS is “falling apart at the seams.”
Joyce Robins, from Patient Concern, said the situation was becoming devastating for patients.
"There is a critical shortage of GPs – and we are getting to the point where it will be impossible to see one," she said.
“Older patients will be worst hit. Many can’t travel and have been seeing the same doctor for 30 or 40 years and who knows their medical conditions.”

It follows warnings that waiting lists have reached up to four weeks in some areas, with senior doctors warning that such delays could cost lives.
The number of junior doctors choosing to train as GP is failing to keep pace with the numbers retiring early ahead of the tax clampdown, or going part-time.
Last year a report by the King’s Fund found that 15.5 per cent of GPs aged between 55 and 59 had left the profession in 2014 . The rate is twice that of a decade ago.
The tax clampdown on large pensions means that savers now pay 55 per cent tax on the share of pension pots above £1 million.
The figure has been steadily lowered from £1.8 million in 2012, with the final clampdown taking the cap from £1.25 million to £1 million last April.
Unions have estimated that most family doctors approaching retirement age would be hit by the latest tightening, with the average GP earning £100,000.
Meanwhile, rising numbers of existing GPs are choosing to go part-time, with many citing “burnout” from increasing numbers of consultations per day as a reason to work fewer days.
In just five years, the number of patient consultations has risen by 15 per cent, while the numbers waiting to see a GP have risen sharply.
Seventy per cent of female GPs and 28 per cent of male family doctors now work part-time, and nine in 10 trainees intend to do so, or to combine GP work with other roles.
The shortages come despite a national recruitment drive, with junior doctors offered “golden hellos” of £20,000 to train as a GP, and attempts to recruit hundreds of medics from Poland, Lithuania and Greece.
Why is the NHS under so much pressure?
Professor Helen Stokes-Lampard, Chairman of the Royal College of GPs, said: “GP practices are the lifeblood of our local communities so the complete closure of any practice will always be a last resort when all other options have proved unworkable.
“Unfortunately, too many practices are being forced to close because GPs and their teams can no longer cope with ever-growing patient demand without the necessary funding and workforce to deal with it.”
Dr Richard Vautrey, deputy chairman of the British Medical Association's GP committee, said: “The crisis in general practice is now impacting patients right across the country.
"Despite repeated and clear warnings by the BMA, a decade of underinvestment, and failure by successive governments to take the growing workload and workforce crisis seriously, has led to this situation."
A survey by the BMA of 46,000 doctors last year found 25 per cent were considering early retirement because of the pension changes.
Lib Dem Health spokesman Norman Lamb said: “This is damning evidence of a system that is falling apart at the seams.
"General practice is buckling under the strain of rising demand for care and massive challenges in recruitment."
An NHS England spokesman said: “All NHS patients wanting to register with a GP practice are guaranteed to be able to do so and we have increased investment in general practice by £1 billion in two years in order to improve services and boost GP numbers.
“These figures as presented don’t reflect the full picture as they include patients whose records automatically transfer after a merger and therefore don’t have to change practice. As part of our plans to improve general practice services and boost the workforce, many practices are choosing to merge in order to offer patients a much greater range of services.”
The disclosures come as a leaked government document revealed fears that Brexit could lead to a shortage of more than 40,000 nurses.
The “worst case scenario” outlined in Department of Health documents seen by Health Service Journal describe a “severe risk of undersupply” if immigration rules stopped all EU health workers coming to Britain.
Meanwhile, a report by the Nuffield Trust warns that A&E units have closed almost 500 times in recent months. The figure for the three months ending in February, is twice the average figure for the past three years.
It comes amid fears of a looming crisis in NHS services over Easter. Locum doctors have been accused of an “organised campaign” to hold hospitals to ransom by withdrawing from shifts at short notice, in order to force trusts to pay them more.
The dispute centres on changes to tax on such workers.
Worsening access to GP surgeries

 Yahoo News
Yahoo News 