Norovirus levels ‘much higher’ than last year, with hundreds in hospital
Norovirus levels in England are “much higher” than last year, with hundreds of patients in hospital with symptoms, figures show.
It comes amid evidence that winter pressures on the NHS are starting to grow, with one in four patients arriving by ambulance last week waiting at least 30 minutes to be handed over to A&E teams.
Health chiefs warned that the impact on hospitals from seasonal viruses is likely to be made worse by the current cold weather.
An average of 351 adult hospital beds in England were occupied last week by patients with diarrhoea and vomiting or norovirus-like symptoms, according to NHS data.
This is nearly three times the average of 126 for the equivalent week in 2022.
There were an average of 13 children with the virus in hospital each day, compared with just three at this point last year.
Norovirus is the most common infectious cause of vomiting and diarrhoea.
It spreads easily through contact with someone who has the virus or with contaminated surfaces.
While most people make a full recovery within two or three days, the virus can lead to dehydration, especially among the very young, the elderly or those with weakened immune systems.
The figures have been published as part of the first weekly snapshot of how NHS hospitals in England are performing this winter.
The data also shows that a quarter of patients arriving by ambulance at hospitals last week waited at least 30 minutes to be handed over to A&E teams.
Some 22,588 delays of half an hour or longer were recorded across all hospital trusts in the week to November 26.
This was 25% of the 89,506 arrivals by ambulance, where the handover time was known.
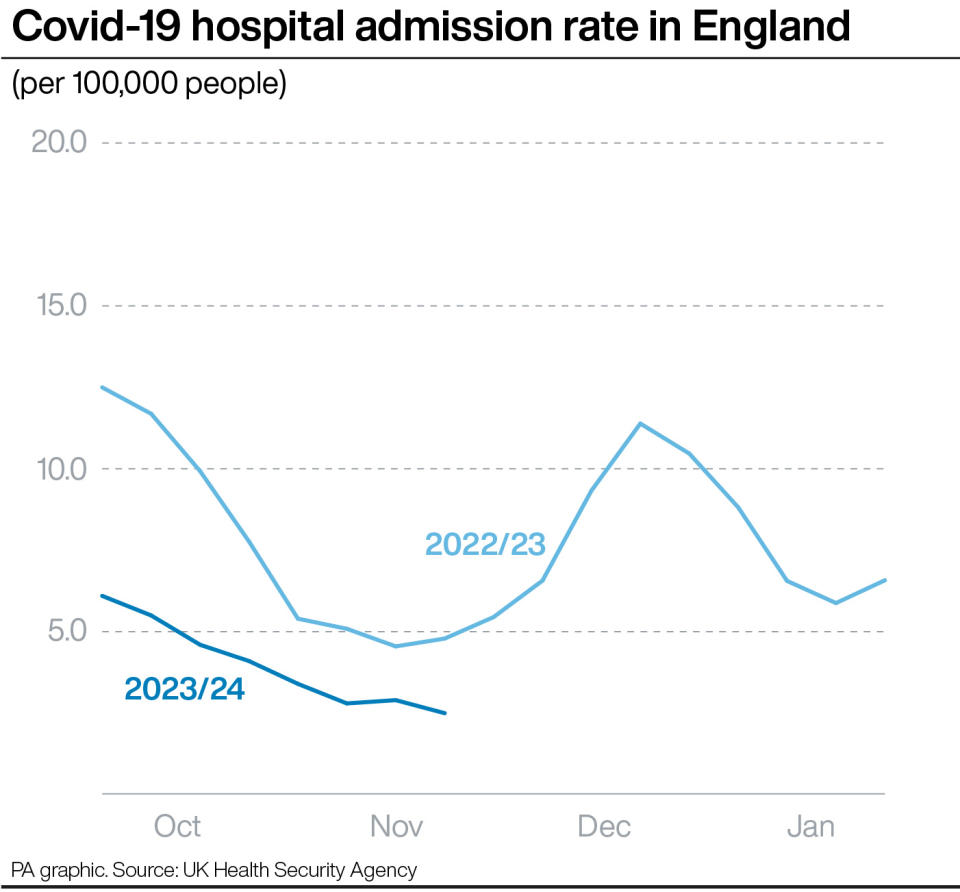
However it is lower than the 31% figure for the equivalent week last year.
Some 9% of handovers last week, or 8,239 patients, were delayed by more than an hour, compared with 15% in this week in 2022.
The number of patients in hospital with norovirus last week was almost triple the number during the same period last winter.
Norovirus is a stomach bug that causes diarrhoea and vomiting. If you catch it, make sure you rest and have plenty of fluids
➡️ https://t.co/adwr1pk3F5 pic.twitter.com/woK0ZhDrpp
— NHS (@NHSuk) November 30, 2023
NHS national medical director Sir Stephen Powis said: “We all know somebody who has had some kind of nasty winter virus in the last few weeks, and today’s data shows this is starting to trickle through to hospital admissions, with a much higher volume of norovirus cases compared to last year, and the continued impact of infections like flu and RSV in children on hospital capacity – all likely to be exacerbated by this week’s cold weather.
“The measures we set out in our urgent and emergency care recovery plan and winter preparations earlier this year are clearly having an impact, and, thanks to the incredibly hard work of staff, there has been a significant reduction in ambulance handover delays despite higher demand, almost twice the number of 111 calls being answered in a minute, and almost 1,500 more general and acute hospital beds open compared to the same time last year.
“However, it is clear that, even before we enter December, the demand on hospitals and staff is high, with more than 1,200 extra patients in hospital compared to last year, and we know that is likely to grow considerably before Christmas.”
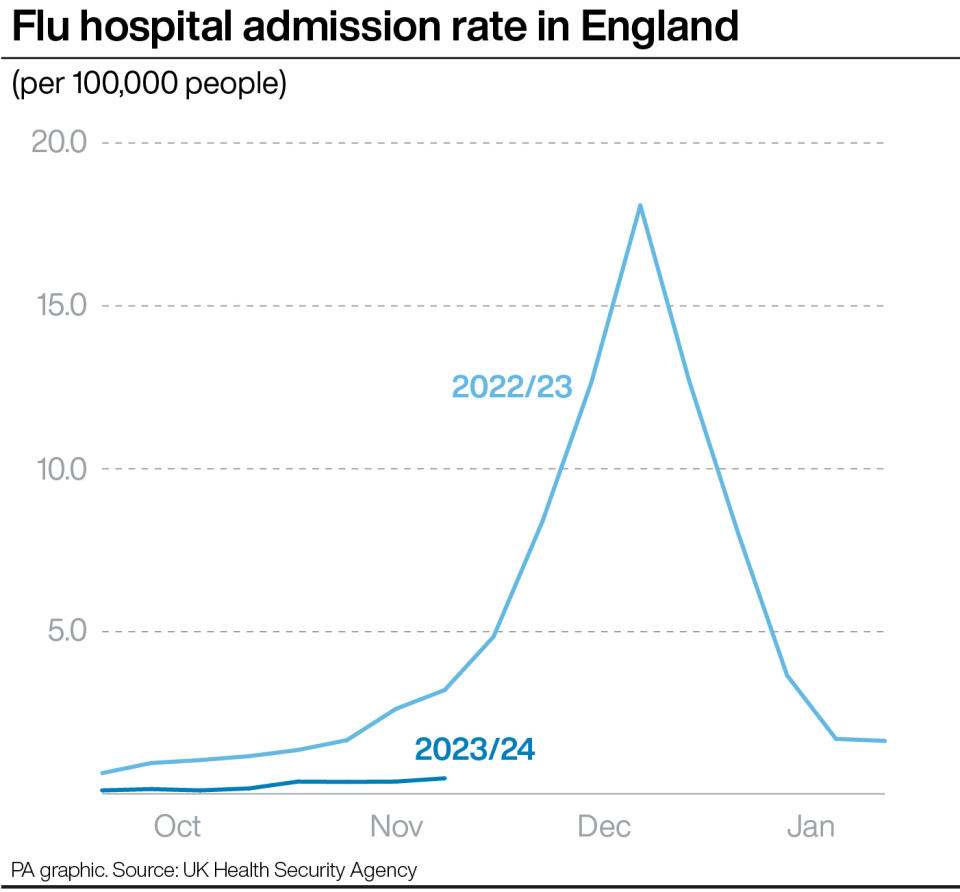
An average of 160 flu patients were in hospital beds in England each day last week, well below the average of 520 at this point last year.
Some seven flu patients were in critical care beds – again, well down on the 38 for the equivalent week in 2022.
Last year saw the worst flu season for a decade, with the outbreak having greater impact due to lower population immunity, with little or no flu circulating during the previous two winters when Covid control measures were in place.
The hospital admission rate for flu stood at 0.5 per 100,000 people last week, compared with 3.2 per 100,000 at this point in 2022.
Dr Mary Ramsay, director of public health programmes at the UK Health Security Agency, said: “Over half of those aged under 65 years in a clinical risk group and over two-thirds of pregnant women have not yet come forward for their flu vaccine this winter.
“Getting vaccinated as soon as possible will help reduce your risk of getting seriously ill with flu or Covid-19 this festive season. The vaccines can take a week or two to provide maximum protection so get booked in now to keep your Christmas plans on track.”
Details of how to book a flu or Covid-19 vaccine can be found at nhs.uk/wintervaccinations.
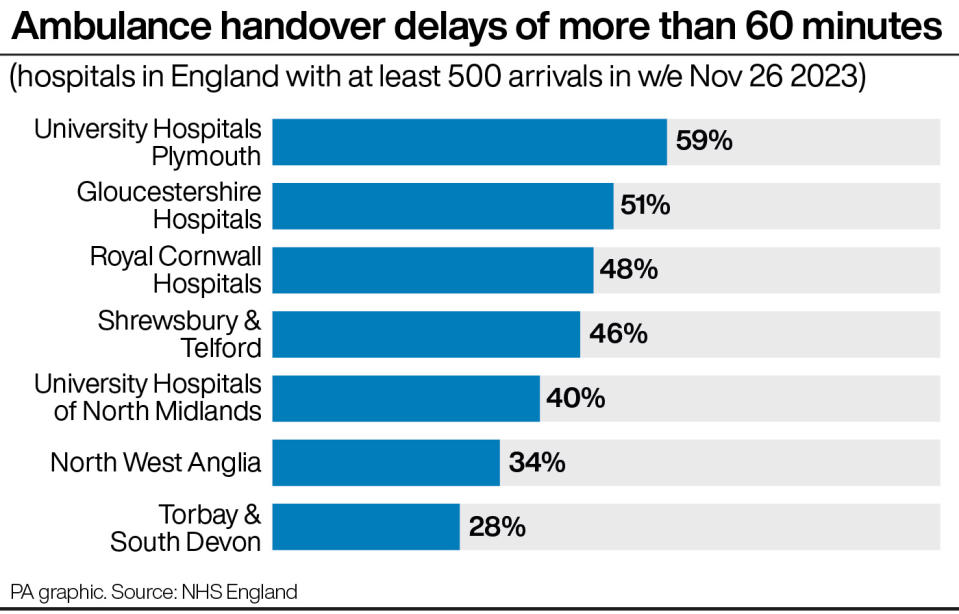
Analysis by the PA news agency shows that, among those trusts reporting at least 500 ambulance arrivals last week, the highest proportion of patients waiting more than an hour to be handed over was 59% at University Hospitals Plymouth (340 out of 574 patients where the handover time is known).
This was followed by Gloucestershire Hospitals at 51% (381 of 746 patients), Royal Cornwall Hospitals at 48% (288 of 601 patients), Shrewsbury & Telford at 46% (312 of 674 patients) and University Hospitals of North Midlands at 40% (350 of 884 patients).
A handover delay does not always mean a patient has waited in the ambulance.
They may have been moved into an A&E department but staff were not available to complete the handover.
But the figures are another sign of the pressures hospitals are facing, amid a record backlog of treatment and delays in discharging people who no longer need to be in hospital.
An average of 12,654 beds per day last week were occupied by people ready to be discharged.
This compares with 13,386 for the equivalent week in 2022.
Some 45% of patients ready to leave hospital last week were actually discharged each day, up from 42% at this point last year.
Rory Deighton, Acute Network director at the NHS Confederation, the membership organisation for the healthcare system, said the drop in ambulance handover delays was “welcome news”, adding: “It is heartening to see the NHS entering the winter period with almost 1,500 more beds than last year.
“However, bed occupancy is still high, and we are concerned about the continuing challenge of discharging patients who are medically fit to leave hospital into social or community care settings.
“The NHS also continues to grapple with the long-term impact of sustained industrial action, as well as more than 120,000 staff vacancies and a dearth of capital funding.”

 Yahoo News
Yahoo News 
