Oxford vaccine trials suspended but not 'doomed' after UK woman hit by rare neurological disorder
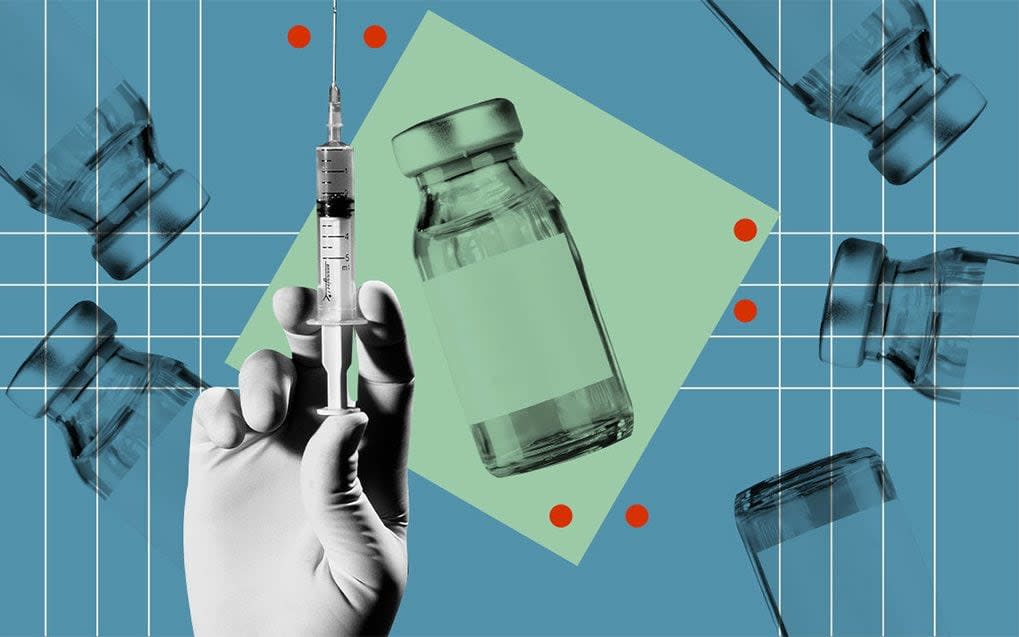

The revelation that AstraZeneca and Oxford University have suspended their phase three vaccine trials after a British female participant fell ill with a rare neurological condition is bad news but may yet prove to be no more than a bump in the road.
The pause will delay the progress of the vaccine making the possibility of it receiving an emergency licence this year much less likely. But experts expect the trials, which are being run in the UK, Brazil and the US, will almost certainly be allowed to continue to allow further data to be gathered and assessed.
The scientific community has been out in force to stress the positives. The suspension of the trial, said experts, demonstrated patient safety was paramount and that the complex system of regulatory checks and balances was working as it should.
“It’s always a concern if someone in the trial develops a serious adverse reaction… but if we had five or six cases I would be much more alarmed,” Prof Beate Kampmann, director of the Vaccine Centre at the London School of Hygiene and Tropical Medicine, told The Telegraph. It was far too early to say the trial was “doomed”, she added.
Yet the incident raises cause for concern - and stock prices in AstraZeneca tumbled after the news broke on Tuesday night that one of the participants, a British woman, had suffered a suspected bout of transverse myelitis.
Ever since President Gerald Ford rushed through the licencing of a novel flu vaccine in 1976, fears of vaccines sparking dangerous neurological side effects have stalked the industry.
Ford acted against scientific advice to licence the mass distribution of a novel HIN1 shot in the US after an outbreak of a new strain of influenza at the Fort Dix military base in New Jersey. He feared it was the start of a pandemic and reasoned it was better to move fast to get ahead of it even if that entailed some risk. It was also an election year.
The pandemic never arrived but the vaccine caused Guillain-Barré syndrome, a neurological condition that can lead to paralysis, in 450 of the 45 million people who received the jab. More than 30 died, sparking a scandal that underpins much of the safety regulations in place for vaccine and drug development today. Ford lost the election in its aftermath.
AstraZeneca’s CEO, Pascal Soriot, said the woman who suffered the suspected adverse effect is recovering and is expected to leave hospital today.
Watch: Yahoo UK Health Correspondent, Alexandra Thompson explain the complications linked to the coronavirus
Mr Soriot added that the trials had also been paused in July after a different participant experienced neurological symptoms. However, these were proven to be unrelated to the vaccine and the individual was diagnosed with multiple sclerosis.
Guillain-Barré syndrome and transverse myelitis are different but related conditions. Both affect the nervous system and can be caused by viral infections and vaccines. And both have also been associated with confirmed cases of Covid-19 and Sars.
Transverse myelitis can cause paralysis, sensory problems and bladder and bowel dysfunction. Most people recover but severe attacks can lead to lasting and serious disabilities.
Several studies have drawn “limited connections” between the condition and vaccination. A 2018 study analysing three decades of data on adverse vaccine events in the US found 119 cases of transverse myelitis - a tiny figure when compared to the number of people vaccinated, but researchers suggested it could be a “very rare” side effect.

Experts say it will be all but impossible for AstraZeneca to know if the adverse event reported yesterday was caused by the vaccine. Instead, they will look at the background incidence of transverse myelitis in the population to understand the probability of it being a random event.
It is likely the trial will then continue, say experts, with additional protocols put in place to actively seek out any additional cases.
The pausing of the current trial is a blow not least because the Oxford vaccine is one of the most promising in development outside China.
The jab is considered a leader not just because it has made rapid progress, but because it is keenly priced and relatively easy to manufacture and distribute. This means it could be widely distributed across the globe - the key to stopping the pandemic.
The Ebola vaccine, which is also based on an adenovirus vector and gained regulatory approval last year, was given to 300,000 people in a recent epidemic in the Democratic Republic of Congo, which was declared over in June.
Having been a significant factor in ending one epidemic, experts have high hopes that the adenovirus technology will yet rid the world of another.
Bumps in the road are unlikely to be confined the adenovirus-based vaccines, according to the Government's chief scientific adviser Sir Patrick Vallance.
“We should expect in other trials situations where things are paused and restarted. It's wrong to just jump over those stages and approve a vaccine on hope, you have to do it on evidence.”
Speaking at a Downing Street press conference he added that there is still a “reasonable chance” that a coronavirus vaccine will become available next year, with the first read-outs of final stage data expected before the end of 2020.
“Many of these vaccinations are showing the right immune response. That is a very important step along the way of making a vaccine,” he said. “Hopefully before the end of the year we will get some indications that some do work and have the right safety profile.”
But even with a vaccine, experts are warning that there is no single intervention that will bring the pandemic to a close.
“Vaccines will allow us to make small steps to return to a sense of normality, but will not be, on their own a magic or instant end to the pandemic,” said Sir Jeremy Farrar, director of Wellcome.
“That can only come with nations, rich and poor, working together in the global, not national, long-term interest.”
Protect yourself and your family by learning more about Global Health Security

 Yahoo News
Yahoo News 
