How the power of art can help scientists like me understand the experience of schizophrenia
People with schizophrenia can experience psychosis, a condition in which they perceive the world very differently to those around them. They may see or hear things that others cannot or hold beliefs that others find bizarre. These experiences can be distressing for those experiencing them, as well as for their families and friends. Current treatments are inadequate: they do not work for all and can lead to unpleasant side effects. But attempts to improve this are hampered by our limited understanding of schizophrenia’s biological basis.
There is no single factor that causes schizophrenia, but we know that genes are important. But neither is there a “schizophrenia gene”. Instead, many hundreds of genes act in concert to subtly increase or decrease how likely we are to become ill, given the environment in which we find ourselves.
In the last ten years, geneticists have begun to uncover the specifics of these complex relationships by identifying precisely which genes are linked with schizophrenia and other mental health conditions. For neurobiologists like me, the discovery of these genes is exciting. This information provides new clues as to which molecules and cell signalling pathways might be altered in these conditions.
From genes to experience
But identifying genes is very much the beginning of a long journey to better understand mental health conditions. Genes don’t directly encode hallucinations, alterations in perception or any of the other complex, subjective states that those with schizophrenia experience. It is therefore essential that scientists, like me, acknowledge these complexities and seek to understand the unique experiences of individuals with schizophrenia.

The challenge, then, is to understand how the function of these genes is altered in schizophrenia, how this influences brain function and, ultimately, how this leads to each person’s subjective experience. Understanding these complex relationships requires collaboration between individuals with lots of different types of expertise, not least those with direct experience of schizophrenia. But since psychiatric genetics has historically been misunderstood and misused, it is crucial that the aims of this research and, even more critically, its limits are clear.
It can be challenging to have meaningful conversations about genetics, the biological basis of mental health conditions and subjective experience, since such conversations require a respectful and trusting environment in which all participants are equal. Art can play a vital role in promoting such an environment. It can help to communicate complex ideas and distinct viewpoints in new ways.
Switching perceptions
This is why over the past three years I have collaborated with Eleanor Minney, an artist with an interest in mental health and subjective experience, and how these relate to genetics. Together, we have worked with people on one of the wards of the National Psychosis Unit (NPU), in a series of workshops.
We used art to explore these relationships and to discuss these often complex and emotive subjects and the participants’ diverse opinions and experiences. Some of the people we worked with were keen to chat about their experiences, while others expressed themselves through the art they created. Eleanor’s textile artwork “Segment of aself”, for example, inspired by conversations with participants, represents genetic information on one side as regimented “switches” while the other side is peppered with hieroglyphic-like symbols that represent all the different facets of an individual life. These two sides are joined with wadding, representing the complex biological processes linking the two, which is where my research is situated.
The value of dialogue about the intersection between biology and mental health was succinctly articulated by one of the workshop participants, who came up with the idea of the “Think Tank”: a forum for interested people (scientists, patients, carers, clinical care team, the wider public) to discuss the biological bases of mental health conditions, and their relationship to subjective experience and clinical care, in an open, pragmatic and constructive manner.
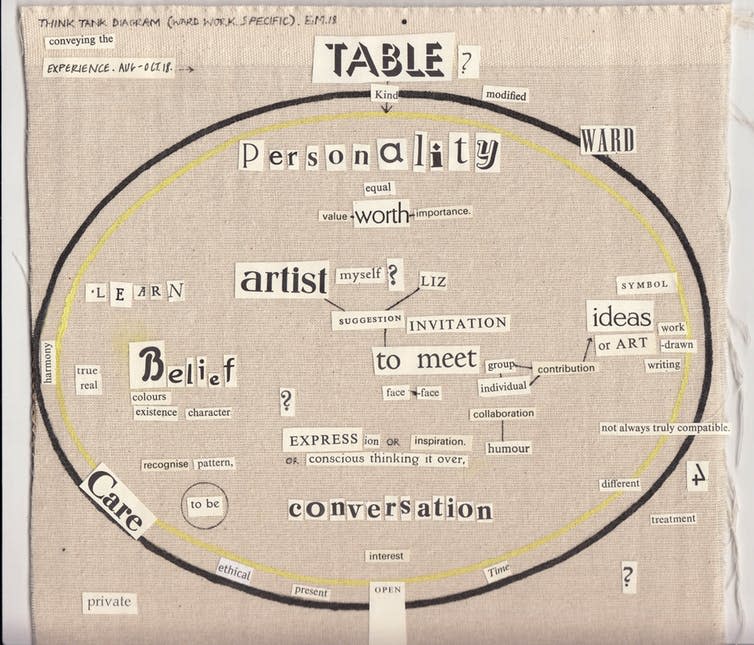
The workshops culminated in an art exhibition – Switching Perceptions – hosted by the Bethlem Gallery, and featuring pieces created both by Eleanor and by those engaged in the workshops. Elements of this exhibition are now open in London’s Barbican Centre, encouraging more discussions with more people. We hope that participants from all walks of life can come together to discuss mental health conditions and their relationship to our biological make-up and sense of self. We want to facilitate these conversations with as many people as possible.
This evolving project has shown me the profound power of art to facilitate respectful and meaningful conversations in the complex area of mental health. I have learnt an enormous amount from the participants, and I believe that all those involved valued the forum to discuss science, personal experiences and their intersection.
On a personal level, I have also found that working with Eleanor has opened my eyes to the relevance of the artistic process to science: I have begun to use abstract, artistic approaches to synthesise my understanding of the scientific literature and to generate new ideas.
This article is republished from The Conversation under a Creative Commons license. Read the original article.

Elizabeth Tunbridge receives funding from the Medical Research Council and an Unrestricted Educational Grant from J&J Innovations. Switching Perceptions is funded by the Royal Society and the University of Oxford, with support from the Bethlem Gallery. It was awarded a University of Oxford Vice Chancellor’s Public Engagement with Research Award 2019.

 Yahoo News
Yahoo News 
