Voices: My brain injury and me: How one moment changed my life
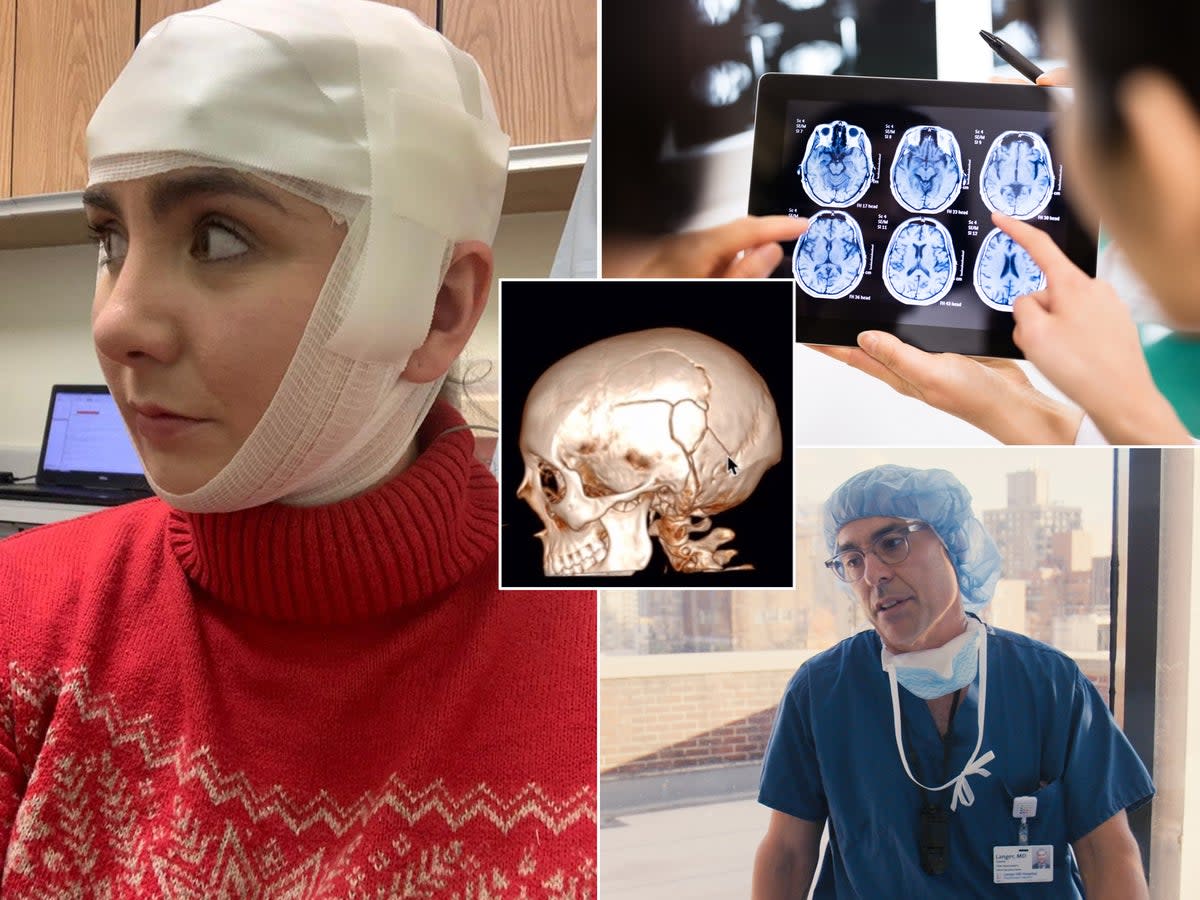
I woke up to a crowd of people trying to force my limp body into a machine. A burning feeling in my throat told me I was about to vomit up blood. Despite me repeatedly warning the nurses and doctors what was about to happen, they didn’t listen and whirred me into what I assume was a CT or MRI machine — the inside of which I instantly decorated. Before slipping out of consciousness again, I realized by their surprised faces they hadn’t understood a thing I said.
It’s a sensation you can’t put your finger on; constantly out of reach like a lucid dream or deja vu. You’re pretty sure you know what’s good or bad, up or down, yes or no, but all are shrouded in such a thick mist that you can’t help but doubt yourself. It’s invisible, volatile, confusing, and painful. At least that’s the closest I can get to describing my experience of having a traumatic brain injury. Like a shitty snowflake, it will be different for everyone.
It’s still unclear how I got the fractured skull and brain injury that led me to experience this. I was riding an e-bike before being found face-down in a road in Queens in a comatose state. Someone had called an ambulance to come help a dead-looking woman covered in blood. Yes, I was not wearing a helmet; you’re more than welcome to lambast me in the comments, but I think this article will prove I’m suffering enough for my lapse in judgment.
I was transported to the hospital and a team of health care professionals worked urgently to save my life, cutting and bandaging and ferrying and consoling. Eventually, I came to just long enough to wave at my friends — who had been contacted once the hospital worked out I was an expat with no family in the country — and point at my chipped tooth.
The first few weeks of recovery were horrific. I had constant pain and confusion, and the tests were relentless, but initially my progress was fast. Within days, I was conscious and could slowly walk. Within weeks, I could speak clearly and exercise gently. Within months, I could return to work and resume a lot of “normal life” activities. However, as I creep towards the one-year anniversary of the accident, I find myself facing new and terrifying hurdles.
Traumatic brain injuries, or TBIs, are not rare; in fact, after I acquired one, I was alarmed to find out just how common they are. “Globally, the annual incidence of traumatic brain injury (TBI) is variably estimated at 27 to 69 million,” Dr Shae Datta, co-director of NYU Langone’s Concussion Center, tells The Independent. That means approximately 2.5 million people in the US every year. There are more than 5.3 million individuals in the States living with a permanent brain injury-related disability, or one in every 60 people.
Given my initially speedy progress, I thought I’d had a lucky escape. I presumed I’d be back to myself within a year and normal life would resume in its entirety. This would turn out to not be the case. Neurologist Dr Daniel Miguel Torres, who has been tirelessly treating me over the last nine months, says the most common long-term issues he sees patients dealing with after a TBI are “headaches, nervous system oversensitivity, emotional problems, cognitive problems and dizziness.” Speaking about my personal experience, he says: “I think you have had to deal with most of the different problems that can be caused by an injury like this. That makes your injury more severe than the average brain injury.” What an over-achiever I am.
As the weeks roll on, different issues bubble to the surface. In addition to those more common difficulties such as headaches, fatigue and sadness, I have had some more unusual symptoms. Recently, I have intermittently experienced a strange sensation in the middle of a conversation, where I’m talking, but I feel like I’ve stopped making sense. I might as well be speaking French for all I can tell; however, those around me insist everything I am saying is completely normal. Then there are the couple times I started hearing voices before passing out. During one of those episodes, I hit my head falling to the floor and ended up straight back in the ER.
Dr David Langer, chair of neurosurgery at Lenox Hill Hospital and star of Netflix’s Lenox Hill, experienced a TBI himself due to a ski accident last year. He doesn’t remember the incident or the days following. In fact, at first — despite being a world-renowned neurosurgeon — he didn’t even realize he had a TBI at all. “I think it’s hard to go into the chair of neurosurgery’s room and say, ‘Hey, you know, we think you had a TBI,’” he says. “When [my doctor] told me, I thought there’s no way, I didn’t even hit my head.” He then came to realize he didn’t actually remember the accident: “I’ve even seen videos of me during the post-op having a conversation that I don’t have any recollection of.”
Dr Langer’s background allowed him to be realistic about his TBI and what recovery would look like: “I feel completely myself. I think neuropsychologically, I’ve never felt better … but I am more reflective on my mortality … I’m not glad it happened, but I can certainly manage it and my own expectations of myself, which is half the battle.”
There are millions of people living with permanent brain injury-related disabilities, but that doesn’t necessarily mean others know it. From the outside, I appear normal and healthy; however, I’m accutely aware I’m not, at least not yet. The invisibility of my condition makes it difficult to convey to people around me that I still need extra consideration when I’m out and about. Until recently I would arm myself with a cane when in particularly busy settings, not because I needed it for walking but because I may require a seat on a train, or would need people on the street to give my still-healing skull a wide berth. The cane served as an easy physical reminder to people that I’m not as well as I might look.
Another issue that a lot of people with TBIs experience is chronic pain, sometimes brought on by what’s known as post-concussion syndrome. That’s something I know all too well. And being in pain for long periods of time can change the way your brain reacts to it, Dr Torres explains. “All chronic pain should be managed through what is called the ‘bio-psycho-social’ model of pain management. It is important that patients engage in the psychological aspects of pain management, whether or not they think psychological factors contribute to their condition.” Where brain injuries are concerned, psychology and biology go hand-in-hand.
As someone with an ironclad personal support system, I often reflect on what life must be like for those with injuries like mine who aren’t as privileged. On top of good health care, a huge part of recovery is having family and friends who will keep on rooting for you. “If someone develops persistent post-concussion syndrome, they often have to cut down on work and social activities and thus do not enjoy life the way others do. This leads to loss of financial wealth and ability to achieve many things in their life,” Dr Datta says. “The most extreme are patients with emotional dysregulation or post-injury movement disorders or mood disorders that need to be treated with a variety of modalities.”
I feel a TBI and fractured skull can be compared to smashing an egg. No matter how many times you try, you would never be able to break an egg in exactly the same way twice. You can’t put it back together in the same way it used to be, either. Everyone will have different genetics, different specifics to their type of injury, different lives and jobs and different levels of psychological resilience. Dr Langer says: “Two people who have exactly the same TBI don’t always end up the same after. Not to mention each person’s intrinsic brain and the differences in bone of the skull and the weight of the brain and all the rotational forces, there are all sorts of different things that can affect the actual injury and the outcomes.”
There are a myriad of factors making the studying of this field incredibly difficult: “Only a minority people have a neuro-psychological profile measurable before and after, who’ve actually had a neuro-psych test ahead of time and then have one afterwards ... I think the reason why there’s not a lot of good data on this is because it’s really hard to design good studies where there are no baselines. We don’t know where people are ahead of time. And there’s a huge neuropsychological component to this: anxiety, depression, fear, PTSD.” If you never knew the person before they hit their head, how can you make meaningful and objective comparisons to their lives after?
It may be the case that no two TBIs are the same, but “that doesn’t mean there can’t be better solutions,” Dr Langer says. “The NFL can’t even solve the problem they have. They’ve spent hundreds of millions of dollars on this and they’re no better off now than they were. All they do is change the rules … Even the military hasn’t done a great job of managing people with traumatic brain injury, which is even more striking.”
Opening my head opened Pandora’s box. Out flew not only months of health issues, but the jarring realization that so many people in the world are living like me. If one in every 60 people have a disability brought on by a brain injury, why is it only when an NFL athlete collapses on the field that we give it due attention?
“There’s an element of risk that we take as humans and we go back to our lives. I feel like I had to show people what I was capable of doing … and prove that I was not any less than I was before,” says Dr Langer, of his own TBI and recovery period. “But I can tell you this has made me become more calm. I felt enlightened for a while afterwards in that post-injury period. I had this near-death kind of emotion that I’ve carried with me that definitely made me aware of the end of life and your own vulnerability.”
Gesturing to his head, Dr Langer adds: “Your happiness is right up here. It’s nowhere else. It’s your own perceptions. And so it’s up to you. If you need to have a feeling, then that should be expressed … It’s important to be honest and show vulnerability, show what’s really going on. Because I think that’ll release some of the stuff inside that might be holding you back in the first place”.
He finishes with a piece of advice I try to adhere to myself: “No guilt or shame. F*** that.” I will of course add to this advice, and say: always wear a helmet.

 Yahoo News
Yahoo News 
