Mass rollout of Oxford vaccine begins in England as hospitals pushed to brink
GPs in England are starting the mass rollout of the Oxford/AstraZeneca Covid-19 vaccine as hospitals across the UK face rising numbers of seriously ill patients.
The jabs are being delivered to sites across the country as the Government commits to offering a vaccine to more than 13 million people in the top four priority groups by mid-February.
It comes as NHS trusts in London are on the verge of being overwhelmed, according to leaked health service documents, while other trusts are rapidly turning normal wards into intensive care units (ICUs).
As of January 4, there were 30,451 people in UK hospitals with coronavirus, much higher than the April 12 peak of 21,684.
Meanwhile:
– A surgery visited by Health Secretary Matt Hancock to promote the vaccine launch in England is yet to receive supplies of the Oxford/AstraZeneca product. Shadow health secretary Jonathan Ashworth said the scenes were like something from political comedy The Thick Of It.
– The leader of Birmingham City Council, Ian Ward, said in a letter the city “has not yet been supplied with any AstraZeneca stock, while current Pfizer stocks are scheduled to run out on Friday”. Signed by Birmingham Hodge Hill MP Liam Byrne and Sutton Coldfield’s Tory MP Andrew Mitchell, it also demanded “a realistic forecast” and assurances that supplies of vaccines will keep pace with demand.
– Of the 269,886 people transferred to the NHS Test and Trace system in the week to December 30, 84.9% were reached, down from 86.4% in the previous week, and the lowest percentage since the week to October 28.
– In the seven days to January 3 there were 9,256 ambulance handover delays of between 30 and 60 minutes in England and 5,318 delays greater than 60 minutes. These are the highest weekly numbers so far this winter.

Exhausted staff in one of England’s largest hospitals have told the PA news agency they are working “to the limit” of their ability.
PA was granted rare access to St George’s Hospital in Tooting, south London, where the trust has had to vastly expand intensive care capacity and move under-qualified staff to high dependency roles.
Medical registrar Omome Etomi said it is impossible to predict the profile of patients brought in for care – and whether they will survive.
The 28-year-old said: “We are seeing patients across the spectrum, from their 20s right up to people in their 80s and 90s.
“It’s so unpredictable – I can’t tell you who’s going to be unwell and not, who’s going to improve and go home and who’s going to have a longer stay in ITU (intensive care or high dependency).
“I have admitted patients to the intensive care unit in their 20s and 30s, people who have no pre-existing conditions.
“There’s almost no pattern to it – we just can’t say.”
Dr Mark Haden, an emergency department consultant, said the rising number of very sick patients is having a huge impact on staff.
“Everyone’s stress levels are higher than usual,” he said. “Everyone is working to the limit, to the threshold of what they’re able to.
“The hospital bed occupancy is very, very high, it has lots of Covid patients as inpatients at the moment. It’s very stressful for staff and that is starting to show.”
Earlier, Rupert Pearse, professor of intensive care medicine and a consultant at the Royal London, said his own ICU staff are having to care for far more sick patients as he urged the public to heed the “stay at home” lockdown message.
He told BBC Radio 4’s Today programme there would usually be one fully-trained ICU nurse to one ICU patient but staff are becoming increasingly stretched.
“Right now we are diluting down to one (ICU) nurse to three (patients) and filling those gaps with untrained staff and in some instances doctors helping nurses deliver their care … and we’re even facing diluting that further to one in four,” he said.
“As intensive care doctors, we’re not sure how we can together deliver the quality of care that we need to.”
Speaking on behalf of the Intensive Care Society, he said the problems are not just in London, but in other hospitals across the UK, and are not limited to ICU wards.
He added: “We are really very concerned now about the seriousness of the situation … which is definitely worse than the first wave and proving much harder to deal with now as the resources we had in the first wave aren’t available to us.
“So we’re really struggling to provide the quality of patient care that we think patients deserve. And the impact of the pandemic is taking care away from other illnesses such as cancer and heart disease.
“In essence, the healthcare available to all of us is not as good as it should be right now.”
Prof Pearse said that unless people take the lockdown seriously, the impact on healthcare across the country “could be catastrophic”.
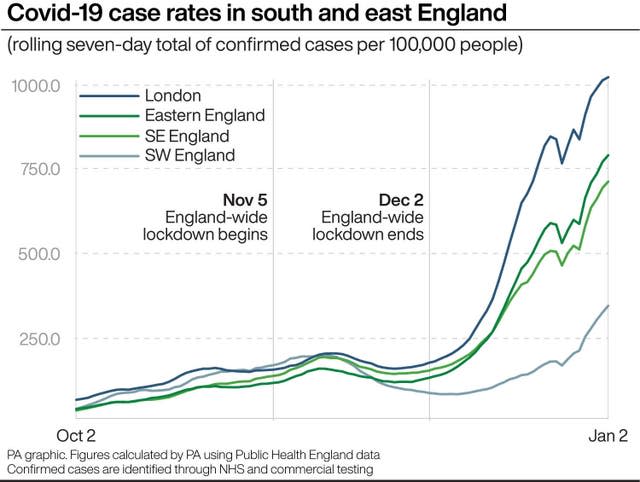
According to an NHS England Zoom presentation seen by the Health Service Journal (HSJ), hospital capacity in London will not be enough for the expected rise in patients in the coming weeks.
The data showed that, even if the number of Covid patients grows at the lowest rate considered likely, and measures to manage demand and increase capacity, including opening the capital’s Nightingale hospital, are successful, the NHS in London will be short of nearly 2,000 general and acute (G&A) and intensive care beds by January 19.
Meanwhile, the chief executive of NHS Providers, Chris Hopson, told the Today programme that hospital bosses across England are looking to the care and nursing home sector for any spare capacity.
He said the Exeter and Manchester Nightingale hospitals are currently being used but Nightingales are the “last-resort insurance policy” as they are not “purpose-built for health and care” and require the diversion of staff.

Elsewhere, Dr Richard Cree, from the South Tees Hospitals NHS Foundation Trust, urged people to follow the rules, writing on his blog: “I have spent a torrid few days desperately trying to keep people alive and failing.
“We have all seen far too many people die. Please, please stay at home.”
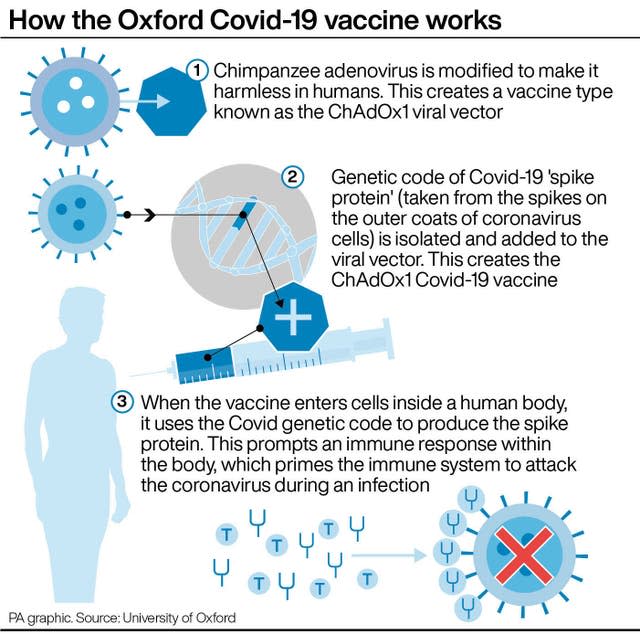
The first community vaccinations in England with the Oxford/AstraZeneca jab taking place in GP surgeries on Thursday and it is hoped that around 1,000 sites will be delivering vaccines by the end of the week.
The vaccine can be stored at normal fridge temperatures, unlike the Pfizer jab which requires storage at minus 70C.
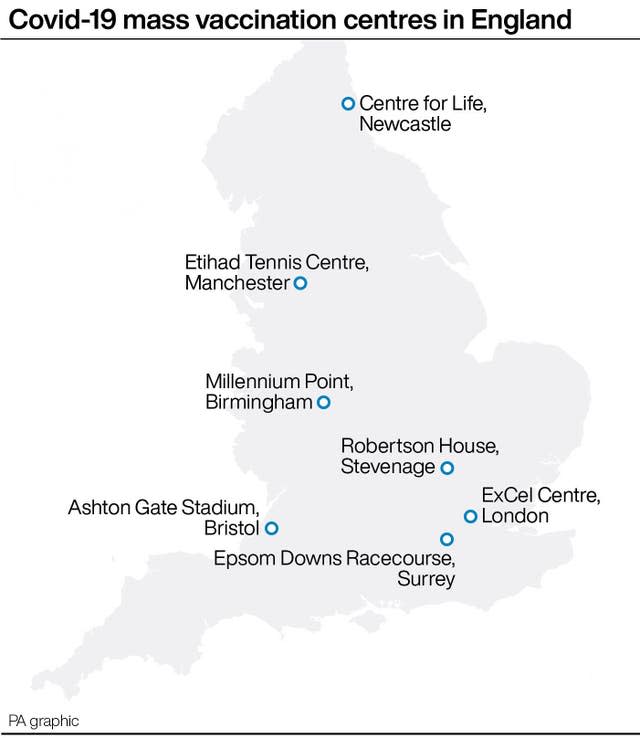
Seven mass-vaccination centres will also open next week in London, Newcastle, Manchester, Birmingham, Bristol, Surrey and Stevenage.

 Yahoo News
Yahoo News 
