When does life end? A father didn’t believe his daughter was dead. The hospital still harvested her organs
Mike O’Connor had just been told that his daughter was brain dead.
Brittany had been in the hospital for six days. One end of a thick blue tube was taped to her mouth, the other connected to a respirator, which pushed air into her lungs with a mechanical force that shook her chest up and down.
Each day, he’d come to her bedside to hope and pray she would open her eyes. And that’s where he was, by her bed, when a policeman entered her room at the intensive care unit at Fresno community hospital.
Mike didn’t believe that Brittany was dead. Forcefully, he told the care team that she was alive, that she was fighting, that they just wanted her heart, her lungs, her kidneys for donation. He feared that the hospital would remove her from life support and that Donor Network West would procure her organs.
He thought he was fighting for his daughter’s life.
Mike believed the hospital and the organ procurement organization needed his consent. Yet the hospital had now called a police officer to remove him from Brittany’s bedside, to remove him from the hospital premises.
“She is without a doubt responding to my touch,” Mike told the officer. “They wanted me to pull the plug, but I said no.”
Mike was given three minutes to say goodbye to his daughter.
•••
At the time of her death, Brittany was 26. She was the mother of two children, 10-year-old Lexi and four-year-old Lane. She was bright-eyed, funny, a little rebellious, and close to her sister, Kaylee. She did hair for friends at her home, giving them highlights and colors. But she also struggled with addiction for nearly a decade, getting clean at times and then falling back into use.
In the early morning hours of 17 November 2017, she was taken by ambulance to Fresno community hospital with hypoxia from an “unknown duration” of asphyxiation.
Her live-in boyfriend reported that he had found her after an apparent suicide attempt. He called 911 as a neighbor gave Brittany CPR.
Mike wanted the officer – who, as he saw it, was charged to do what was right – to force the hospital’s staff to hear his pleas.
“Brain dead patients cannot respond to touch, and she clearly is… right?” Mike desperately said, touching Brittany’s warm body. Brain dead patients cannot respond to external stimuli. “That doctor came in and started talking to me about body parts and donating them.”
The police officer told Mike that he was a father too. “I don’t want to take you to jail,” he said. “That’s the last thing I want to do.”
“I’m afraid they’re going to kill her,” Mike told him. “Them pulling the plug on her now would be murder. And now I am worried about her safety.”
After three minutes, the officer escorted him out of the hospital.
Once home, Mike posted a message on Facebook asking his friends to call the hospital: “TELL THEM NOT TO PULL HER PLUG.” When he called the next day, he says, they refused to tell him where Brittany was.
Throughout the day, Mike posted a series of Facebook messages displaying escalating anxiety: the hospital was denying him information and access to his daughter, and then trying to kill her. Finally, he wrote: “THEY WANT HER ORGANS!”
What Mike did not know is that, while he was begging friends to call the hospital and updating family about her health, doctors were already removing Brittany’s heart, kidneys, liver, and lungs. The next day, her tissue was collected for donation.
No one from the hospital called Mike. He says he did not receive confirmation that Brittany was dead until three days later, when the coroner called to ask what Mike wanted to do with her remains.
•••
How we die is a deeply misunderstood process. Dying is not a momentary last breath after a serious illness or a tragic accident, but often the shutting down of a series of bodily systems, primarily the heart and lungs (circulation) and the brain (neurological function).
This has always been so, but in the 1960s medical advancements began to isolate and address circulation. These advancements include respirators that can mechanically force lungs to function, and defibrillators that can sometimes restart the heart. But there is still no way to resuscitate a human brain after its cells have ceased to function.
It was in 1967, when the first heart transplant was performed in South Africa, that the world of medicine realized the use of a dead person’s organs to save the life of another. Patients without brain function, but whose heart and lungs were mechanically revived, were ideal organ donors; their organs were healthy because circulation (artificial or not) had maintained them.
The next year, a multidisciplinary team at Harvard Medical School convened to examine what it meant for a person to have heart and lung function, but not brain function. Their objective was twofold: to establish uniform criteria to determine when a brain had ceased to function; and to provide the burgeoning organ transplantation practice with a clear source of healthy organs.
Haider Warraich, a physician and professor at Harvard Medical School, wrote in his book Modern Death: “The Harvard committee spoke as much to the legal community as it did to the medical, keenly aware of just how far behind the courts had been left by advances in medical resuscitative science.”
Over the next decade, various US states had established their own legal and medical brain death precedents, often as the result of lawsuits. But from one state to another, the definition of death was not uniform, rendering it different in Wyoming, say, than it was in Kansas.
It wasn’t until 1980, when President Jimmy Carter convened a taskforce that included theologians as well as doctors, historians, neurosurgeons and other experts, that a nationwide definition of death was established.
The Uniform Determination of Death Act (UDDA) offered two statutory definitions for when an individual is legally declared dead. There were now two ways to die: based on circulatory criteria (heart and lungs) and neurologic criteria (the brain).
In the latter, patients can not respond to external stimuli, like touch, but latent nervous system activity can be deceptive. Mike, for example, mistakenly thought that Brittany was responding to his touch. The body is warm, the patient breathing because circulation is often continued with medical assistance.
The UDDA was effectively adopted by all 50 states. Ultimately only one, New Jersey, offers a religious exemption, and three others – New York, California, and Illinois – allow “reasonable accommodations” to families who require additional support in coping with the diagnosis.
It was apparent to the UDDA authors that clear guidelines were imperative to the public’s comfort with organ donation; the act allowed the creation of today’s organ procurement and transplantation system.
More than 40,000 lives a year are saved by organ donation. It is a revolutionary technology that has changed the medical system for the absolute good. It is also directly tied to the development of brain death criteria because, like Brittany, a vast majority of donors – more than 65% – are declared dead by neurological criteria, or brain death, before their organs are procured.
“If anything, it is a relief not only for physicians but for families [of organ donors] when patients do meet the criteria for brain death,” Warraich wrote. Surveys show that these family members who choose donation find solace in their grief, knowing that their tragedy has extended the life of someone in need.
But for some who are mistrustful of or feel manipulated, bullied, or disrespected by the medical institution they are at the mercy of, their loved one looks deceptively alive.
•••
After Brittany’s death, things fell apart for Mike. Over the next two years, his life shut down: he gained 150lb and his alcoholism came rushing back. He was unemployed. Then his mother died. At one point he found himself homeless, living in his truck with his dog.
A family connection brought Mike to an experienced trial lawyer named Thornton Davidson. In 2018, they filed a lawsuit against Fresno community hospital and Donor Network West. It claimed that the hospital and organ procurement organization (OPO), “without proper and effective legal authorization”, had “performed or assisted in harvesting organs and body parts from [Brittany]’s dead body, and in doing so mutilated, desecrated, violated and outraged [Brittany]’s human remains”.
The lawsuit claimed that the hospital and OPO had frozen Mike out of the decision-making process for Brittany’s care, instead favoring Mike’s ex-wife, Shawna, Brittany’s mother. Mike said they did this as soon as they learned that he did not want her organs to be donated and that he believed she may still be alive.
(Counsel for both organizations declined to comment for this article.)
Brittany was an unmarried adult without adult children. The suit claimed that both organizations had colluded to violate the California Uniform Anatomical Gift Act by conspiring to obtain consent from only one parent instead of the legally required two, and that they made no “reasonable effort” to contact Mike for his consent.
The lawsuit said the hospital and OPO were responsible for the intentional infliction of emotional distress on Mike.
In July 2019 the defendants, Fresno community hospital and Donor Network West, asked the court of Judge Rosemary McGuire to dismiss the intentional infliction of emotional distress clause from the suit. The court agreed.
To Mike and his lawyer, the court had made a mistake; Mike was “committed to proving that the hospital and donor network had intentionally caused him harm – not just that they had done so by accident”, according to Davidson. They took their claim to the fifth district court of appeals.
On 31 January 2022, the court decided Mike’s case could proceed. “We conclude that O’Connor’s broader conception of extreme and outrageous conduct is correct,” the opinion said, “and that his allegations of defendants’ intentional conduct directed at him, and reckless conduct in his presence, are sufficient to state a cause of action for intentional infliction of emotional distress.”
For Mike and Davidson, the case doesn’t rest on how Mike behaved while Brittany lay dying, nor is it about whether Brittany was dead or alive when Mike was escorted from her hospital room.
Instead, they say their suit exists to bring attention to how the altruism surrounding organ procurement too often allows hospitals and OPOs to flout the law.
•••
Organ procurement and transplant surgery are big business. In 2020, the cost of one heart transplant was more than $1.5m, a liver more than $800,000, a kidney nearly $500,000.
In March, the US government announced that it planned to break up the United Network for Organ Sharing (UNOS), the congressionally created non-profit that has administered organ procurement in the US since 1984.
For years, patient advocates have railed against OPO behavior and operation, citing UNOS’s failure to meet the nation’s needs.
The organization holds a $6.5bn annual federal contract – funds that largely come from fees patients pay to be added to the organ recipient waiting list. (About 20% of the total cost of transplant surgery is required for waiting list registration.)
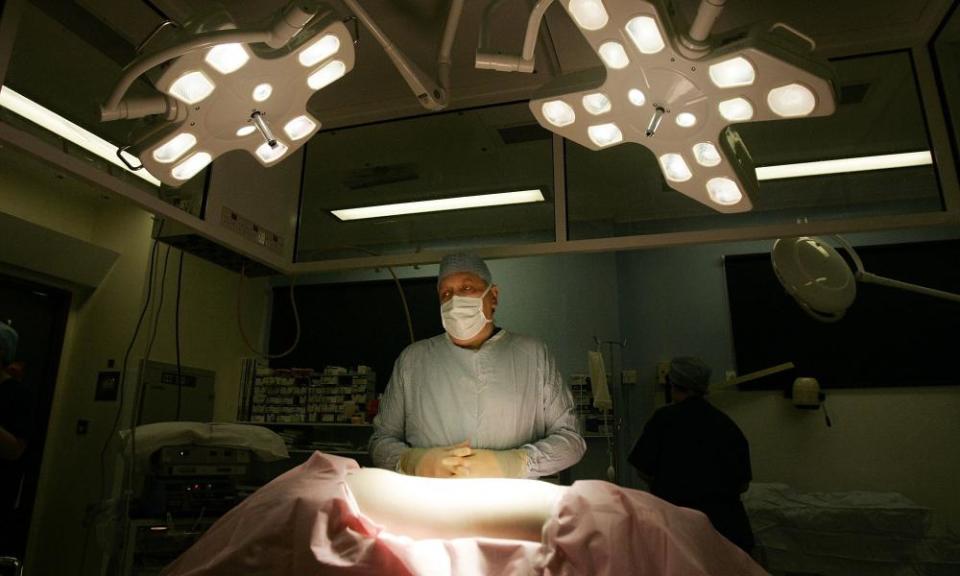
Hospitals are paid for the organ procurement organizations’ use of their operating rooms and surgical resources. Donor Network West – which is overseen by UNOS – received in excess of $81m in earnings the year after Brittany’s death.
Some of the UNOS issues that have become too big for even the federal government to ignore include the woeful inadequacy of available organs to meet the needs of the country’s ill. Each day, 22 people die while waiting for a donated organ. Nationally, more than 100,000 people are on a waiting list for hearts, lungs and other organs, a majority of them waiting for kidneys (a patient can wait for an average of 685 days to receive a kidney, 236 for a liver, and 213 for a heart).
In California alone, there are 23,000 patients on the list. The system is rife with inequality, with low-income and minority patients receiving fewer donations than their white counterparts. African American patients, for example, experience heart disease at a higher rate than white patients and are diagnosed with kidney disease four times as often, and yet they have a 10% lower likelihood of transplantation.
“Historically, we’ve excluded the poor,” Michele Goodwin, professor of constitutional law and global health policy at Georgetown Law School, told me about the US medical system. “Historically, we have discriminated against people of color. So we’ve not actually practiced inclusive medicine.”
In 2018, Goodwin wrote about a highly publicized case of a 13-year-old girl, Jahi McMath, who was declared brain dead by Children’s Hospital Oakland in 2013 after a routine surgery for sleep apnea. Complications after surgery, including excessive blood loss, led to the hospital’s determination. The family balked at the designation, staging a protest outside the hospital and a national media campaign.
McMath’s family appealed to a non-profit organization that raised funds to move the young girl to New Jersey, where religious exemptions to the UDDA are legal. She was kept on organ support for nearly five years. All the while, her body grew and she began menstruating.
Goodwin wrote that McMath’s family was protesting the treatment of their daughter and themselves as much as they were contesting the brain death diagnosis. After the surgery, the girl had begun to bleed excessively. When Nailah Winkfield, Jahi’s mother, pointed it out to doctors and staff, she was ignored or told that it was normal.
Winkfield, who is Black, told the New Yorker in 2018: “No one was listening to us, and I can’t prove it, but I feel in my heart: if Jahi was a little white girl, I feel we would have gotten a little more help and attention.”
Politics, too, plays a pronounced role in how medicine is delivered. “We’re in a very curious political moment,” Goodwin told me, “that’s been influenced so deeply by religion in a way that would have been shocking and unheard of 50 years ago. As we think about how we understand birth, how we understand death, these are questions that now have a political-religious shroud over them.”
•••
Everyone agrees that a family meeting was held on 20 November, three days after Brittany was admitted to Fresno community hospital. Mike and Kaylee both say that everyone, including his ex-wife, Shawna, decided to give Brittany 30 days to fight. Mike was prepared to remove Brittany from life support after that date.
Both “mother and father” are noted as “surrogate decision-maker” in the medical records on the 20th. The day before, fearing the worst, Mike had set up a GoFundMe account to raise money for Brittany’s funeral. (Shawna O’Connor did not respond to repeated requests for an interview.)
But a note in the medical records, written two days after the meeting took place, says: “Family meeting … showed parents with different opinions on management.” The note states that Shawna “believes patient would not want to be kept in this condition because of continued suffering”, and says that Shawna and Brittany “watched the Terry Shivo [sic] case together and they stated none of them would want to [be] kept alive in that condition”.
Terri Schiavo’s case has become a touchstone for families who are faced with brain injuries that render a patient unconscious, unable to make their own medical decisions. It remains a landmark in social awareness of artificial organ support, consent, and guardianship. And it highlighted the role that religion plays in medical care provisions: the US Conference of Catholic Bishops, which governs the more than 600 Catholic hospitals in the country, changed its rules after the case. In Catholic hospitals, artificial nutrition and hydration is now “comfort care”, according to the organization’s ethical and religious directives. Discretion to remove it is left to the hospital director, not the family. Enforcement of this hierarchy is up to the local bishop.

At noon the day after Thanksgiving, six days after Brittany was admitted, Mike called to speak with the doctor (“Dr. Harp NEVER called me,” Mike wrote on a copy of the medical records he received after Brittany’s death) and was told to come to the hospital.
What followed, everyone agrees, was a series of interactions that involved a lot of yelling. Mike told hospital staff that he would “shove the law so far down your throats that you’re the ones who will need the tube”. The doctor wrote that Mike “refused to believe that she was dead” and a staff member wrote that Mike was “verbally threatening and aggressive”, stating that “people in far worse conditions have come back” and that he was not going to allow Brittany to be removed from life support “because my faith has told me she is going to make it through this. I’m not letting her die.”
At 4.18pm, the medical records state, the Fresno police department came to the unit at the behest of the hospital.
Dr Lynn Burnett, who worked for Fresno community hospital and is now deceased, wrote an extensive explanation the same day, 24 November, for why Mike should have no say in Brittany’s care: “In this case, the Patient’s Father has voiced Religious objections to discontinuation of physiologic support. His objection, however DOES NOT pertain to religious practices, but rather, to the medical determination of Death by Neurological Criteria.”
Crucially, he then wrote: “Given these events, it is Ethically Appropriate NOT to tell the Patient’s Father about the plan for organ recovery until after such has been accomplished.”
A note in the medical record states that “organ donation was never brought up to the father by any hospital staff”.
The day after Brittany’s funeral, which Shawna did not attend, Mike visited his ex-wife with a camera. She appeared tall and lean in the video, wearing a black shirt and pants. Her hair was short, blond and tousled. She was looking at Mike, not the camera. “There was a discrepancy… I did not want a donation and Shawna knew that,” he said.
“Well, yeah, I knew that,” Shawna said. “They just kept pushing me and they would push me and they got us separated. They took me into a room at one point and said that I was the logical one and that they were no longer going to deal with you at all.”
•••
Fresno, in the center of the San Joaquin Valley and the state, is home to nearly 1 million people. The sprawling city’s backdrop, when the air is clear, is the white-capped peaks of the Sierra Nevada mountains. Windswept fields surround the city. Clouds of white blossoms adorned acres of almond, apple and plum trees when I was there.
Mike, Brittany, and Kaylee have always lived in Fresno – and all four have struggled with the addiction, health issues, and underemployment that are endemic to the city.
Fresno is characterized foremost by agriculture, land development, and disparity – economic, health, educational, racial. The haves traditionally owned and developed the valley’s land and the have-nots farmed and built it.
Perennially on the list of cities with the highest rates of extreme poverty, social inequality, drug use, suicides, and overdoses, Fresno has been plagued with poor health outcomes for decades.
“Old mayors, new mayors have called it ‘a tale of two cities’, but no mayor has been able to make the divide less stark,” Mark Arax, a Fresno native, wrote about the city in the New York Times last summer. “In the span of 15 miles, from the wealthy subdivisions and megachurches of the Northside to the meth-fueled hustle of the Southside, life expectancy drops 20 years.”
Even if it’s one out of a hundred chances that your daughter is coming back – what father wouldn’t take those odds?
Mike O’Connor
On Valentine’s Day last spring, I pulled into the dusty driveway of the sober ranch where Mike O’Connor had been living for nearly 12 months, working as a house manager. He’d been sober for several years but found the work rewarding.
The ranch was on the outskirts of Fresno, a vast canopy of orchards lined the surrounding fields. A dry wind pinwheeled the leaves on the palm trees behind the house.
Mike and his lawyer, Thornton Davidson, were scheduled to attend a mandatory settlement meeting in a week, and I wanted to see them before any accompanying non-disclosure agreement prevented them from talking about the case. (They chose not to settle.)
“My main problem is,” Mike said, “it’s a hospital where you’re supposed to try to save people. They weren’t trying to save her. They were trying to preserve her.
“Brain dead doesn’t mean soul dead,” he said. “So, in my opinion, even if it’s one out of a hundred chances, which is what they told me, that your daughter is coming back … what father wouldn’t take those odds?”
He said the hospital and organ procurement staff had befriended Shawna. “If they wanted to comfort her and make her feel great, great. She needed that at that time. But they didn’t do it out of love. They did it for money. They did it because they wanted body parts.”
Even if Mike felt that his daughter had had enough time to fight, he would never have consented to organ donation because Brittany had told him she did not want to be a donor.
When she was eight or nine, Mike said, they saw a TV commercial for organ donation. Brittany asked what it was and after Mike told her, they agreed that “we, neither of us, wanted to be donors”, Mike said. “And one of the main reasons was, she always said: ‘My heart is your heart, Dad.’ And I said: ‘My heart’s yours too, don’t ever let them take mine.’ We wanted to be buried intact, we didn’t want to be butchered.” The phrase became an expression of familial love and commitment between them: “My heart is your heart.”
Mike had a specific reason to oppose organ donation. For four months, after he was discharged from the navy, where he served as an EMT, he worked as a procurement technician for California Blood Bank, removing organs, bone grafts, and tissue from cadavers for donation and research. “One of the reasons I’m so against it is the way it’s done. It’s brutal. I’ve literally opened up people and taken out not just bone grafts but the entire joint.” We noted that we’d both had ACL replacements in our left knees, where the torn ligament is replaced with one from a cadaver, mine a few months ago, Mike’s 30 years ago, before the navy.
It was during his time at the blood bank that he changed his mind about donation. “That’s when I found out what donation was all about,” Mike said, referring to the procurement process. “You just keep the heart alive. You keep your blood running through and they’re on a cold slab in a cold room. Somebody comes in and takes the kidneys. And the heart specialist, not coming for eight hours. You just lay there.” Mike grew distant as he talked, as if imagining what Brittany’s body was exposed to.
Mike doesn’t oppose donation for others; he’s just seen too much for him to want it for himself. And Brittany agreed.
“Why didn’t the hospital talk to you about Brittany’s diagnosis, organ donation, her death?” I asked him the next day, when I picked him up. We planned to drive to locations around Fresno that were meaningful to him, including the house where he grew up.
We were sitting in the parking lot of a distinctly California strip mall. On our right were the beige stucco walls of a nondescript drug testing office where Mike had once worked.
“Seems to me they just weren’t willing to. They had some kind of preconceived notion about me,” Mike said. Instead of staff explaining what was happening, he said, he remembers them repeating “brain dead”, assuming he knew what that meant. “They used the term to shut down any conversation,” he said.
“It’s supposed to be a choice. If you’re not there to make that choice, the person closest to you is supposed to make that decision for you,” he said of organ donation, “and that’s what was taken from me.”
The lawsuit was a way to teach Fresno community hospital and Donor Network West a lesson, sure. But what motivated Mike was preventing what happened to him and to Brittany from happening to anyone else, he said.
We sat quietly in my white rental car for a moment. “They wanted her organs. They stopped [talking to me] because it was the easiest, fastest way of getting the organs,” he said. “They gave it all away. Everything. And I have thought about it every day for five years, trying to find another reason, so that I could be OK.”
“What is it you come back to again and again?” I asked.
“Could I have saved her? Was she really dead? Am I gonna pay for this in the long run? When I get to heaven, is God gonna say….”
“So it’s made you question your own salvation?” I asked.
“Is it a mortal sin? Could it be considered murder?”
“You think you’re responsible for your daughter’s death?” I asked.
“I don’t know. I think I might be. A lot of times I wish I was anybody but myself.”
•••
Every expert I spoke with about the Uniform Determination of Death Act expressed their concern for the protection and improvement of organ donation.
“The biggest thing at stake is public trust in medicine and in transplantation,” Brendan Parent, a professor of population health and surgery at New York University’s Grossman School of Medicine, told me. “The framework we have created for donation is that we all get to decide what happens to our bodies after we die,” Parent said. “Organs are gifts and we need permission.”
It is because they are gifts that the system needs to be transparent, just, and clear to the public, he told me. Any actual or perceived injustice, either in how brain death is diagnosed or how organs are procured, can harm an organ donation system already under great pressure.
The idea that brain death was created to facilitate organ procurement means to some groups that “something nefarious is going on”, Parent said. Fear of being an organ donor persists often because many believe that healthcare professionals will not try to save a designated donor’s life.
The fear can be rooted in medicine’s very real unjust and paternalistic history. “We can’t just say that it’s a myth,” Parent said, referring to the sterilizations, unauthorized testing, and neglect of disabled people and people of color that have plagued modern medicine. The Tuskegee syphilis experiments are one example. But the fear is also rooted, he said, in “the pressures of the organ donation system”, amid a dire shortage of viable organs.

Parent’s concern is that any effort to discredit the experience of the loved ones, like Mike, who might be traumatized by how organs are procured could lead to further erosion of public trust. He said understanding and listening to questioning families can only improve the entire organ procurement system.
Goodwin reiterated a need to strengthen the organ donation process, for the sake of the many thousands of people on the waiting list. The best way to do so, in her estimation, is to make healthcare more equitable. “More inclusive medicine actually would mean that we were more efficacious overall,” she said.
Thaddeus Pope, a lawyer and professor at Mitchell Hamline School of Law in Minnesota, has been advocating for the revision of the UDDA for several years, urging the Uniform Law Commission – the national non-profit that works to make state laws as uniform as possible for legal consistency – to take up revision of the criteria used to determine brain death. His objective, and that of his colleagues and co-authors, he said, has been to improve equality and the number of organs donated. (I first learned about Brittany’s case from Pope’s website; at the request of Mike’s lawyer, Pope has since become a designated expert witness on the issue of ethics for the case.)
I met with Wesley Ely, co-director of the critical illness, brain dysfunction, survivorship (CIBS) center at Vanderbilt University Medical Center, in the vaulted, book-lined anteroom of the National Academy of Sciences in Washington DC in May. “I think it’s important to optimize organs for the patients who are waiting, but we can’t do that at the expense of our ethical and moral values,” he said. He told me plainly that he believes in brain death as currently laid out in the UDDA. But he acknowledged that it was difficult for some families to understand the diagnosis. He also sympathizes with patients who are hesitant donors.
Ely said that he, as the former medical director of a lung transplant program and a longtime practicing critical care doctor, has been faced with explaining donation to families after brain death. He emphasized that it was possible to explain the process to patients’ hesitant loved ones: “If you take time, hold their hand, walk them through the notion of why the body can’t live a meaningful life, then they can begin to understand that if it was the patient’s preference, this should be consented to.”
It is a weird experience to walk in, see someone’s cavity opened and organs taken out. And I don’t think we should ever get over that
Dr Wesley Ely
Still, organ procurement is an emotionally complex process. “It is a very weird experience to walk in, see someone’s cavity opened, and all these organs taken out of it. And I don’t think we should ever get over that,” Ely said.
“There is a beauty to giving organs to another person. But it’s not for everybody.”
•••
On the phone, Brittany’s sister, Kaylee, has a bright, tinkling voice. She is the mother of two children, seven-year-old Tommy and six-month-old Karter.
“I don’t know why it was such a thing with her, but she always said that organ donation was a scam,” she told me about Brittany, who was seven years older. “And I was like, ‘What do you mean? You’re selfish.’ It’s crazy how she never wanted [organ donation], and that would end up killing her.”
When I asked why she described her father as the only “reasonably minded” parent, she said that her mother was very sick. “She’s been addicted my entire life. But then there’s mental illness. It’s been really hard to grow up with that. It was really hard on Brittany.” In many ways, she says, it was Brittany who raised her.
When I told Kaylee that Mike believed Shawna had been coerced by the hospital staff, she agreed. I asked her why. “Organs are valuable and Brittany was only 26, my age right now. There’s definitely not enough organs for everybody in the world,” she said.
She also thinks the EMTs, the hospital, the police and the organ donation staff looked down on Brittany and her father. The police knew the house Brittany was living in. There was addiction. Her father was overweight. “I felt like they thought we were some white trash, you know, some low-income family. I mean, who’s gonna fight for her?”
Kaylee is heartbroken. “I was 20 years old and just out of my mind about it.”
To this day, she doesn’t know who’s to blame for her sister’s death and donation. But she now knows that she’ll never donate her organs.
•••
Current tests to evaluate brain death include putting ice water in the ear, removing the patient from a respirator, and shining light in the eye; the goal is to demonstrate that there’s no response to external stimulation, no brainstem reflexes, and no ability to breath without assistance. No patient who has been accurately diagnosed as brain dead has ever recovered.
The UDDA, which stipulates criteria for brain death but does not state specific tests that should be used, notes that doctors rely on “accepted medical standards”. Doctors have been trusted to use the necessary criteria to make their determinations.
But after nearly 40 years of relative stability, the UDDA has come under scrutiny.
Several high-profile cases like Brittany’s, in the US and abroad, have rallied families, allies, and religious groups to argue that brain dead patients are actually not dead. The case of Jahi McMath, the young girl who remained on organ support for five years despite a brain death designation, was watched by the medical community with great attention; it upended the understanding that the bodies of the brain dead would soon begin to decompose. (Current testing does not examine the functioning of the pituitary gland or the hypothalamus, parts of the brain that kept McMath’s body from decomposing.)

Lawyers, doctors, and bioethicists began to call for a revision of the brain death designation to bring bedside testing in line with the UDDA, to make it more uniform, to increase clinicians’ confidence and the public’s awareness of what brain death is. The hope was to save families and healthcare providers from the doubt and distrust that a lack of uniform criteria can garner – and to save everyone the financial and emotional destruction of lawsuits.
The Uniform Law Commission’s early meetings proved contentious, revealing a wide array of ideas about what changes should be made to the definition of brain death, some suggesting more rigorous testing, others less. Still others proposed leaving the old standards in place. Earlier this year, a draft introduced at a meeting in Hawaii included a universal religious exemption and more clinician discretion.
The lack of consensus among committee members caused ULC to postpone their projected date for recommended legislation, originally set for 2023, an unprecedented additional year.
Cases like McMath’s may be few but their attending publicity – whether in legacy media or across religious or rightwing channels – influences millions and can undermine established medical paradigms. And the impact that the UDDA has on transplantation is enormous.
•••
When life ends is particularly contentious in an environment where half the population’s medical rights are held hostage by the politics of when life begins.
The conservative lawyer James Bopp Jr is most responsible for the legal assault on abortion access that has taken place since the passage of Roe v Wade in 1973, and for the decision being overturned in the summer of 2022. He was at the forefront of litigation that led to the institution of waiting periods, age limits, and notification laws that incrementally limited who could receive an abortion, where and when.
But it is his current work on the Uniform Law Commission’s review of the UDDA that has brought him renewed media attention.
When I spoke to Bopp this summer, he was genial and candid. Publicly he’s been clear that he sees abortion and the debate surrounding brain death to be on the same continuum because, from the moment of conception, the fetus “does not yet exercise functions we identify as human”. Neither does the brain dead patient, and therefore, like the fetus, according to Bopp, they must be protected.
He told me that he agreed in the 1980s with the UDDA’s criteria for brain death, and, as general counsel to the National Right to Life Committee, a non-profit anti-abortion group with chapters in all 50 states, he urged the organization to support it.
“They asked me, ‘Does this meet our criteria that every human life has inherent value from fertilization to natural death? Does whole brain [death] determine natural biological death?’ I said yes.”
But to Bopp and his allies, new information has emerged: testing for death of the “whole brain, including the brain stem”, as stated in the UDDA, is not (and never has been) consistently conducted throughout the country. And cases like that of McMath have shown that other brain functions not addressed by existing testing, such as those of the hypothalamus and pituitary, may continue after the death of the rest of the brain.
Bopp’s concern is that biological death may not occur at the time that all brain function ceases. Others on the Uniform Law Commission, where he is a member of the drafting committee, have focused instead, he told me, on consciousness. Most families, when they understand that their loved one will never be conscious again, decide to remove organ support, or “pull the plug”.
But Bopp thinks this is unjust. Unlike those who see consciousness as essential to life, patients like McMath, and perhaps Brittany O’Connor, in the eyes of Bopp and other “pro-life” advocates, are disabled. Severely disabled, yes, but too often “directly targeted” by those with a “relative value of human life”.
What Bopp calls integrated function, Joseph Eble, a physician and president of the Tulsa, Oklahoma, Catholic Medical Association, calls the soul.
Related: Nearly half of American adults faced medical bill issues in last year – survey
A prolific writer for Catholic publications, Eble has appeared on a host of Catholic TV shows, podcasts, and radio shows to talk about his interpretation of brain death. “The human person is the substantial union of the body and soul,” Eble said on the St Philip Institute Podcast last year. “The soul is the principle of integration of the body. Its absence is evident, despite its invisibility. When the body is no longer integrated, [it is in] a state that is indicated by decomposition.”
Hugh Brown, executive vice-president of the American Life League, a Catholic non-profit with a $3.5m annual budget, recently weighed in on brain death on an anti-abortion Catholic podcast hosted on more than 200 channels of Relevant Radio, a Catholic network. Brown told the host that protecting those with a brain death diagnosis was as important as protecting what he calls the unborn because “during the first six weeks of pregnancy, our body lives without a brain”. Brown’s belief is that the brain is not necessary for human life.
It might be easy for some of us to shrug at Brown’s definition of life, or Eble’s formulation of body-soul integration, but similar ideas about brain death exist within today’s medical journals.
Alan Shewmon, a pediatrician and professor emeritus at the University of California, Los Angeles, has argued against the brain death designation for decades, becoming a hero with credibility to many on the religious right. In 1998, he published a study that claims a significant number of brain dead patients retained enough blood flow to the brain to prevent its deterioration. Shewmon advised McMath’s family, finding that McMath had what he calls “chronic brain death”, not a terminal ailment.
When I asked Bopp what would happen if every hospital in the US were forced to comply with his formulation of brain death, keeping brain dead patients on organ support indefinitely, he chided me for putting a price on human life. And yet, when quality healthcare is a luxury in the US, when only those who can afford organ transplants get them, it is evident that we already do.
•••
Thornton Davidson, Mike’s lawyer, is surprisingly accessible thanks to a puckish, wry wit. We met in the conference room of his modest office on Shaw Street in Fresno the day after I visited with Mike.
We were discussing the “trolley problem”, a thought experiment that goes like this: there is a runaway trolley on a track. You are a bystander and see that a nearby switch would allow you to divert the trolley from its current course, which will undoubtedly kill five people. But if you divert the trolley, the one person on the alternate track will surely be killed. “What are you gonna do?” Davidson asked. “You have a choice: kill one person to save five? They weren’t going to kill [Brittany], but the argument would be: give up the organs and save five people or bury her with her organs, which will rot.”
Davidson waited a beat. “But that’s not what the case is about.”
“What’s the case about?” I dutifully asked.
“Love,” he said.
“The legislature,” he said, “made it so that people who were the closest, who had the closest bond, had the authority to make this decision in the absence of what the person dictated.
“But the law also anticipated that where you had more than one person, you could have a conflict. And so the law doubled down on the protection of that familial relationship. And it said, ‘It’s got to be a majority.’”
In Brittany’s case, the majority should have been both Mike and Shawna, Brittany’s parents.
In this way the legislature created a “failsafe”, so that if there was not unanimity among the parties, the organs would not be removed from the body.
“That’s why the case is about love, because this is one of the rare instances where the law protects that familial relationship.”
The hospital and Donor Network West might say that five lives are ethically more valuable than one. They might say Mike wasn’t “reasonably available”, despite having him escorted off the premises by a policeman, that he was a threatening voice at his daughter’s bedside. They might even say that it was up to Shawna to notify Mike of her decision. But what matters to Mike, and probably to the judge who will preside over the trial, is what the law says.
In the third week of September, the fifth circuit judge threw Donor Network West out of the lawsuit, but kept Fresno community hospital. According to Davidson, this showed how the courts “bend over backwards to protect the organ procurement industry” and allow them to flout the law.
Davidson planned to continue with the trial against the hospital, and says he’s not given up on holding Donor Network West accountable.
•••
Mike and I drove east to the cemetery in Clovis, California, where Brittany is buried. Cedar trees line the open field and colorful plastic flowers dot the stones, which are flush with the dry ground. Nearby the 168 bends east before heading north, out of town, and into the Sierra national forest.
Mike told me that he would like a clause added to the California Uniform Anatomical Gift Act that further codifies unanimous agreement for organ donation among decision-makers. Brittany’s clause, he imagines. “That would be kind of cool, to have my daughter’s name on it for as long as there is a clause, for as long as there is donation. She’ll be remembered for ever.”
In the last week of September, the Uniform Law Commission paused its review of the UDDA. “The result of this pause is that, although we will continue to hope mid-level principles will become apparent,” the email, sent to the commission’s members and observers, stated, “no further drafting committee meetings will be scheduled at this time.”
I followed Mike to Brittany’s stone and watched him dust a bit of dirt and grass from it. He designed the marker: a teal butterfly is on either side, just below Brittany’s name. Between them, there are two hearts, one with her picture and the other with the words “We find the trees behind the trees”, the lyrics to a song he and Brittany made up when she was young.
Across the bottom the marker reads: “Loved By All.”
• In the US, you can call or text the National Suicide Prevention Lifeline on 988, chat on 988lifeline.org, or text HOME to 741741 to connect with a crisis counselor. In the UK and Ireland, Samaritans can be contacted on freephone 116 123, or email jo@samaritans.org or jo@samaritans.ie. In Australia, the crisis support service Lifeline is 13 11 14. Other international helplines can be found at befrienders.org
This article was supported by The Economic Hardship Reporting Project

 Yahoo News
Yahoo News 
