Stress led to more NHS staff absences than Covid, new figures show

“Burnout” and stress among doctors, nurses, paramedics and other health staff has cost the NHS in England more than 15m lost working days since March 2020, about 50% more than the days lost to Covid infections and self-isolation, analysis of official figures by the Observer reveals.
NHS sickness figures show that between March 2020, the month of the first Covid lockdown, and last September, 15.4m working days have been lost in the NHS because of stress-related absences, compared with 9.8m days lost from staff who were required to self-isolate or were ill with Covid.
Related: ‘It’s soul destroying’: why so many NHS staff are off sick with burnout
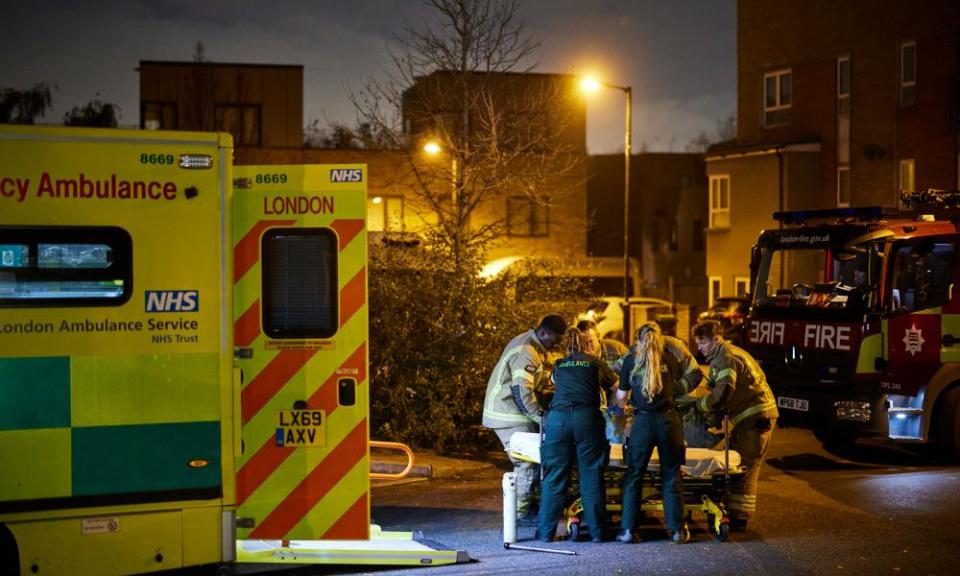
Staff who have spoken to the Observer warn an exhausted and demoralised workforce is increasing the risk of errors in patient care. Some of the workers with the highest rates of sickness from stress are ambulance staff who are routinely delayed getting to urgent calls because of long waits to hand over patients at hospitals.
Daisy Cooper, the Liberal Democrats’ spokesperson for health and social care, said: “These figures are a staggering reminder of the pressures NHS staff are under. When dedicated workers are pushed to the brink, it not only severely impacts their wellbeing, but also increases the risk of mistakes being made. No one should have to work when they are exhausted.
“The shortage of healthcare workers, combined with the immense pressure they are under, is a recipe for disaster.”
The scale of the mental health toll staff are under is revealed as nurses in the Royal College of Nursing prepare to strike on Monday and Tuesday. Ambulance workers will also join nurses in taking strike action.
The NHS Confederation, the membership organisation for the NHS in England, Wales and Northern Ireland, estimates that recent strikes have led to about 88,000 operations and outpatient appointments being cancelled.
NHS sickness absence rates showed that in most of the months that staff were battling the pandemic, stress, anxiety and other mental health illnesses accounted for more lost days of work than staff who had Covid or were self-isolating.
New figures from the BMA’s latest survey of junior doctors in England show that more than three-quarters of respondents (78%) felt unwell as a result of work-related stress in the past year. Most junior doctors (81%) who took part in the survey reported that their health and wellbeing has worsened, or not improved, since December 2021.
Dr Vivek Trivedi, the co-chair of the BMA junior doctors committee, said: “It is a huge risk to patient safety for doctors to work under pressure while feeling exhausted, burnt out, and often suffering with poor mental health.
“They want to feel as if they are doing the best job possible, the job they trained to do, but the constraints of working in the NHS means many feel they cannot give the level of care they would like to patients as in many cases there simply is not the staff to deal with demand.”
Another survey of members of the Royal College of Radiologists (RCR) found that half were considering reducing working hours and nearly a third (31%) are considering leaving the NHS to work elsewhere.
Dr Tom Roques, a clinical oncologist and vice-president of the RCR, said: “It’s a vicious circle because the more people that go off with stress, the fewer people are left to do the work. People are more demoralised because it’s hard to see the light at the end of the tunnel.”
Some ambulance trusts have reported absence rates of more than one in 10 staff during the pandemic. The overall sickness absence rate for the NHS in England was 5% in September 2022, which are the most recent figures available. Freedom of information requests by the Liberal Democrats show that, in 2022 alone, ambulance trust staff have taken off more than 154,000 days due to poor mental health.
An NHS spokesperson said: “The NHS locally and nationally has taken significant steps to support all our staff as they deal with record levels of pressure across our services, so that they can provide the best possible care for patients.
“These include putting in place regular health and wellbeing conversations, providing a range of health and wellbeing support, supporting flexible working, and making resources available to support staff with the cost of living.”

 Yahoo News
Yahoo News 
