Coronavirus: who were the first 775 critically-ill patients in the UK?

Information has been released on the first 775 patients in the UK who became critically ill with the coronavirus.
Early research suggests four out of five cases are mild, with a relatively small number of patients becoming seriously unwell with pneumonia.
Nevertheless, with the virus virtually unheard of just three months ago, how it affects different ages, sexes and underlying health issues is somewhat of a mystery.
To learn more, the non-profit organisation Intensive Care National Audit & Research Centre (ICNARC) looked at all 775 patients in critical-care units who were reported up to 26 March.
Experts have stressed this limited pool of patients will unlikely be representative of the overall number of coronavirus-positive people.
Nevertheless, one called the report “stunningly important” in the fight against the pandemic.

The coronavirus is thought to have emerged at a seafood and live animal market in the Chinese city Wuhan, capital of Hubei province, at the end of last year.
Since the outbreak was identified, over 724,200 cases have been confirmed across more than 170 countries on every inhabited continent, according to John Hopkins University.
More than 152,000 patients are reported to have “recovered”.
Latest coronavirus news, updates and advice
Live: Follow all the latest updates from the UK and around the world
Fact-checker: The number of COVID-19 cases in your local area
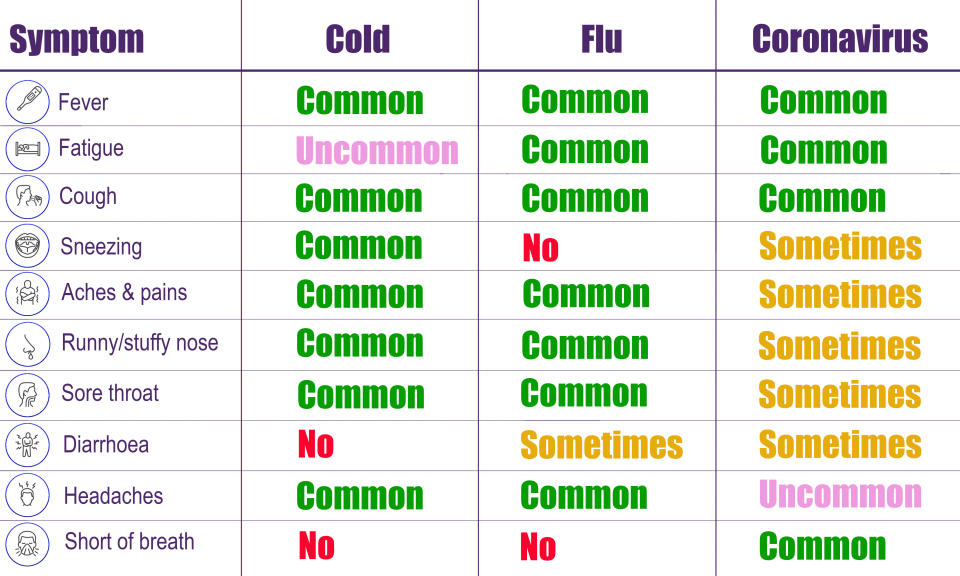
Explained: Symptoms, latest advice and how it compares to the flu
Cases have been plateauing in China since the end of February, with the US and Europe now considered the worst-hit areas.
The UK has had more than 19,700 confirmed cases and 1,228 deaths.
Globally, the death toll has exceeded 34,000.
Coronavirus: what we know of the UK patients so far
Of the 775 patients, 86 had been discharged from critical care at the time of the report’s publication and 79 had died.
These patients were compared against those who were critically ill with viral pneumonia, not coronavirus-related, in 2017-to-19.
The coronavirus is an infection of the airways. In severe cases, it can lead to pneumonia.
This occurs when the infection spreads to the air sacs in the lungs, causing them to become inflamed and filled with fluid or pus.
The lungs then struggle to draw in air, resulting in reduced oxygen in the bloodstream and a build-up of carbon dioxide.
Based on the ICNARC data, the coronavirus patients had an average age of 60 at admission, compared to 58 for those with non-coronavirus viral pneumonia.
Less than a third (29%) of the coronavirus patients were female, versus 45% of the viral-pneumonia sufferers.
Coronavirus deaths have been reported as disproportionately affecting men, which many experts put down to males being more likely to smoke in “hotspot” areas like China and Italy.
When it comes to BMI, most of the coronavirus patients (34%) fell into the overweight category, while most non-coronavirus related sufferers were a healthy weight (nearly 34%).

Nine out of 10 (90%) of the coronavirus patients were “able to live without assistance in daily activities”, compared to around three quarters (73%) of the other pneumonia sufferers.
Just one of the 775 patients (0.1%) admitted with the coronavirus required “total assistance with all daily activities”, versus 2.4% of those with non-related viral pneumonia.
When it came to pre-existing health issues, a suppressed immune system affected 3% of the coronavirus patients, compared to nearly 9% of the other pneumonia sufferers.
“Immunocompromise” was defined as undergoing chemo, radiotherapy or a daily high-dose steroid treatment in the past six months.
Blood cancers were the next most common comorbidity, affecting 1% of those with the coronavirus and 4% of the patients with another form of viral pneumonia.
More than three quarters (78%) of the coronavirus patients had to be mechanically ventilated in the first 24 hours of admission to critical care, compared to less than half (43%) of those with viral pneumonia.
Based on the data available, it appears around half (47%) of the coronavirus patients died.
It is important to remember, however, this only includes information on those who were “discharged from critical care or who died in critical care” at the time of the report’s publication.
“To say the mortality rate of ICU patients is 50% is misleading and may induce panic,” said Dr Tim Crocker-Buqué from the London School of Hygiene & Tropical Medicine.
“More accurately, it shows of the 21% of those patients who have left critical care, 48% of them had died.
“However, it excludes the 79% patients who do not have an outcome yet.”
The coronavirus’ death rate has been up for debate.
The World Health Organization previously reported a 3.4% fatality rate globally, however, scientists from the University of Hong Kong later put it at 1.4%.
The deceased in the ICNARC study spent on average three days in critical care, compared to the four days before the “survivors” were sent home.
“Of note, these are very early data, so the patients who have already died have had very short stays in critical care, suggesting they may have deteriorated much quicker than other patients and so are unlikely to be representative, and may be reflecting a higher risk of death in this early group that died”, said Dr Crocker-Buqué.
Sir David Spiegelhalter from the University of Cambridge agreed, adding: “Those discharged already, whether dead or alive, presumably comprised the most and least sick, and it remains to be seen what happens to the intermediate group still in intensive care.”
Overall, the scientists welcomed the data.
“The value of this report is it gives a good indication of the likely needs for critical care as the epidemic progresses,” said Professor Paul Hunter from the University of East Anglia.
“It also gives a good indication of those who are likely to do well and those who are likely to do poorly on critical care.
“Sadly such information may become crucial if social distancing is insufficient to reduce the size of the peak and demand for critical-care beds outstrips availability over the coming months.
“What this report does not do is give an indication of the outcomes for people who are not considered for a critical care bed or cannot access one and we need data to be collected and reported on all patients.”
Professor Sheila Bird from the University of Cambridge described the report as “stunningly important”, “timely” and “insightful”.
“Soon, the authors may be able to report separately on the seven-day and 14-day post-admission status for [coronavirus] admissions who have reached these [clinical] landmarks and to offer the corresponding results at these landmarks for their 2017-to-19 comparator group”, she added.
What is the coronavirus?
The coronavirus mainly spreads face-to-face via infected droplets coughed or sneezed out by a patient.
There is also evidence it can be transmitted in faeces and urine and survive on surfaces.
Symptoms tend to be flu-like, including fever, cough and slight breathlessness.
The coronavirus has no “set” treatment, with most patients naturally fighting off the infection.
Those requiring hospitalisation are offered “supportive care”, like ventilation, while their immune system gets to work.
Officials urge people ward off the infection by washing their hands regularly and maintaining social distancing.

 Yahoo News
Yahoo News 


