Scientists develop new opioid painkiller that could help prevent lethal overdoses
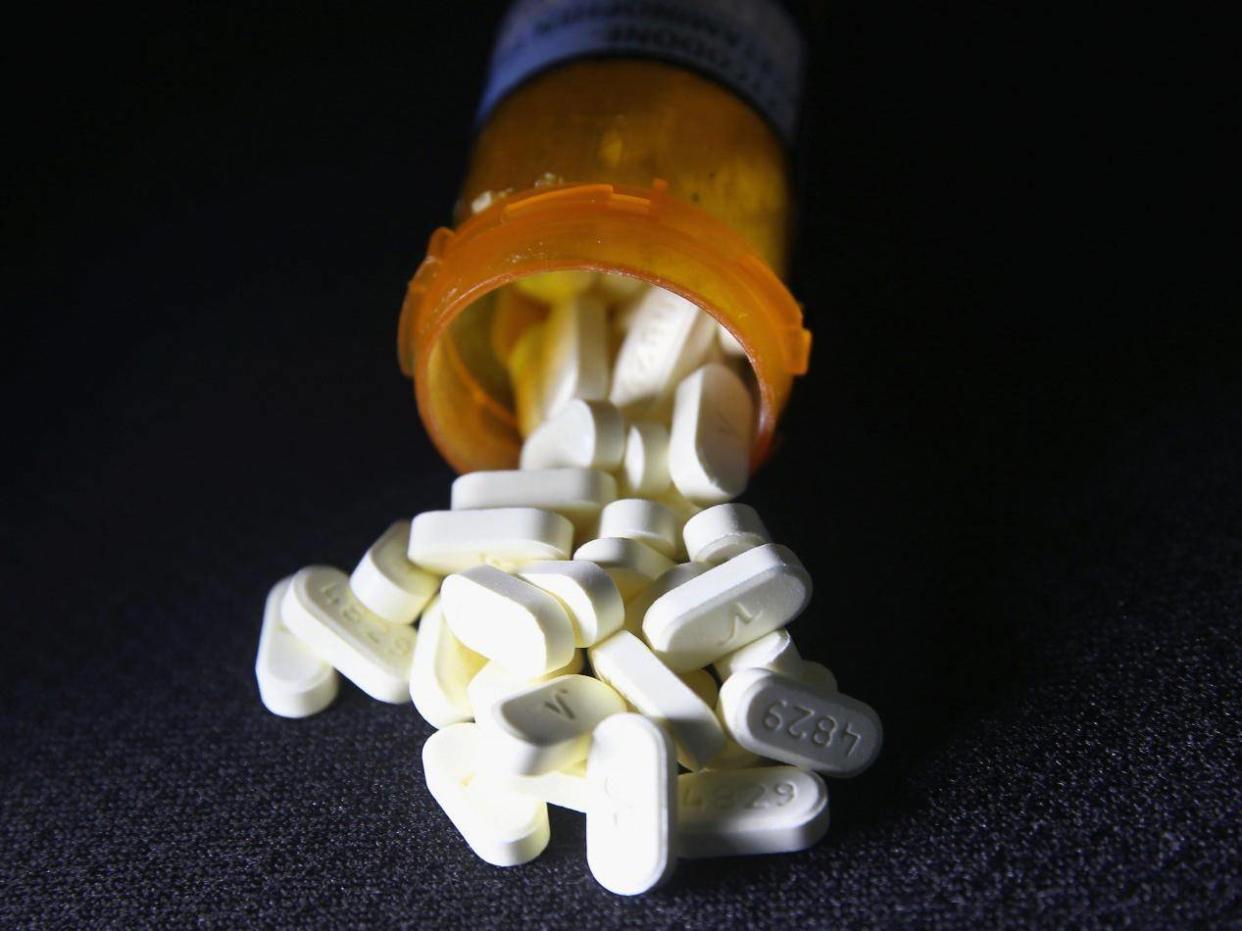
A new model for developing painkillers could help cut opioid related overdoses, which killed around 2,000 people in the UK last year and which account for the deaths of 91 people every day in the states.
Research published in the journal Cell on Thursday demonstrates it is possible to develop opioids which relieve pain as effectively as morphine but without stopping or slowing breathing.
There were 3,744 drug poisonings in the UK in 2016 and 2,038 involved an opiate, most commonly heroin or morphine, Office for National Statistics figures show.
But in America prescription opioid addiction has devastated communities and left hundreds of thousands dead, with Donald Trump declaring it a public health emergency earlier this year.
The crisis in America has spiralled since the 1990s with overprescribing of addictive medications, high levels of chronic pain, and an influx of potent synthetic opioids, like fentanyl.
Fentanyl is usually used to relieve pain in terminally ill patients and, at a strength 100 times that of heroin, is a growing cause of deaths in the UK.
Researchers at The Scripps Research Institute, Florida, have spent two decades looking at ways of unlinking opioids' effects on two pathways - the “G protein” pathway, which is thought to mediate pain-relief and the “beta-arrestin2” pathway, which is linked to breathing suppression.
In the last six years they have developed 500 potential new painkiller drugs compounds, 60 of which impact more on one or the other pathway.
In this group they identified key drugs, all of which were able to be absorbed to the brain, and were all as potent as morphine “if not more so”, but some of which only impacted one pathway.
The compounds that were more lethal in mice primarily acted on the beta-arrestin2 pathway, and this is the primary way that fentanyl acts – possibly explaining its high rate of overdose.
The study says that the findings “strongly support the hypothesis that compounds that do not recruit beta-arrestin2 may prove to be safer than current clinical opioids.”
However it has still not been conclusively proven that beta-arrestin2 is the main cause of breathing suppression - there could be other factors at play.
It’s also yet to be seen if drugs that avoid this pathway have other side-effects, such as being more addictive or causing constipation, that would undermine their lower overdose risk.
But the drugs identified in the research have the largest separation of pain and breathing suppression of any study so far, the authors conclude: “Our hope is that this work may aid the pharmaceutical development of safer alternatives to current opioid therapeutics.”

 Yahoo News
Yahoo News 
