The Perils Of Being A Black Woman Needing Medical Care
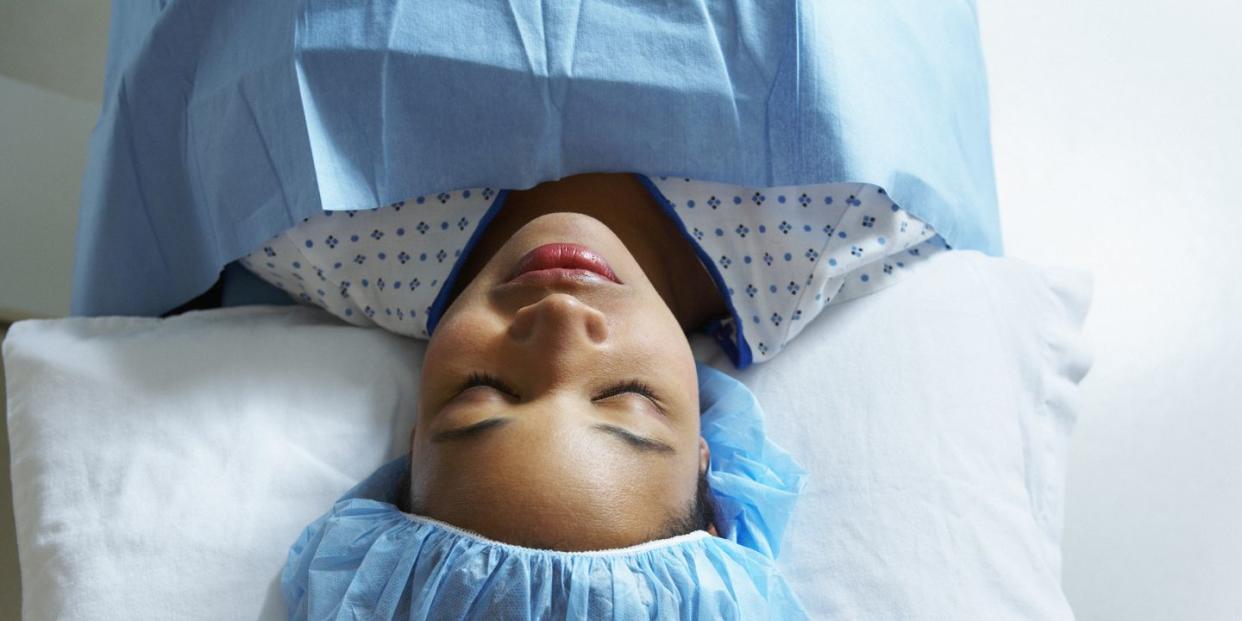
Stephanie Yeboah knows what it’s like not to be listened to by healthcare professionals. Two years ago, the body acceptance advocate was rushed to A&E in an ambulance after experiencing excruciating pelvic cramps.
So intense was the pain that she questioned whether she was a ‘one of those women who were unknowingly pregnant until labour,’ she tells ELLE. Unable to move or breathe, she described the pain she was feeling to the paramedics and said they refused to listen to her. ‘I literally thought I was dying and the more I screamed the less they listened, they even tried to tell me the pain was coming from a completely different part of my body.’
Once at the hospital, Yeboah states that she was repeatedly dismissed by the receptionist, even though she was visibly bleeding as she lay out on the floor in tears trying to suppress her feelings of pain. When she was eventually seen by a nurse, she says she was faced with inappropriate questions, such as: ‘Having a bit of a diva moment out there were we? Putting on a show?’
And the micro aggressions did not stop there. During her 10-day stay at the hospital for a suspected gallbladder issue, she indicated that she heard several sweeping generalisations about her condition, including a Caucasian nurse noting that, ‘west African women tended to suffer these sorts of complications because they eat too much Yam and plantain.'
For Yeboah, the experience confirmed that ‘medical racism and bias is a real thing…Black women die all the time due to negligence.’
While this summer’s Black Lives Matter Movement has triggered conversations around systemic racism in a way that’s not been seen before, especially in our judicial and policing institutions, there is still an area of systemic racism that remains underreported. And that is the inequality and discrimination that BAME people face in the healthcare system.
Although access to healthcare is an essential human right, Black people (who accounted for 13% of the British population in 2011 consensus) remain one of the most disadvantaged demographics when it comes to patient care within the system.
This has come into even sharper focus during the global pandemic. BAME patients have accounted for 34.5% of critically ill COVID-19 cases in the UK. One demographic that was disproportionately affected has been Black pregnant women: during the height of the pandemic, they were eight times more likely to be admitted to hospital with COVID-19. Astonishingly, women from a BAME background have accounted for 55% of the pregnant women admitted to hospital with COVID-19, despite only making up a quarter of the births in England and Wales.
But while the pandemic has highlighted the medical disadvantages Black people experience, the problem is not linked exclusively to COVID.
Black women in the UK are five times as likely to die in childbirth and the NHS’s own statistics show black babies have a 121% increased risk for of being born stillborn in comparison to white babies born in the same hospital. This shows that there is difference in the quality of care offered by identical providers. This includes post-natal care: Black babies are 50% more likely to die in the first 28 days in comparison to white babies.
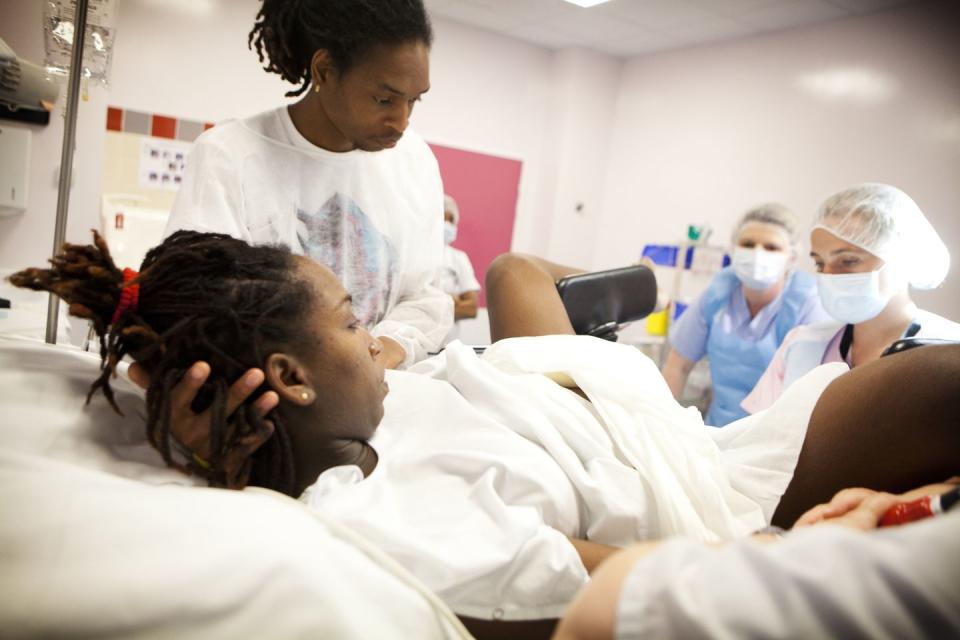
The need for change has not gone unrecognised, however, as England’s most senior midwife, Jacqueline Dunkley-Bent, has written to all maternity units asking for improved quality of care for Black women and has introduced the 2020 ‘Long Term Plan’.
The plan commits to ensuring that by 2024, three-quarters of pregnant BAME women will receive care from the same midwife before, during and after they give birth. This is proven to help reduce pre-term births, hospital admissions, the need for intervention during labour and to improve women’s over experience of care.
Many Black women feel that medical workers are influenced by personal biases that they subconsciously bring into the workplace. This bias has an effect on several areas of treatment, not just pregnancy and maternity care.
Kanayo Dike-Oduah, a doctoral student and Head of Psychology at a secondary school in London, was given Carbamazepine painkillers for wisdom tooth pain. The GP failed to mention that Black and Asian women tend to react badly to this type of medication.
Days later Oduah suffered a severe allergic reaction known as Steven’s Johnson disease. Her whole face was swollen, she had problems breathing (her lips had doubled in size) and had visible spots on her palm and dark marks on her face. She had to go to A&E three times consecutively.

On arrival, she says she was misdiagnosed with tonsillitis and conjunctivitis. Doctors then allegedly ignored red flags that indicated that she was suffering with a severe allergic reaction to Carbamazepine and failed to identify that her symptoms were typical of Steven’s Johnson disease. On her second visit to A&E, she claims the nurse omitted the protocol rash test which would've been able to help identify her symptoms.
Oduah says, ‘My sister visited the pharmacy on my behalf as the pain was increasing and we were growing more and more concerned.’ After seeing images of Kanayo, the pharmacist reportedly shouted, ‘Get this person to A&E NOW!’ On her third and final visit she was adamant that she had to be admitted immediately; the disease has a one-in-three mortality rate. Oduah continues: ‘the doctors later admitted that if I returned home, I would’ve died that night’. She won a case against the NHS for medical misconduct.
One reason for reduced quality of care seems to be the lack of diversity across medical and clinical training. In pharmaceutical studies, medicine, dermatological samples and across the NHS' own website, examples of disease are only shown on Caucasian skin. What’s more, a 2016 poll of 222 qualified doctors showed they believed that Black people had ‘thicker skin and shorter nerve endings’ which gave them a higher pain threshold than white patients. The poll revealed that the doctors maintained that Black people could go longer periods of time without the need for painkillers, something that remains unsupported by medical evidence.
More recently however, and in light of conversations around the effect of the pandemic and the BLM movement, there has been a call for modernisation and accountability on the part of healthcare institutions. This is largely driven by a new generation of professionals and students.
In the UK, petitions have started demanding medical institutions to diversify the case studies that students are shown during medical training. The GMC (General Medical Council) has stated that they acknowledge and support the need for reform but ‘can only set the standard for medical schools to follow’. In other words, they have no way of ensuring this kind of reform actually comes to pass.
But the drive is also coming from students themselves. Newly qualified dermatologist Michelle started a petition with almost 5,000 signatures demanding more diversity in the skills taught and the symptoms identified. She said ‘one of the many reasons this is so important is because it affects so many different areas of pathology. For example, one sign of a lack of oxygen is lips turning blue and this is much harder to identify on dark skin until a patient has reached a critical stage and healthcare workers would not necessarily know this until there is greater exposure to black patients.’ The British Association of Dermatologists has responded to the petition, pledging to make improvements.
It is encouraging to see that change is coming from ‘the bottom up,’ as a new generation of medical students spearhead the movement out of frustration.

Medical student Malone Mukwende has just written ‘Mind The Gap’, a clinical handbook detailing how to identify the signs of disease presented on darker skin. He noticed the need for change during his first year of university, after consistently being expected to assess Caucasian skin exclusively. He says it was as if resources showing darker skin ‘didn’t exist’ and that he knew the system needed ‘decolonisation’. The handbook will be available to medical schools nationally and Mukwende wants it ‘to become a staple in all medical institutions across the UK and eventually in the world. This being everywhere from medical school libraries through to GP consultation rooms’.
It’s clear that there is a desperate need for more diversity and representation in healthcare at every level. There is still a very long way to go in terms of progress, but with a new generation of medical staff and students driving change from within the healthcare system, and more reporting on such issues, much needed change could be closer than we think.
Like this article? Sign up to our newsletter to get more articles like this delivered straight to your inbox.
In need of more inspiration, thoughtful journalism and at-home beauty tips? Subscribe to ELLE's print magazine today! SUBSCRIBE HERE
You Might Also Like

 Yahoo News
Yahoo News 
