‘Measles is the canary in the coal mine’: World’s most infectious disease makes unwanted comeback
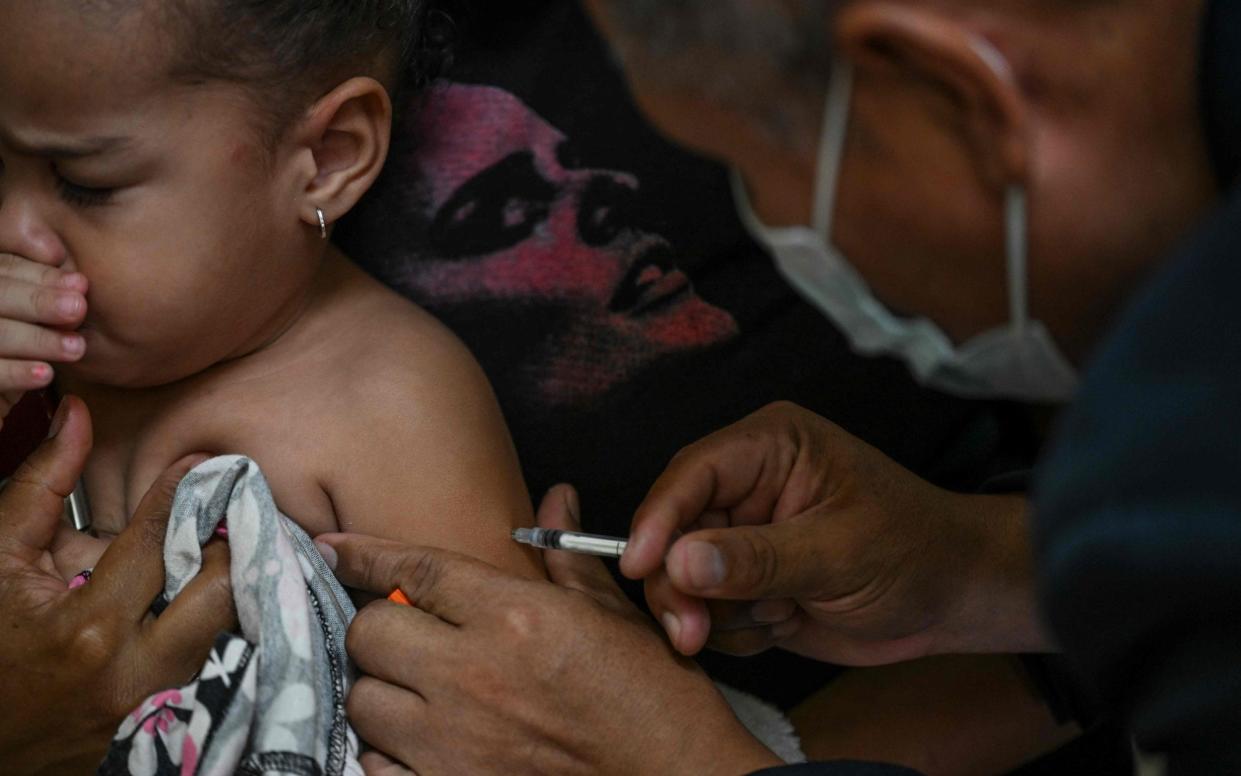
Long considered the world’s most contagious disease, measles is making an unwanted comeback. Cases of the childhood illness plummeted during the height of the pandemic – the result of social distancing and mask wearing – but that trend is now rapidly reversing.
“We are starting to see cases of the disease tick up globally,” says Dr Patrick O’Connor, a measles expert at the World Health Organisation (WHO).
“A disruptive outbreak is classed as one where there are more than 20 cases of the disease per million people, and every month we are seeing more and more countries fall into that category.”
Before the introduction of a measles jab in 1963, the disease infected millions worldwide and killed an estimated 2.6 million people every year, mostly children under five. Vaccination proved to be a game-changer; as access to doses rose, the prevalence of the infection dropped and some countries, including the UK, even succeeded in eliminating measles.
Yet these hard-earned gains have been undermined by the pandemic, which forced countries to suspend immunisation services and redirect health resources to responding to Covid. As a result, years worth of progress in tackling measles have been wiped out.

Indeed, in 2019, before Covid hit, 86 per cent of all children under the age of one had received a first dose of measles vaccine by their first birthday, according to the WHO. But by 2021, this had fallen to 81 per cent – the lowest number since 2008.
Roughly 67 million children missed out on shots over this two-year period, while vaccination coverage fell across 112 countries.
The consequences of this are now starting to crystallise. Dr Gunter Boussery, a senior health specialist for Unicef who works across South Asia, said outbreaks of measles are occurring in Afghanistan, India, Pakistan, Nepal – and even in the Maldives, where it was classed as eliminated in 2020.
‘First sign of a weakening health system’
The disease is a particular threat in countries where health services are poor and hunger is rife. Set against this backdrop, measles is often one of the first diseases to rear its ugly head.
“Measles is the canary in the coal mine,” says Dr Boussery. “It’s the first sign of a weakening health system.”
While South Asia has particularly struggled with measles in the wake of the pandemic, other regions are also contending with outbreaks: from richer countries such as Austria, to middle-income ones like Russia, Turkey and South Africa.
In the UK, there were nearly as many cases of the disease in the first four months of this year as there were in the whole of 2022. The numbers are small – there were 49 cases between January and April compared to 54 in the whole of 2022 – but the disease is so infectious a single case can quickly turn into an outbreak.
Across the rich west, these numbers are only likely to rise, says Dr O’Connor.
“This summer is anticipated to see the largest number of travellers since Covid. It only takes one person who doesn’t realise they’re sick to get on a plane and they take the disease elsewhere.
Measles has an R number (the number of people each infected person can pass the disease onto) of between 15 and 20; by comparison, the original Covid virus had an R number of about 1.4 to 2.4.
Because of this, 95 per cent of children must receive two doses of the measles vaccine to ensure the viral disease is kept at bay in a population. But while there have been enormous strides in vaccinating children over the last 20 years, this golden target has never been achieved – and is now slipping further out of reach.
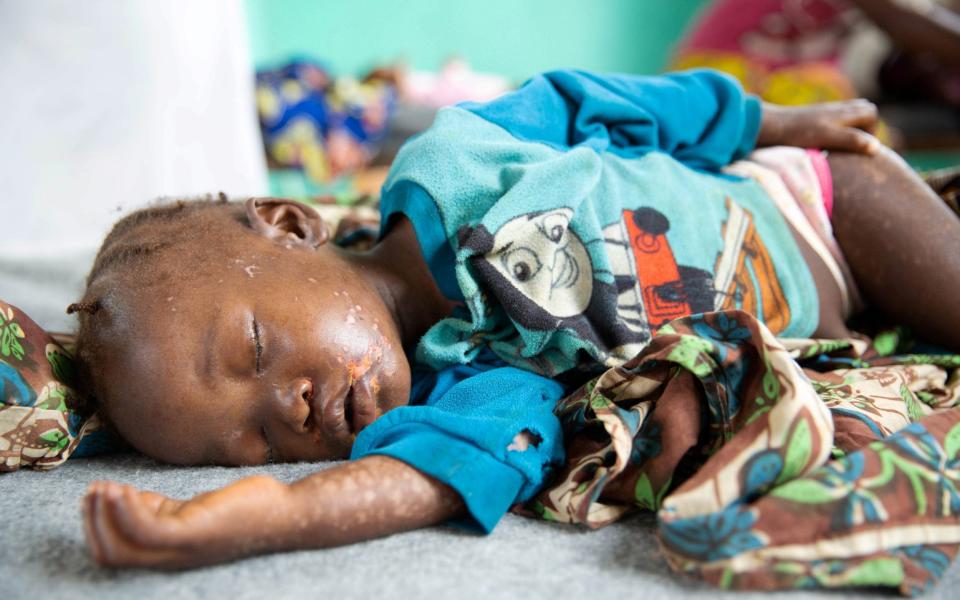
The global vaccination figures for 2022, published next month, are unlikely to show much improvement on what was reported through the most disruptive years of the pandemic, says Dr O’Connor.
There is particular concern around children missing the second dose of the measles vaccine. This jab is important as some recipients will fail to produce antibodies against the virus after the first shot – so the booster is a way of ensuring everyone is protected.
“Up to about 2019 we saw a slow but steady increase in the number of children who had had their first vaccination but for the second dose that’s flatlined and it’s hovering at 71 per cent,” says Dr O’Connor.
‘A mosaic picture’
Many wealthier countries, like the UK, may still boast relatively high levels of protection against measles among their populations, but the picture starts to change at a localised level.
In London, uptake of the measles, mumps and rubella (MMR) vaccine in children aged two years is well below the national average – in Hackney, for example, just 60 per cent of children have received both doses of the jab.
Helen Bedford, professor of children’s health at University College London, puts this down to various factors such as a mobile and diverse population that might not know where to get vaccinated or have missed reminders.
The patchy coverage seen in the UK is mirrored elsewhere in Europe, says Dr Dragan Jankovic, a technical officer for vaccine preventable diseases at WHO. While cases of measles are not as high as public health officials had feared in the wake of the pandemic, outbreaks have been reported across the continent – from Malta to Cyprus.
“We are concerned for all countries because it’s possible that coverage reported nationally is not representative of all sub-national levels and all sub-groups,” says Dr Jankovic. “There may be a particular ethnic minority or religious group who don’t get vaccinated because of beliefs or level of knowledge. In every country it’s a mosaic picture.”
At the beginning of May, the UK Health Security Agency urged parents to check their children’s vaccination status whatever their age, warning of unprotected teenagers mixing at graduation parties and festivals.
“We’ve got quite a number of children who’ve never been vaccinated, and that number is increasing year on year. If you’ve got 90 per cent uptake every year, you’ve got that 10 per cent that aren’t vaccinated accumulating every year and that’s fertile ground for measles,” says Prof Bedford.
Controlling the disease is a particularly high stakes game of Whac-a-Mole. Between 2021 and 2022, Pakistan immunised more than 90 million children in what is thought to be the largest vaccination campaign ever carried out by a single country. But despite these Herculean efforts, the country is still reporting outbreaks. Gains are fragile.
The UK knows this well. In 2016 and 2017, measles was considered eliminated in Britain, but it started spreading again in 2018 and 2019 when cases exploded around the world.
What experts fear most is a return to those pre-pandemic years: in 2019, some 207,000 children died from the disease – a 50 per cent increase from 2016; the US reported its highest caseload in 25 years; four European nations lost their measles elimination status; and in the Democratic Republic of Congo, around 6,000 children died from the disease.
However, nowhere was the tragedy of the virus more evident than in the tiny Western Pacific nation of Samoa. In an eerie foreshadowing of the Covid pandemic, the country went into lockdown in December 2019 as international medical experts battled to stem an outbreak that killed nearly 80 children in a population of just 200,000.
A combination of anti-vaxx sentiment and two fatal vaccine accidents saw immunisation rates in the country drop from around 90 per cent to 60 per cent.
More generally, vaccine scepticism appears to be on the rise globally – although whether that translates into refusal is unclear. Last month, a Unicef survey showed a decline in vaccine confidence in 52 out of 55 countries. The report suggested that a toxic combination of misleading information, declining trust in experts and political polarisation was responsible.
The UK was not included in this survey but Prof Bedford says the best way to overcome fears is to allow parents to talk their concerns through with a trusted health professional.
“If you trust somebody, and surveys show that parents trust the advice of health professionals above all other sources, you’re much more likely to follow their advice,” she says.
In some ways, the MMR vaccine is a victim of its own success – most parents have never seen a case of measles and do not know how awful it is. There is no specific treatment: just fluids, bed rest and paracetamol for aches and pains and fevers.
“Even a regular case of measles is nasty, because you get a very high temperature, conjunctivitis, a bad cough and a horrible rash. It keeps small children in bed – and it takes a lot to keep small children in bed,” says Prof Bedford.
For adults the disease is particularly serious with a hospitalisation rate of between 20 and 40 per cent, she adds.
Even if the disease does not kill it can have severe complications including blindness; measles is the biggest cause of loss of sight in children in low-income countries.
“I’ve treated children with measles and I have seen about a dozen children go blind. It can happen overnight. You feel helpless because you know that there’s nothing you can do to get their sight back,” says Dr Boussery. “It’s heartbreaking.”
Protect yourself and your family by learning more about Global Health Security

 Yahoo News
Yahoo News 
