How to spot gestational diabetes: Symptoms, causes and diagnosis

Many mothers-to-be may feel concerned if they’re diagnosed with gestational diabetes, but it’s a fairly common condition affecting around one in 20 pregnancies in the UK.
“If you’re diagnosed with gestational diabetes, it means you have high blood sugar and need to take extra care of yourself and your baby,” says Emma Elvin, the deputy head of care at Diabetes UK. “This will include eating well, keeping active, and some people may need medication.”
Here’s everything you need to know.
What is gestational diabetes?
Gestational diabetes, or GD, is a type of diabetes that can develop during pregnancy. It primarily affects women who haven’t had another type of diabetes before.
“It’s a condition in which your blood sugar (glucose) level is too high during pregnancy,” says Amina Hatia, a midwifery manager at pregnancy charity Tommy’s. “It’s usually caused by the hormones your body produces when you’re expecting a baby. These hormones are vital for your pregnancy but they can stop your body from using another hormone, insulin, in the way it needs to control your blood sugar level.
Your system will usually respond naturally by producing more insulin. If it can’t, or that extra insulin isn’t working effectively, your blood sugar level will stay high and you may develop gestational diabetes.”
Symptoms of gestational diabetes
Many women have no noticeable symptoms, according to Elvin. Many of the symptoms are similar to ones experienced during pregnancy e.g. fatigue.
The most common symptoms, she says, include:
Going for a wee a lot, especially at night
Being really thirsty
Feeling more tired than usual
Genital itching or thrush
Blurred eyesight
When to see a doctor
“Usually between eight and 10 weeks of pregnancy, when you go to your first midwife appointment, your midwife will ask about things that might put you at higher risk of gestational diabetes [see below],” says Hatia.
If you’re at higher risk, you’ll be offered a test for gestational diabetes at between 24 and 28 weeks, or sooner if you’ve had gestational diabetes before (although you’ll be tested earlier if you’ve had it before).
What is the test for gestational diabetes?
The main test to diagnose gestational diabetes is a blood test known as the oral glucose tolerance test (OGTT). “This is a simple test that doesn’t harm you or your baby,” says Elvin. “After not eating or drinking anything except for water for eight to10 hours, you’ll have a blood test to measure your blood glucose level. You’ll then be given a sugary drink and have your blood tested again after two hours of resting to see how your body is dealing with the glucose.”
However, Elvin says if you have symptoms of diabetes at any time, or any concerns during your pregnancy, it’s important to discuss them with your healthcare team. “GDcan develop at any time during pregnancy, so if you develop any symptoms, even if you’ve earlier tested negative, it’s important to talk to your midwife about this,” she says.
How does gestational diabetes affect your pregnancy?
“Most people with GD have healthy pregnancies and babies, as long as it’s diagnosed and their blood sugar levels are managed,” says Amina. However, problems can arise when GD isn’t diagnosed or managed properly.
These can include, says Hatia:
Low blood sugar or jaundice in your baby
A bigger than average baby because of too much amniotic fluid
Pre-eclampsia
In rare cases, stroke, liver failure or fits
Unmanaged GD can also increase the risk of pre-eclampsia, a condition that causes high blood pressure during pregnancy and after labour. If pre-eclampsia isn’t diagnosed and monitored, in rare cases it can lead to serious complications for the mother, such as stroke, liver failure and fits, while increasing the risk of low birth weight and premature birth.
Elvin adds: “As well as the physical impact, some women feel guilty about their diagnosis or anxious they might hurt their baby. Other women have told us they feel judged by family and friends leading to feelings of shame and isolation. It can be worrying to be told you have gestational diabetes and we would encourage women to seek support from their midwife or other healthcare professional if they’re struggling emotionally.”
The causes of gestational diabetes
“We don’t know exactly why some people get GD and others don’t, but there are some things that put you at greater risk,” says Hatia.
These risk factors include:
Having had GD before
Having a large baby (4.5kg/10lb at birth) before
Being very overweight with a body mass index of over 30
Having a parent or sibling with diabetes
Being of a black, Middle Eastern or south Asian heritage
Having polycystic ovary syndrome (PCOS)
Whether you’ve had a gastric bypass or other weight-loss surgery
Women over 40 are more likely to experience gestational diabetes, and the NHS currently recommends GD screening for pregnant women over 40.
Can you prevent it?
It’s not always possible to prevent GD, but there are things you can do to reduce your risk.
“If you’re planning a pregnancy, or pregnant, it’s important to try and eat a healthy balanced diet, exercise regularly and maintain a healthy weight,” Hatia advises. “If your BMI is outside the healthy range, talk to your GP about changes you can make either before pregnancy or if you are pregnant. They can advise you on the safest option to ensure you are able to be a healthy weight for you.”
Treatments
“Once diagnosed, you’ll have extra prenatal appointments and your healthcare team will give you advice and support to manage it,” explains Hatia. “That might include changing your diet and taking gentle exercise like walking, yoga or swimming.”
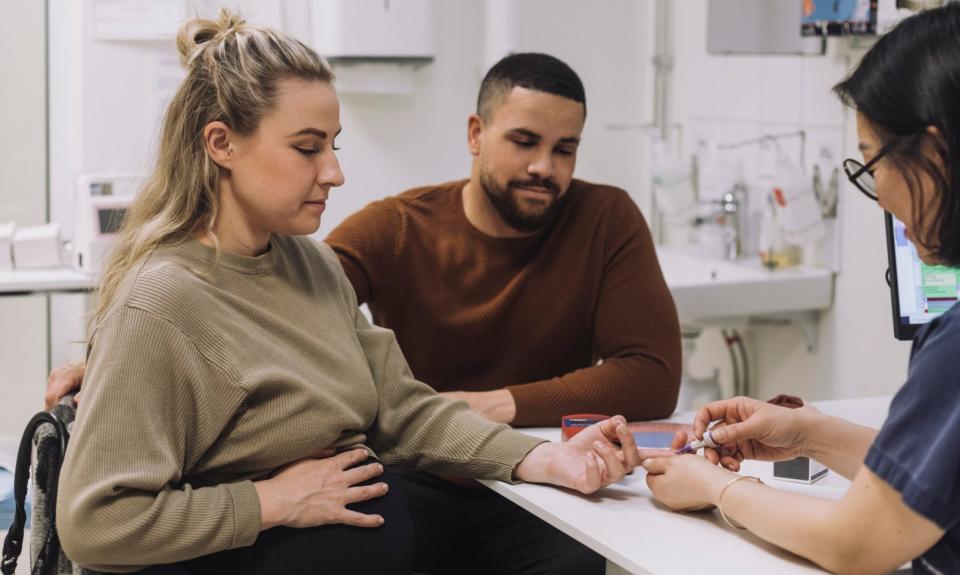
You may be advised to control your blood sugar (glucose) levels, which involves being given a testing kit, which uses a finger-pricking device and testing a drop of your blood on a testing strip (your healthcare team will advise how often and when to do this). You may also be offered a continuous glucose monitor (CGM) to wear on your skin, which sends data to your phone.
You could be given medicine or insulin injections if exercise and diet changes don’t help, which usually stop after birth. Last October, researchers from the University of Galway in Ireland discovered that Metformin, which is currently used to treat Type 2 diabetes, could be an effective treatment for GD in findings they called “a significant step forward” in managing the condition.
Does it go away after your baby is born?
Usually, gestational diabetes goes away after the birth of the baby. “Having a blood glucose test at six to 13 weeks post birth will confirm this,” says Elvin.
However, having GD can increase your risk of receiving a diagnosis of Type 2 diabetes and in some cases, GD in pregnancy can reveal existing diabetes. Fifty per cent of women who had GD will receive a diagnosis of Type 2 diabetes within five years.
For more help and advice: Visit Diabetes UK or Tommy’s
Recommended
What happens to your body when you have Type 2 diabetes?

 Yahoo News
Yahoo News 
