Coalition gave private pathology companies lucrative Covid contracts
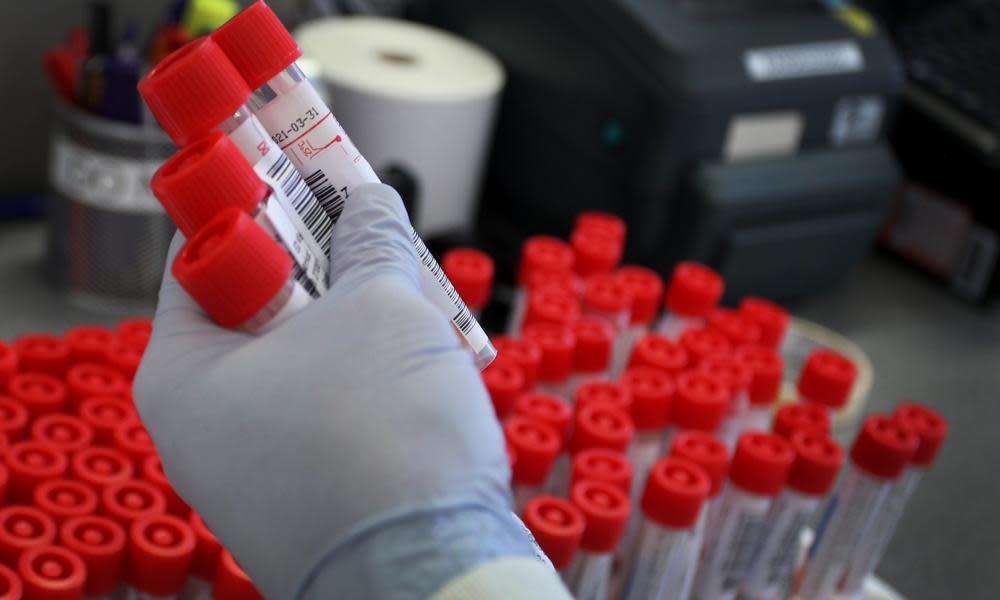
The Australian government handed major pathology companies lucrative Covid-19 contracts through limited tenders, shielded their closed collection centres from takeover, provided large subsidy increases after industry lobbying, waived normal registration fees and promised to provide additional assistance outside jobkeeper.
Guardian Australia has spent the past week examining aspects of the federal government’s response to coronavirus, investigating problems with jobkeeper, the childcare support package, and the potential economic impact of the sudden cessation of stimulus.
A critical part of the government’s response was aimed at helping the highly concentrated and influential private pathology sector.
Related: Questions raised over hydroxychloroquine study which caused WHO to halt trials for Covid-19
The sector has played an important, providing important testing capacity at a time of immense need. The sector also suffered a significant financial hit when non-Covid-19 testing declined in the middle of the pandemic.
The sector has lobbied government, including through its peak group Australian Pathology, for assistance. In one case, it threatened to stop providing Covid-19 testing unless the subsidy it received was drastically increased.
The government has since made a significant package available to private pathology, including:
Increasing the Covid-19 testing subsidy to private pathologists to $100 a test, applied retrospectively. The subsidy is vastly above the $50 received by public pathology for Covid-19 testing, despite public pathologists warning they are conducting testing at a loss in rural and remote areas. Australian Pathology, the peak group for the private sector, says this subsidy is actually only $85 a test, and that the comparison with public pathology is not fair, because public pathologists are remunerated in other ways. Private pathology argues that the testing is complex, new and extremely expensive, and that, before the increase, the subsidy was well below cost. Sonic, one of two massive players in the sector, said the increase to $85 “was simply correcting what the initial test fee should have been when introduced only days earlier”.
Waiving of approved collection centre registration renewal fees between 27 March and 30 September.
The introduction of a moratorium on the opening of new pathology approved collection centres to replace any existing centre that closes down due to low testing volumes, between 27 March and 30 September. This has effectively shielded existing pathology providers from others taking over their newly vacant collection centres. Many collection centres are co-located within GP clinics and the rent is a critical source of revenue for GPs.
The government also says it plans to offer additional financial assistance to private pathology companies which are not eligible for jobkeeper. The health department said the details are being worked on but the aim of the extra assistance is to help private pathologists retain permanent staff, and maintain rural or regional pathology collection and urban collection points in critical areas.
The Australian Pathology chief executive, Liesel Wett, said the measures were crucial in supporting an important sector amid a significant downturn, caused by the drastic reduction in demand for non-Covid pathology during the crisis.
“How critical were these measures? Extraordinarily critical, all of them,” she said.
Sonic – which, along with Healius, dominates the market – was also given a $22m contract to run a rapid Covid-19 collection and testing service for aged care facilities between 30 April and 30 September.
The health department said the contract was awarded through a limited process due to the urgency of the situation. The department said it only approached major pathology providers with existing collection and testing capacity across at least one full state.
No details were published on the government’s public contract database, Austender, until questions from the Guardian.
Sonic announced to the Australian Securities Exchange that about 2,700 aged care providers were eligible to use the service.
A number of states and territories, including Western Australia, New South Wales, and the Australian Capital Territory, told the Guardian they were not using the testing service that Sonic was contracted to provide.
NSW said it has not “requested Sonic Healthcare to conduct testing for any outbreak investigation in an aged care facility”. During NSW’s Newmarch House outbreak, the state government said it had the capacity to test every staff member of the aged care facility daily.
A Queensland Health spokesman said: “Pathology Queensland is more than capable of meeting the public health system’s needs in normal circumstances, including all public Covid-19 testing.”
The ACT said it had not yet used the Sonic service, though would consider doing so if there was a major outbreak at an aged care facility. WA said it had enough capacity but welcomed any new testing options.
Victoria and Tasmania said they had worked with Sonic on aged care testing.
The federal health department acknowledged that “some states have so far decided to do all aged care testing in public laboratories”.
“The tender was to provide a service that supplements, not replaces, existing public health pathology services in residential aged care facilities through the provision of services from the private sector as required,” a spokeswoman said.
Sonic Pathology Australia’s chief executive, Ian Clarke, said the company had tested more than 1,000 residents of aged care facilities through the contract. He categorically rejected any suggestion that the tender was not open.
“It was an open federal government tender that Sonic Pathology Australia participated in and was awarded,” he said. “SPA laboratories have for years performed more nursing home collections and testing than any other pathology provider, including the combined public sector which hasn’t had much presence in that space.”
Related: Newmarch House took six days to accept government-funded coronavirus medical staff
Jenny Sikorski, the chief executive of Public Pathology Australia, said her members had been testing in aged care facilities and “continue to have the capacity”.
Sikorski said state and territory governments were being told they could now choose between public pathology and Sonic for their aged care testing.
She said it was good to have additional capacity in the event that there were numerous outbreaks in aged care facilities at the same time, but that that hadn’t yet occurred in Australia.
As it stood, she added, the contract had created confusion.
“The thing with the contract is that it has brought an element of confusion into who should be doing the testing, that hadn’t been there before. That’s the one thing it has created.”

 Yahoo News
Yahoo News 
