Hospitals in small-town and rural America warn they are drowning in Covid cases
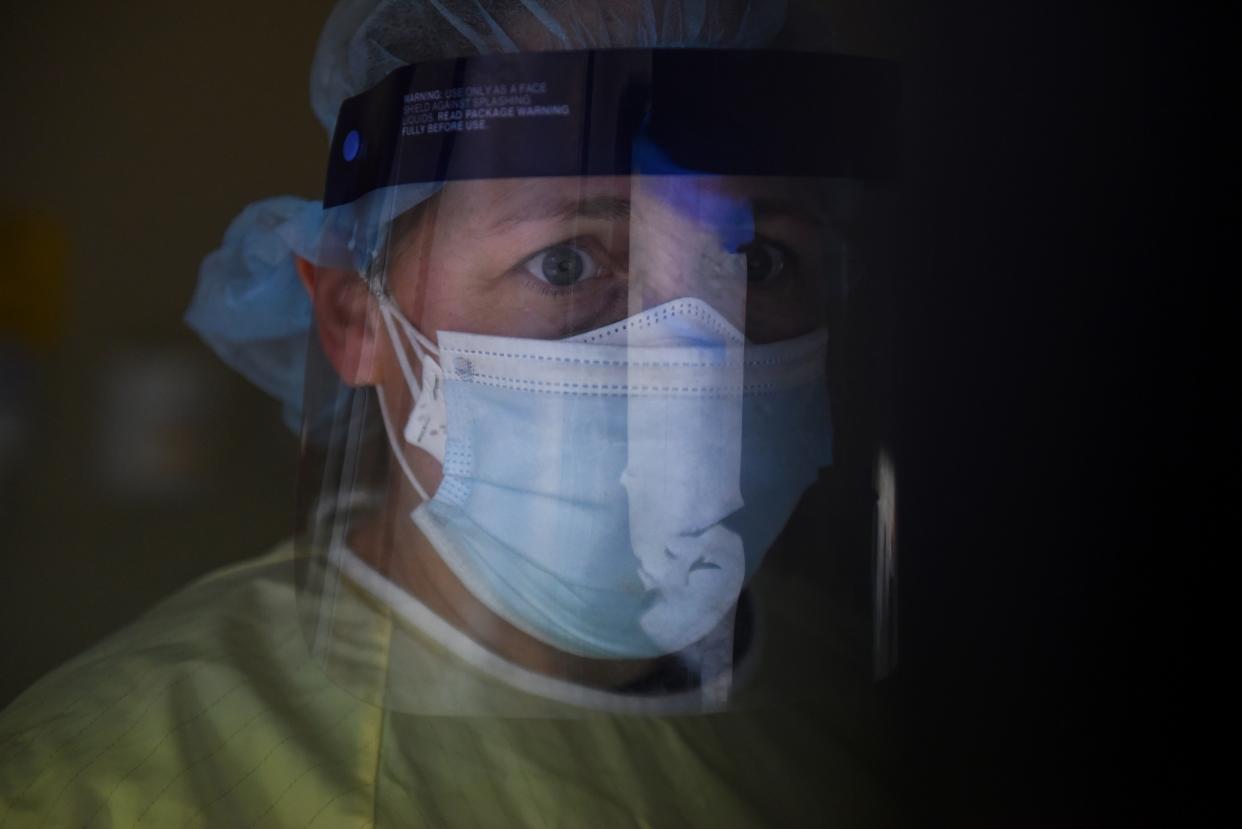
After pounding the country’s biggest cities in the spring and summer months, the coronavirus has now caught-up with rural and small-town America, where officials say they are drowning, and fast.
According to Reuters’ interviews with more than a dozen medical care providers and public health officials in the country’s heartland, many hospitals are severely lacking in beds, equipment and - most critically - clinical staff, including specialists and nurses.
And while Covid-19 cases and hospitalisations have spiked all over the United States, the Midwest - which stretches from Ohio to the Dakotas - has been particularly brutalised.
Reported case rates are more than double that of any other region in the United States, according to the COVID Tracking Project database, with more than a thousand cases reported on average per day in states such as North Dakota, Wisconsin and Kansas.
While in New York’s worst week in April - with business shut and widespread panic among the public - the state never averaged more than 500 new cases per million people. California never surpassed 253.
The Midwest’s hospitals have told Reuters they’re now at capacity or nearly so, and most have attempted adaptations to working hours and repurposed wings. Others have crammed more patients into single rooms.
In rural Kansas, one local hospital had to call on the support of larger hospitals for access to Intensive Care Units, as cases soar in the state.
Miller, a chief medical officer at the Kearny County Hospital who doubles as the county’s health officer, told Reuters he couldn't find a single ICU unit to treat one 30-year-old patient, who neared death.
Somehow, Miller said, the patient regained a pulse, and was dispatched in an ambulance to the larger facility about 25 miles away. He stayed behind to pray with the man’s family, whom he knew “very well” from Lakin, a town of just a few thousand people.
Facilities like Kearny, known as “critical access” hospitals, weren’t made for this kind of health emergency.

The Midwest’s hospitals have told Reuters they’re now at capacity or nearly so
REUTERSThey are often sparsely funded, mainly provide basic or emergency care to residents who live long distances away from bigger medical centers, and have had trouble convincing both conservative patients and politicians about the dangers Covid-19 poses.
Donald Trump has himself stood shoulder-to-shoulder with Midwesterners at campaign rallies, and treated masks as a matter of personal choice.
Kirsti Noem, South Dakota’s governor, has meanwhile refused to mandate mask-wearing across her state, and has not imposed restrictions on businesses or public gatherings, saying she would leave such matters to “individual responsibility.”
Some medical officials and hospital staffers have said it’s hard to reconcile such laissez-faire policies with the sickness and suffering they see.
“There’s a disconnect in the community, where we’re seeing people at bars and restaurants, or planning Thanksgiving dinners,” said Dr Kelly Cawcutt, an infectious disease doctor at the University of Nebraska Medical Center. As health workers, she said, “we feel kind of dejected.”
“Everyone [is] continuing to go about their lives [but] we sort of feel like we’re drowning,” said Dr. Alison Schwartz, an infectious disease physician at SSM Health in Janesville, Wisconsin.
A patient there recently refused to believe Covid-19 was a serious threat, even as it consumed him.
When he died, “the family did not want to admit this patient had died of Covid, because they didn’t believe Covid kills people,” said Dr Schwartz.
All told, the coronavirus has claimed the lives of more than 256,000 Americans, and infected at least 12 million - more than any other nation.
And yet, as doctors have learned more about the disease, and vaccine developments provide some hope for the long-term, health officials such as Miller believe that “the worst is [not] here yet”.
Reporting by Reuters
Read More
Trump adviser Boris Epshteyn tests positive for coronavirus
Congress braces for Biden's national coronavirus strategy
Texas grandparents send life size cardboard cutouts to family
Nurse dies of Covid after leaving retirement to teach students

 Yahoo News
Yahoo News 
